Dr. Phil Zeltzman’s Blog
When should my pet’s tumor be removed?

As much as I enjoy a challenge, I would rather remove a small tumor than a big one.
There are at least 15 reasons for that:
1. A smaller mass means a less invasive surgery
2. A smaller mass means a shorter incision
3. A smaller mass means a shorter anesthesia
4. A smaller mass means a less expensive surgery
5. A smaller cancerous mass usually means fewer chances of spreading to other organs
6. A smaller mass means fewer chances of rupturing/bleeding/infection

7. A smaller mass means fewer complications related to surgery (fluid build-up, failure of the stitches, etc.)
8. A smaller mass means fewer complications related to the tumor (increased calcium levels, decreased sugar (glucose) levels, seizures etc.)
9. A smaller bone tumor means fewer chances of a fracture
10. A smaller tumor means fewer chances of losing a body part (leg, tail, eye)
11. A smaller tumor means less pain before AND after surgery
12. A smaller tumor means fewer chances of a life-threatening emergency (e.g. inability to pee or breathe)
13. A smaller mass may mean a shorter recovery
14. A smaller mass usually means a better outcome
15. A smaller mass removal means a safer surgery

This was a cancerous mass (fibrosarcoma) in a 12 year old pitbull
Although some of the above reasons may seem obvious, we regularly remove large tumors.
We can still help these patients.
Sometimes the outcome is still good, and sometimes it’s much worse than it could have been…
Also please don’t fall into the trap of assuming:
- It’s just a fatty tumor
- It’s just a cyst
- It’s just a polyp
NOBODY can say for sure what a mass is by simply looking at it or feeling it. Only a biopsy can.
Anything else is an assumption, or an educated guess at best.
So for your pet’s sake, schedule a consult with your family vet or a board-certified surgeon as soon as you notice a mass, a lump, or a bump, anywhere in the body.
Better safe than sorry…
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified
Pete Baia, DVM, MS, DACVS

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How Fecchi’s Owner Twisted My Arm

NOTE: This is a free excerpt from my upcoming book about cancer in pets!
Fecchi, an 8-year-old Sheltie, had a firm, golf ball-sized mass in his left cheek. It was hard to be more specific since I couldn’t even open his jaw during the exam.

Note: I have pictures of the entire surgery, but I decided some were too graphic. So I will only show a few relatively “tame” pictures.
Upon further exam, it looked like the mass was coming from the upper jaw (maxilla) and/or the the lower jaw (mandible).
Clearly, a major reconstructive and possibly disfiguring surgery was necessary to remove the mass.
Fecchi’s owner had consulted with 3 surgery colleagues, who all had told her that this mass was some horrible cancer that couldn’t be removed.
Given the poor outcome and Fecchi’s lack of appetite, they all told her she should humanely put him to sleep. Yet that option wasn’t good enough for this client.
And that’s when we met. During the surgery consultation, she insisted on removing the mass.
I wasn’t so sure it was in the patient’s best interest.

Fecchi had lost weight and wasn’t in very good health because of the tumor.
So we compromised and agreed on taking a biopsy first. A week later, the biopsy came back as osteo-chondroma – a benign tumor of both bone and cartilage.
Of course, I didn’t believe it. More convinced than ever about her decision, the owner insisted on removing the mass.
After a lot of soul-searching, I finally gave in. I accepted to “explore the area and see what I could do to help.”
Granted, removing jaw tumors is not an uncommon procedure. So why the hesitation?
After all, with the numerous pain management modalities available, we can make these patients comfortable despite aggressive surgery.
Anyway, we ended up taking Fecchi to surgery.
It turned out that the mass came from the upper jaw, but on both sides of the jaw.
As the tumor grew bigger and bigger, the teeth of the lower jaw dug sort of a “gutter” into it.
Surgery was long and challenging. It was followed by reconstruction of the surgery site to make it look as cosmetic as possible.
To make sure Fecchi would get enough nutrition after surgery, we placed a feeding tube to inject a special liquid diet directly into the stomach (see the red tube coming out of the skin).

The entire mass was submitted to the lab.

Fecchi recovered smoothly from anesthesia.
He stayed in ICU overnight, on IV fluids, pain medications, and antibiotics.
10 days later, the biopsy report came back. As you can imagine, it concluded… osteochondroma – still a benign tumor!
So what’s the moral of the story?
Fecchi’s owner kind of twisted my arm – in a nice way – and she was totally right.
Should we always do what clients require?
Of course not.
Otherwise, we would do ear crops, declaws, and tail docks all day long.
What’s the moral of the story? It is perfectly acceptable to perform a procedure, invasive or not, as long as client and practitioner are on the same page, and the procedure is acceptable and ethical.
Sometimes, it’s good to be pushed out of one’s comfort zone.
Almost one year later, Fecchi was reportedly doing great at home.
“The surgical site looks great,” the owner says. “You can’t even tell that he ever had surgery.”
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How Toast recovered after deranged knee surgery

Toast, a 4-year-old kitty, was sleeping on the couch when he was suddenly woken up by a porcelain vase that fell and broke into a million pieces. Spooked, he jumped from the couch and hid in another room.

