Dr. Phil Zeltzman’s Blog
THE TRUTH ABOUT CANCER IN DOGS AND CATS: 10 COMMON MYTHS EVERY PET OWNER SHOULD KNOW ABOUT

When your veterinarian or your surgeon says the words “cancer in your pet,” time seems to stop.
Your mind races.
You’ve heard horror stories.
You think of a family member.
You wonder if treatment is truly worth it.
You worry about your pet’s quality of life.
As veterinary surgeons who have treated thousands of dogs and cats with cancer, we’ve seen firsthand how misconceptions and myths can prevent pets from getting life-saving or life-extending treatment.
Let’s clear up some of the most common myths so you can make informed decisions for your pet.
A week doesn’t go by without a conversation with a pet lover who fell into one of those traps…
Please don’t be one of them!
PET CANCER MYTH #1: A cancer diagnosis means my pet will die soon
The Reality: Not all cancers are the same, and many are highly treatable – even curable.
Just like in human medicine, “cancer” is an umbrella term for hundreds of different diseases.
Yes, some cancers are aggressive and fast-spreading.
Others are slow-growing and localized.
Some can be completely cured with surgery alone.
The key is getting an accurate and early pet cancer diagnosis.
A lump that’s been there for months or years isn’t necessarily “just a fatty tumor.”
Any new lump or growth on your dog or cat, or any growth that’s changing, should be evaluated by your family vet or a surgeon.
PET CANCER MYTH #2: Surgery will just spread the cancer
The Reality: This is one of the most harmful myths, and it’s simply not true.
We hear this constantly: “My neighbor’s dog had surgery and the cancer spread everywhere.”
Let’s be clear: cancer surgery in dogs and cats does not cause cancer to spread (when done properly of course).
What actually happens is this: sometimes when we remove a tumor surgically, it is impossible to prove spreading (aka metastasis) before surgery, because it was too small to detect at that time.
The surgery didn’t cause the spreading.
It was already there, but we could not prove it.
For many cancers, surgery is the only chance for a cure.
Removing a tumor completely before it has a chance to spread can save your pet’s life.
The goal of cancer surgery is to achieve “clean margins” – i.e. removing the tumor along with a rim of healthy tissue around it to ensure we got all the cancer cells.
Sometimes this means removing more tissue than you might expect, but that’s because we want to give your pet the best possible outcome.
PET CANCER MYTH #3: My pet is too old for cancer surgery
The Reality: Age is not a disease.
What matters is overall health, not the numbers on the calendar.
We’ve performed cancer surgeries on 14, 15 and 16-year-old pets who recovered beautifully, and we’ve recommended against surgery for 6-year-old dogs with cancer that was ignored for too long.
It’s not about age—it’s about:
- Overall health status
- Heart and lung function
- Kidney and liver function
- Ability to handle anesthesia
- Expected quality of life after surgery
Modern veterinary anesthesia is incredibly safe for dogs and cats.
We tailor anesthetic protocols to each individual patient, and we monitor pets constantly during surgery (heart rate, blood pressure, oxygen levels, temperature, CO2, and more).
Don’t let age alone prevent you from exploring treatment options.
A healthy 12-year-old dog who has a curable tumor removed could have 2-4 more wonderful years with you.
PET CANCER MYTH #4: Chemotherapy will make my pet miserable
The Reality: do dogs and cats tolerate chemotherapy?Pets tolerate chemotherapy better than humans do.
When most people think of chemotherapy, they picture hair loss, severe nausea, and debilitating side effects.
But here’s what’s different in veterinary medicine:
- We use lower doses. Our goal isn’t to cure cancer at all costs (i.e. quantity of life) – it’s to extend quality of life.
- We use gentler protocols that cause fewer side effects.
- Pets typically don’t lose their hair (except in rare cases with certain breeds).
- Pets don’t have psychological issues. They don’t know they’re sick. They don’t anticipate feeling bad. They don’t experience the psychological distress that humans often do.
Side effects are usually mild. The most common side effects are:
- Mild digestive upset (usually managed with medication)
- Temporary decrease in appetite
- Mild fatigue for a day or two after treatment.
- Nothing dramatic in most patients.
Most pets receiving chemotherapy continue to eat, play, and enjoy life.
In fact, many owners tell their oncologist, “I can’t even tell (s)he’s getting chemo!”
Your oncologist will or should go over the most common side-effects so you are fully informed.
One last very important point: nobody will force you to choose chemo (or radiation for that matter, another option to treat some cancers)!
Your surgeon or oncologist will only recommend it if it’s been shown to make a difference.
It all depends on the type of tumor.
PET CANCER MYTH #5: If the lump isn’t bothering my pet, I should just leave it alone
The Reality: By the time a tumor “bothers” your pet, it will be much harder (and invasive) (and costly) to treat.
Cancer doesn’t hurt in the early stages.
A small, removable tumor doesn’t cause pain.
That’s why a diagnosis of cancer is sometimes delayed.
But if you wait until it’s ulcerated, infected, bleeding, stretching the skin, or interfering with movement, the surgery becomes much more complicated and invasive – and the cancer may have already spread.
Early detection and early treatment offer the best outcomes.
If you notice a lump on your dog or cat, don’t panic, but don’t ignore it.
Have your family vet or ask for a referral to a surgeon to examine the mass.
Remember: Not every lump is cancer, but every lump should be checked.
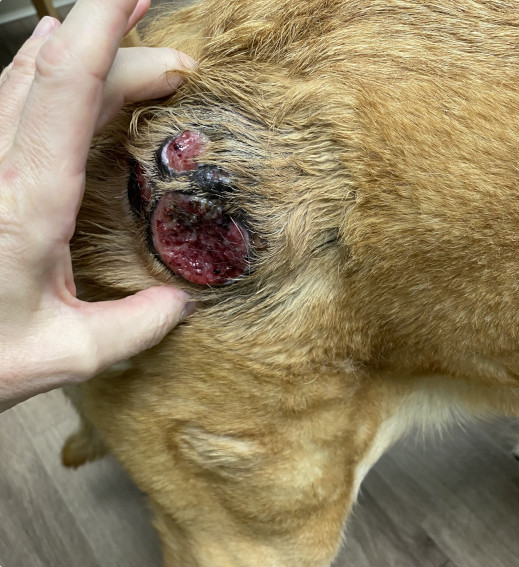
PET CANCER MYTH #6: Cancer treatment is always expensive and not worth it
The Reality: Treatment costs vary widely, from a simple pill to injections. Many options are more affordable than you think.
Yes, some cancer treatments – especially with a board-certified surgeon – can be more expensive than with your family vet.
But there is a reason your family vet might recommend a surgeon, depending on the complexity of the surgery.
You don’t have to do everything.
You can choose surgery without chemotherapy, or palliative care without aggressive treatment.
What matters is making the choice that’s right for you, your family and your pet.
My favorite tool against difficult financial decisions: pet insurance for cancer treatment.
Some include cancer treatment, some have it as an option.
Pet insurance can save your pet’s life.
PET CANCER MYTH #7: Amputating a leg is cruel
The Reality: most dogs and cats adapt to having 3 legs remarkably well – and it can save their life.
This is a conversation we have with 99% of pet owners whose pet needs an amputation.