Later that evening, the owner found his poor kitty crying out in pain and unable to use the left back leg.
The next day, he took Toast to his family vet. An exam revealed severe pain in the left knee. X-rays under sedation showed pretty drastic findings.
After reviewing the X-rays, I realized that the knee was completely dislocated (luxated). This is called a “deranged knee.”

I suspected that Toast’s leg got caught during the escape from the couch and the evil vase. While Toast was running for his life, he pulled on the leg, and that presumably caused the damage.

What’s a deranged knee?
Toast’s owner asked what this condition with a weird name was about. I explained that there are four ligaments in the knee: two inside the knee (anterior and posterior cruciate ligaments) and two outside the knee (collateral ligaments). When more than one ligament is torn, the knee is so severely affected, that the condition is called a deranged knee.
Most of the time, both cruciate ligaments and one collateral are torn. Occasionally, with very violent trauma, all four ligaments are torn.
How is a deranged knee treated?
A deranged knee is so unstable (wobbly) that the only hope for a good recovery is surgery. The goal is to make the knee more stable. Post-op care involves a combination of strict rest, pain medications and physical therapy.
During surgery, I confirmed that Toast had 3 torn ligaments (one collateral and both cruciate ligaments). They were repaired with heavy nylon sutures to mimic or imitate the original ligaments.
Toast recovered smoothly from anesthesia and went home the day after surgery.
Recovering from a deranged knee
After 2 weeks of strict confinement and physical therapy, Toast had his stitches removed. At that point he was “toe-touching,” which means that he was starting to put gentle pressure on the foot. After another 6 weeks of continued rest and physical therapy, he had another follow-up exam: he was using the leg very well.
It was time to progressively increase his activity level. We designed a program to help him rebuild muscle and regain flexibility in the surgery knee. By using toys and food, Toast’s owner managed to convince him to follow him around.
Long-term outcome of a deranged knee
Although patients can do well after surgery to repair a deranged knee, they will get arthritis.
We managed Toast’s arthritis by maintaining a healthy weight, and giving joint supplements (aka arthritis supplements) such as glucosamine and fish oil (omega 3 fatty acids) – for life.
In the end, Toast’s owner was happy with the outcome, and promised not to break fragile objects anymore!
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified
Pete Baia, DVM, MS, DACVS

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What questions should you ask your pet’s surgeon?

Trusting your vet or a surgeon with doing surgery on your beloved pet is not as easy as it sounds.
It requires a lot of trust.
To help you establish that trust, here are some questions I feel are reasonable to ask your vet or your surgeon.
- Are you a board-certified surgeon, i.e. a true specialist?
- What’s my pet’s exact diagnosis?
- What are ALL of the treatment options?
- What is the specific surgery you recommend?
- What is the purpose of the surgery?
- Why do you think this surgery is a better option than the other ones?
- Is my pet a good candidate for this surgery?
- Who is the best person to do the surgery?
- How many of these surgeries have you done in your career?
- How many of them have you done in the last year?
- What are the possible risks and complications?
- How common are they in general?
- How common are they in your patients, in your hands?
- What is your success rate?
- Are there additional tests required before surgery?
- How will my pet be monitored during and especially after surgery?
- How long will the surgery take, and how long will my pet need to stay at the clinic?
- If there is an overnight stay, who will supervise my pet?
- How will pain be assessed and addressed?
- What is the expected recovery like?
- How long will it take for my pet to fully recover?
- What are the postop care instructions and restrictions?

Even though this list looks long, and seems like it would take hours to answer, a good surgeon should answer many of these questions during the consultation anyway.
So check those questions off as they go, and ask the remaining questions after that.
It’s critical to have open and transparent communication with your surgeon to ensure you make an informed decision about your pet’s surgery.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How can I tell my pet has cancer?