You just cannot help but think of yourself hoping on 1 leg for the rest of your life.
But that’s just it.
Pets don’t hop on 1 leg, they can walk, run, jump, and play on 3 legs!
Bone cancer in dogs (osteosarcoma) is one of the most common reasons for limb amputation.
And we understand why the idea seems devastating.
Pets don’t have the same emotional attachment to having 4 legs that we do.
They don’t even know how many legs they have!
They live in the moment.
They don’t mourn the loss of a leg – they’re just relieved the pain is gone.
Most pets are walking within hours of surgery – we see it all the time, as hard as it is to believe.
Within weeks, they’re running, playing, and acting like nothing happened.
We’ve seen 3 legged dogs hike, swim, and even do agility courses.
Living with bone cancer pain, and the risk of breaking the weakened bone, is far more cruel than living with 3 legs.
If amputation can give your dog or your cat more comfortable, happy years (especially with chemotherapy), that’s a gift.
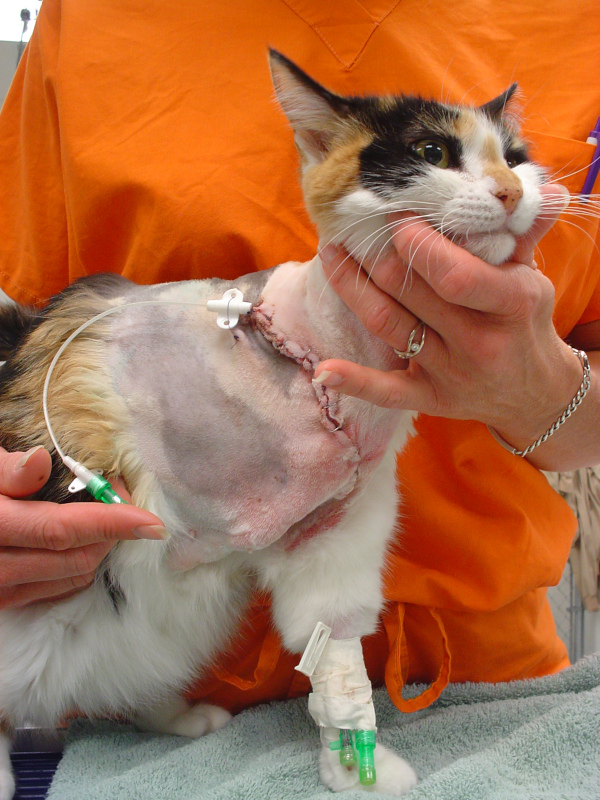
PET CANCER MYTH #8: Natural or holistic treatments can cure cancer without surgery or chemo
The Reality: there is no scientific evidence that holistic or natural treatments alone can cure cancer in dogs or cats.
If they did, we would know.
We’re all for integrative approaches, such as:
- A diet change to an “anti-cancer” food
- Supplements that support immune function
- Acupuncture for pain management
- CBD for comfort (where legal and vet-recommended).
These can be wonderful complementary options that improve quality of life.
But they are not replacements for proven treatments like surgery, chemotherapy, or radiation.
Delaying effective treatment to try unproven therapies can allow cancer to progress to a point where it’s no longer treatable.
If you’re interested in holistic approaches, work with a vet who can integrate them safely alongside scientifically proven treatments.
PET CANCER MYTH #9: I would know if my pet were suffering
The Reality: Pets are masters at hiding pain and sickness.
Remember, if an animal acts sick in the Wild, they get eaten.
Dogs and cats are hardwired to mask weakness – it’s a survival instinct.
Your pet might still wag their tail, eat, and greet you at the door even while dealing with significant discomfort.
This is why regular veterinary exams are crucial for early cancer detection in dogs and cats, especially as they age.
Your vet can detect subtle signs of cancer such as:
- Weight loss
- Changes in muscle mass
- Enlarged lymph nodes
- Pale gums
- Lumps and bumps.
Annual exams for younger pets, and twice-yearly exams for senior pets (7+ years for large dogs, 10+ for small dogs and cats), give us the best chance of catching cancer early.
PET CANCER MYTH #10: My friend told me I should not treat my pet
The reality: always seek professional veterinary advice for pet cancer decisions.
Of course there are multiple variations: “my neighbor said”, “my colleague thinks”, “a family member told me”…
People have all kinds of ideas about all kinds of topics.
The last people you should get advice from is people who don’t have pets (or don’t like them!!!).
They simply cannot understand the bond and the love you have for your pet.
And the worst place to get advice is most online forums, where anybody with a keyboard will be happy to share their opinion, seemingly for free, but sometimes at a great cost to your pet.

BONUS PET CANCER MYTH #11: A good vet can tell if this is cancer or not
The reality: vets are not magicians.
We can have an impression.
We can even have a conviction.
But there is simply no way to confirm cancer in a dog or cat without diagnostics such as cytology or biopsy reviewed by a veterinary pathologist looking through a microscope.
We remove “benign” masses that turn out to be cancer, and “cancerous” masses that end up being benign all the time.
With all due respect to our colleagues, to this day, we have never ever met anybody with microscopic vision.
The only way to come up with the correct diagnosis is to look at actual cells under a microscope.

THE BOTTOM LINE: WHAT EVERY PET OWNER SHOULD KNOW ABOUT CANCER IN DOGS AND CATS
Cancer in pets is not an automatic death sentence.
Many cancers are treatable.
Some are curable.
And even when a cure isn’t possible, we have more tools than ever to extend quality of life and keep pets comfortable.
SIGNS OF CANCER IN PETS EVERY OWNER SHOULD WATCH FOR
Tips to remember:
- A loss of appetite is not normal
- Difficulty eating, chewing, or swallowing is not normal
- Bleeding is not normal
- Suffocating is not normal
- Limping is not normal
- Difficulty urinating or defecating is not normal
- Check your pet regularly for lumps, bumps, or changes
- Unintentional weight loss should be a cause for concern
- Notify your vet of any wound that just won’t heal
- Don’t wait. Have new lumps evaluated promptly
- Ask questions. Your vet wants to help you understand your options
- Age is not a barrier to treatment if your pet is otherwise healthy
- Surgery does not spread cancer – it often cures it
- Chemotherapy in pets is gentler than you think
- You have options at every budget level
- Quality of life matters more than quantity, and we can help you navigate that balance
10 IMPORTANT QUESTIONS TO ASK YOUR VETERINARIAN IF YOUR DOG OR CAT MAY HAVE CANCER
- What type of cancer is it, and how aggressive is it?
- Has it spread, or is it localized?
- What are my treatment options (surgery, chemo, radiation, palliative care)?
- What’s the goal of treatment – a cure or extending quality time?
- What’s the expected outcome with and without treatment?
- What will my pet’s quality of life be like during and after treatment?
- Do you know a surgeon and/or an oncologist you trust?
- How much time do I have to make a decision?
- What signs should I watch for that mean something has changed – and when should I get help?
- How do I know if my dog or cat is in pain from cancer?
Searching for answers about cancer in your dog or cat can feel overwhelming, but early detection, accurate diagnosis, and the right treatment plan can make a life-changing difference for your pet.
Cancer is scary.
Armed with accurate information, you can make decisions with confidence, give your pet the best possible care, and cherish whatever time you have together.
As we always say, “we would rather have 6 months of happiness, than 6 years of misery.”
Your pet is lucky to have an owner who cares enough to learn the facts.
And whatever you decide, know that you’re doing your best for the friend who has given you so much.
Ultimately, only you can make the decision.
We firmly believe that the best decision you can make is by working as a unified healthcare team, with your family vet and your surgeon.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What are the top 5 concerns before anesthesia?

Most pet owners are not really concerned about surgery.
They’re mostly afraid of anesthesia.
Here are their top 5 concerns, based on multiple conversations with pet lovers.
Note: we will not discuss one classic question here, which was answered in a previous blog:
https://www.drphilzeltzman.com/blog/is-my-pet-too-old-for-anesthesia/
1. Is Anesthesia Safe for My Pet?
Having a pet die under anesthesia is probably the #1 fear of most pet owners.
And we’d be the first ones to tell you that no anesthesia is 100% safe.
Few things in life are.
Driving a car, flying on a plane or eating peanuts in not 100% safe.
The fear of anesthesia is very emotional and somewhat irrational.
It has to do with fear of the unknown.
It probably has to do with the magic of anesthesia.
Think about it.
We put a patient under anesthesia.
We do surgery, – and sometimes very invasive surgery (cutting tissues, removing body parts, putting broken bones together) – while the pet is sound asleep and completely pain free.
And then they magically wake up – all thanks to our amazing nurses.
Maybe not super happy, but overall comfortable.
And after a few hours or a few days, they look like they never had anesthesia.
What we can to help pet these days is truly remarkable!
Yet most clients are terrified of anesthesia.
Science confirms how incredibly safe anesthesia is.
The risk of a pet dying under anesthesia is, on average, under 0.25%.
While every death is an absolute tragedy, this number is incredibly low.
The risk is even lower in healthy patients, and a bit higher in very sick patients.
Still, this number is very low, which means that anesthesia is overall very safe.

2. What Are the Real Health Risks of Pet Anesthesia?
Many pet owners are concerned about how their pet’s preexisting health conditions could affect their ability to handle anesthesia.
Now, that’s a fair concern.
As you can imagine, a pet with severe heart disease, kidney disease, or liver disease, can be affected by anesthesia.
It’s very clear that pre-existing health issues increase the risk of anesthesia, making this a significant concern.
So what do we do to minimize the risks?
. We do a physical exam before any anesthesia and surgery.
. If we detect a mild heart murmur, we can change one of the drugs we use to put a patient under.
We can be more conservative with the amount of IV fluids we give to the patient, so we don’t overload the heart.
Some pets with severe heart disease should have an ultrasound of the heart and may need heart medication.
That would make anesthesia safer.
We require full blood work before any anesthesia and surgery.
If we find out that the patient has kidney or liver disease, we put them on IV fluid first thing in the morning to give their body time to get rid of the toxins before anesthesia and surgery.
Then we rely on the family vet to decide what medications, food, or supplements could support the liver or the kidneys.