NOTE: This is a free excerpt from my upcoming book about cancer in pets!
Many pet owners think we can diagnose cancer by looking at routine blood work, when that is very rare.
Exceptions include liver and thyroid cancer.
So how might you suspect your pet has cancer?
Here are 7 findings that should put you on alert.
1. Skin mass
The most common type of mass is directly visible on or under the skin. Sometimes, the mass can burst open and bleed, or ooze.
Don’t make the classic mistake of thinking “It’s just a cyst” or “It’s just a fatty tumor.”
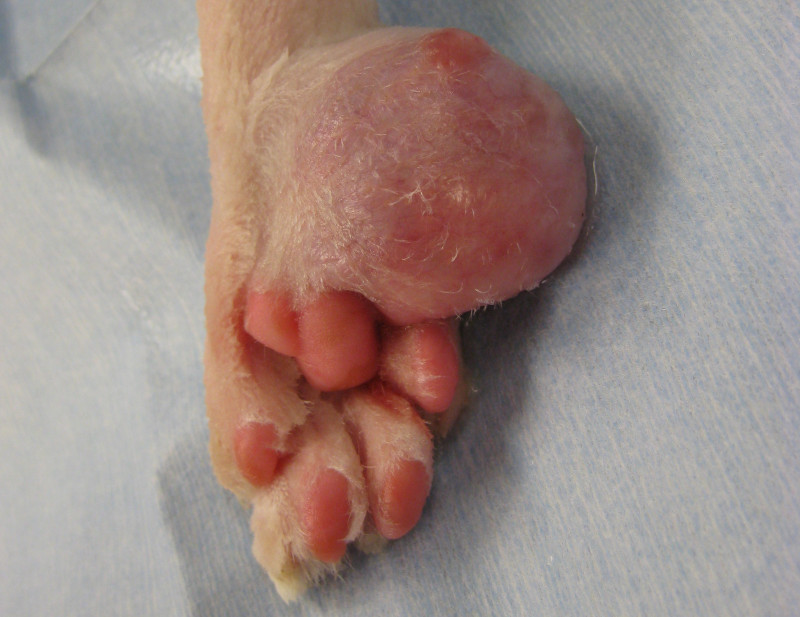
Never procrastinate in those situations. Early intervention can make the difference between success and failure. Removing a small mass is understandably less invasive and cheaper than removing a big mass.
In some cases, removal of a mass has become impossible and the best option is to amputate a leg.
2. A big belly
Of course not every cat or dog with a big belly has cancer!
Rather, it’s about a belly that becomes big quickly.
That can be a sign that a mass has grown inside an organ (for example the spleen).
Occasionally, such a mass can rupture and cause internal bleeding, which can also cause a big belly.
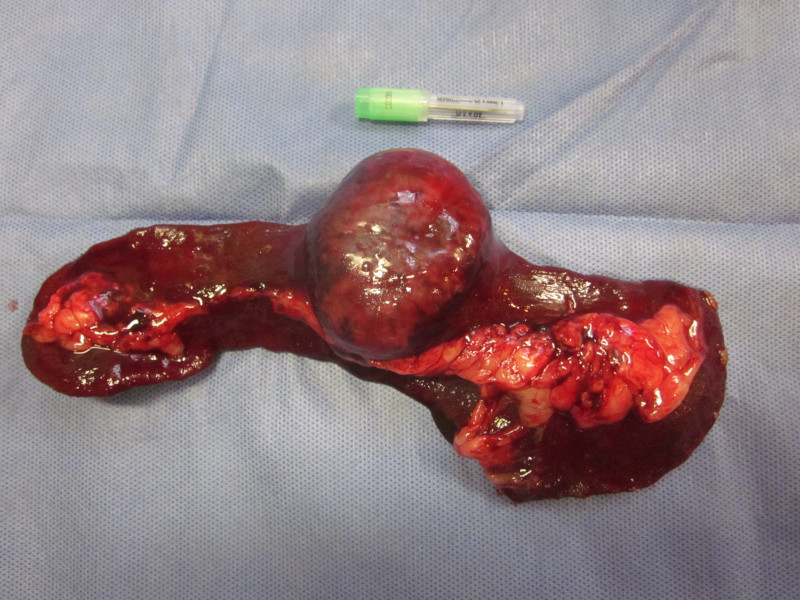
3. Unexplained weight loss or gain
A mass in the spleen can weigh several pounds, so it would make sense that the pet would gain weight despite having the same appetite.
In other cases, it’s the other way around. Cancer can cause weight loss.
Why? Because cancer cells need specific nutrients to grow and thrive, so they rob them from the patient.
4. Bleeding
Bleeding from anywhere in the body should be a cause for concern – and a veterinary consultation.
- Bleeding from a mass or a wound as mentioned above.
- Bleeding from the mouth, the ear, the bladder, or the rectum.
- Internal bleeding, causing an enlarged belly as mentioned above, which may be difficult to tell.
5. Difficulty breathing, eating, walking
Any mass can affect a body part, and its function.
A mass in the throat can cause difficulty breathing.
A mass in the jaw, the gum, or around the tongue can cause pain and difficulty eating.
A mass in a leg or the armpit can cause difficulty walking.
6. Stubborn vomiting or diarrhea
Tumors in the stomach or the intestines can cause vomiting or diarrhea.
They typically don’t stop after the usual treatments provided by your family vet.
As they grow, these tumors affect the lining or the thickness of the stomach or the intestines, which can affect the way they work.
This can cause bleeding, so vomit or poop/diarrhea can contain blood, either red (“fresh”) or blackish (“digested”).
Sometimes, a mass grows so big, that it can cause a blockage of the stomach or the intestines.
7. Something just doesn’t make sense
A bladder infection that keeps coming back despite multiple rounds of antibiotics may very well be masking a bladder tumor.
And then sometimes, my experience shows that when something just doesn’t make any sense, or defies a logical explanation, cancer should be considered as a possibility.
If you ever notice any of the signs above, please get an appointment with your family ASAP.
If cancer is suspected, time is of the essence.
The sooner we intervene, the better off your pet will be.
Procrastination never helps.
Quite the opposite. Procrastination may mean there is no hope to help your pet.
So the sooner you act, the better it will be for your pet.
If you would like to learn how we can help your pet with safe cancer surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