3. What to Expect After Anesthesia?
Some pet owners worry about how their pet will recover from anesthesia.
They want to know how long it will take for their pet to wake up, how they will feel afterward, and what to expect during the recovery process.
A. How long will it take for my pet to wake up?
It takes a few minutes to a few hours.
It’s hard to predict, every patient is different.
As you can imagine, a young, healthy pet will usually wake up faster than a senior pet with a serious health condition.
B. How will my pet feel after anesthesia?
We wish we knew!
We don’t know how pets feel after anesthesia.
They refuse to tell us!
It’s probably safe to assume that they feel the same as a human waking up from anesthesia: groggy, spacey, and discombobulated.
The main difference is that pets, unlike humans, have no clue what just happened.
That’s when it’s important to have amazing, loving, caring nurses who can reassure their patients and make the waking part less stressful.

4. Will My Pet Be in Pain After Anesthesia?
Some pet owners are concerned that their pet is in pain during and after anesthesia.
We are extremely aware of this, which is the reason why we are so incredibly generous with pain medications.
Before, during and after our most common surgery, the TPLO (to address a torn ACL), we use about a dozen different types of pain medications!
That’s a lot!
In other surgeries, we use every possible way to fight pain.
For example, we routinely inject a pain-blocking medication near a nerve (similar to what you get at the dentist), under the guidance of an ultrasound.
As we always say, “pain is not acceptable.”
We have made a tremendous amount of progress in the last few years to understand, prevent and treat pain.
We now have access to safe and powerful drugs, and we use them every time we can.
5. What to Expect After Surgery?
Pet owners who haven’t worked with us before probably worry about not fully understanding the surgery, the risks and the postop instructions.
We provide a ton of information so that our pet owners are fully educated before anesthesia and surgery ever happens.
We explain food and water restrictions, which medications to give or not give, and all specific preop and postop instructions.
We communicate via phone, email, video and face-to-face.
We provide written instructions, which we go over line by line, right before a pet goes home.
We always ask “do you have any questions?” several times, until all questions are answered.
So our clients should feel very well prepared before their pet’s surgery.
And if that were not enough, we’re just a phone call away if there’s any additional questions.
We may have done a procedure 1,000 times.
Yet for most pet owners, it’s their first time.
So we educate them step by step, so they are fully prepared.
Hopefully the answers to the top 5 concerns you may have before your pet’s anesthesia and surgery reassured you.
We will do everything we can to ensure a safe and happy outcome.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Is my pet too old for anesthesia?

Is my pet too old for surgery?
We often hear this question from pet lovers, and even occasionally from family vets.
What they really mean is: is this pet too old for anesthesia?
Our usual answer is “Age is not a disease,” which is true.
Age is just a number.
We’ve seen extremely sick 5 year old patients, and very healthy 15 year old patients.
Which one do you think is at higher risk for anesthesia?
In addition, all dogs are not treated equal. A 10 year old poodle cannot be treated like a 10 year old Mastiff (we are alluding to the fact that it is said that small dogs live longer than large breeds).
Rather than a blanket, somewhat tongue-in-cheek answer (“Age is not a disease”), the solution to the dilemma is a bit more nuanced.
It’s not so much the age, or the number of years, that matter.
Instead, it’s the consequences of aging that we should focus on, because it makes the patient more “frail”.

What is a frail patient?
In humans, “frailty” is defined as having less “fuel in the tank” and being “easier to be stressed out” (in the medical sense).
Frailty better predicts getting in trouble (or dying) under anesthesia, compared to age alone.
A frail patient will have a tougher time maintaining their heart rate and blood pressure, or staying warm, or breathing well, while under anesthesia.
Their liver and kidneys may be less capable of eliminating toxins (e.g. anesthesia drugs).
Who is considered a senior patient?
- Senior age is tough to tell in a dog, so it is considered to be the last 20% to 25% of the pet’s lifespan.
- Cats are more uniform in size compared to dogs, so they’re considered senior once they turn 10.

So how do we keep senior patients safe?
We take multiple precautions, depending on the particular patient, including:
- smaller drug amount.
- more padding, from the kennel to the OR and back.
- more heat support.
- more oxygen at the beginning and the end of anesthesia.
- conservative amounts of IV fluids to avoid overloading the heart.
- appropriate amounts of pain medications: not too little, not too much.
- overall more TLC, which might include hugs, kisses and handfeeding.
How about anesthesia drugs in older patients?
The general idea is to give as little as needed.
More specifically, we can lower the amount of drugs to put them, and keep them, under anesthesia.
In addition, we sometimes will avoid using a certain type of drugs altogether, depending on the organs affected, such as heart, liver, and kidneys, based on preop exam & blood work results.
And of course, like any of our patients, a senior pet will be closely supervised by one of our amazing nurses, from the very beginning to the very end of anesthesia.

How many senior patients die under anesthesia?
Thankfully, dying under anesthesia is exceedingly rare when all of the above precautions are taken.
In 2008, a gigantic British study (on almost 100,000 dogs and almost 80,000 cats) showed that 0.17% of dogs and 0.24% of cats die under anesthesia.
And you would think those numbers could be even lower today with safer drugs, better protocols and fancier anesthesia monitoring.
A death is always a tragedy, but these numbers are incredibly low when you remember that they combine the absolute healthiest and the absolute sickest of patients.
So remember, it’s not the age of the patient that matters, as much as how sick they are.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified
Pete Baia, DVM, MS, DACVS

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Notes from a physical therapy conference in South Africa
I was very fortunate to attend the 12th Symposium for the International Association of Veterinary Rehabilitation and Physical Therapy (IAVRPT) in Cape Town, in South Africa.
Below are some notes that can be of interest to pet lovers.
I will also intersperse a few nice pictures, with a caption.
It was an amazing conference, with over 200 people, from all over the world, who dedicate their lives to physical therapy and rehab in pets.

What is a force plate?
I attended a day of “lab” work centered around the use of a force plate.
A force plate is a sensitive platform embedded in a walkway, that objectively measures the weight a patient places on each leg, in order to diagnose subtle lameness and track their progress during rehab.
Vets (mostly surgeons) have said for years that the weight distribution is not 50-50 between the front and back legs. We’ve said it’s 60% in the front, because the front legs “carry” the head, the neck and the chest. And the back legs mostly “carry” the belly, so that’s only 40% of the weight.
Force plate analysis shows that this is a generalization. We just can’t compare the body shape of a mini Doxie, a Bassett hound and a mastiff.
This is important when we talk about the impact of weight loss and leg amputation.
Weight loss benefits the entire body, and now you understand why it helps the front legs even more, since they “carry” more weight.
The speaker, a physical therapist, also explained that seemingly minor things can change the results of force plate analysis: the position of the pet’s head, a wagging tail, turning the head to get a treat, pulling on the leash, wearing a neck collar rather than a harness, etc.
Bottom line: a force plate is very helpful to diagnose a difficult lameness, and we have a lot more to learn!

How to best treat arthritis pain?
I loved a lecture presented by a surgeon, who reminded us that the source of pain in a patient with arthritis is the LINING of the joint.
Therefore, treatments should target the lining of the joint.
We’ve started to inject various products and medications in our patients’ joints, with excellent results.
We started years ago with:
- stem cells
- PRP (Platelet Rich Plasma), both of which you may have heard of in people.
Now, we also inject:
- collagen (Spryng®)
- steroids (cortisone)
- hyaluronic acid etc.
The results have been very impressive, including in “desperate” cases where nothing else had helped the patient.

When should we use modern arthritis drugs?
Another physical therapist reminded the audience of something surgeons know all-too-well. The newer anti-arthritis medications like Librela® and Solencia® should not be used when a joint is instable. To avoid potentially devastating side-effects, surgery should be recommended first in these patients, specifically to stabilize the joint.
In addition, these drugs should NOT be combined with Non-Steroidal Anti-Inflammatory drugs (NSAIDs), again for fear of potentially disastrous side-effects.
So remember, our current understanding is that there are at least 2 situations when Librela® and Solencia® should not be used:
- with an unstable joint
- with an NSAID
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Fascinating Monkeys in South Africa and Zimbabwe
| I was very fortunate to recently visit South Africa and Zimbabwe after a veterinary conference. Since 100% of the pet owners we meet are animal lovers, I thought I would share some information and pictures about his incredible trip. |

When traveling through southern Africa, it’s impossible to miss the lively antics of monkeys.
We mostly observed 2 species: vervet monkeys and baboons.
These primates are not only fascinating from a scientific perspective, but their bold behavior provides unforgettable moments for visitors – sometimes a bit scary!
Here’s a look at these cheeky creatures and my personal encounters with them.
Vervet Monkeys in South Africa
Vervet monkeys may not be the most well-known monkeys, but they are found across sub-Saharan Africa.
They are small monkeys, weighing only 6 to 11 lbs (3 to 5 kg).
For comparison, that’s the weight of a Yorkie or a mini Doxie.
They have distinctive, cute, black faces framed by white fur and long tails that help with their agile movements.
These monkeys are highly social, living in troops that can range from a few individuals to over 50.
Their diet is omnivorous, meaning they eat a bit of everything, including fruits, flowers, insects, and sometimes small animals.

Adorable Vervet Babies
Vervet monkey babies are adorable, with their tiny black faces and inquisitive eyes.
These shy little ones are often seen clinging tightly to their mothers’ bellies as the moms move gracefully through trees.
As they grow, they begin to explore their surroundings cautiously, staying close to their protective mothers.
The sight of a vervet mother tenderly grooming her baby is a heartwarming reminder of the strong bonds within these social groups.

A Bold Encounter
During lunch in South Africa, I witnessed just how bold vervet monkeys can be.
A guest was enjoying his meal when, in the blink of an eye, a vervet jumped onto the table and grabbed a piece of chicken.
The guest’s surprised scream was met with the monkey’s triumphant retreat to a nearby tree, where she enjoyed her stolen snack.
I apologize for the blurry pictures, but it’s a miracle I was able to get shots from the encounter, which lasted a split second!
And during this entire scene – her baby clung to her belly!

Baboons in Zimbabwe
Baboons are much bigger monkeys. They are among the largest primates in Africa.
Male typically weigh 44 to 88 lbs (20 to 40 kg), so between a Border Collie and a Lab.
Females average 22 to 33 lbs (10 to 15 kg), same as a Cocker or a Beagle.
These primates live in complex social structures and display remarkable intelligence, including tool use and problem-solving skills.
Their diet is even more varied than that of vervet monkeys, ranging from plants to small mammals.

Close Call with a Baboon
One afternoon in Zimbabwe, while visiting the impressive Victoria Falls, I found myself a little too close to a baboon for comfort.
It certainly wasn’t intentional. We simply stumbled across a group crossing the path…
We stopped and observed, respectfully, with complete admiration since it was by far the closest encounter, and the biggest group.
They kept moving around us, looking for food on the ground.
At one point, a large male sat just a few feet away.
I froze (OK, OK, aside from taking 348 pictures of him!).
For a heart-stopping moment, I thought he might leap toward me.
Instead, he jumped into a tree with effortless grace.
While baboons can be intimidating due to their size and sharp canines, they generally avoid conflict with humans unless provoked or seeking food.
The canines of a male are easily the size of those of a German shepherd or a Rottie!

Why Are Monkeys So Bold?
Since we invaded their territory, these monkeys have adapted to human presence, often frequenting tourist spots where they’ve learned that food is very easy to come by.
Both vervet monkeys and baboons have adapted to living alongside humans.
In many areas, their natural habitats overlap with villages, towns, and tourist hotspots.
They’ve learned that humans often mean easy access to food, whether it’s from unattended picnics, restaurant tables, or open car windows.
Their boldness is a testament to their intelligence and adaptability, but it’s also a reminder of the challenges of human-wildlife coexistence.

A Word of Caution
While vervet monkeys and baboons might seem amusing or endearing, it’s important to treat them with respect.
Feeding them or leaving food accessible can encourage aggressive behavior and disrupt their natural foraging habits.
Observing these animals from a safe distance ensures both your safety and their well-being.
Final Thoughts
From the cheeky vervet monkey who stole a restaurant guest’s chicken dinner to the imposing baboon that startled me in the Wild, these primates leave a lasting impression.
Their boldness adds a unique charm to encounters with Africa’s wildlife, blending humor and awe.
Just remember to protect your snacks – and keep your distance!
We can’t help your baboon, but if you would like to learn how we can help your cat or your dog with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

