Dr. Phil Zeltzman’s Blog
How do we monitor your pet’s anesthesia?
Vets have been able to dramatically decrease the death rate under anesthesia thanks to better anesthesia drugs and better monitoring.
What does monitoring mean?
Let’s review some techniques we use at our hospital to reduce the risks.
Please understand that not all practices have this equipment, for financial reasons mostly. As a general rule, we perform higher-risk and longer anesthesia and surgery, so we have an obligation to provide the best equipment available.
Vital signs
One of the many roles of the anesthesia nurse is to record the pet’s vital signs and numbers indicated by the devices described below: body temperature, blood pressure, heart rate, respiration rate, temperature etc.
This is critical to determine if there is a trend.
For example, is the blood pressure slowly dropping?
The surgeon is then alerted, and decisions can be made in a timely manner.
ECG
Most people have had an ECG (aka EKG), so most are familiar with the concept. An ECG measures the electric currents generated by the heart. It helps monitor the heart rate and rhythm. It allows early recognition of heart issues, such as arrhythmias (extra heart beats), which can then be treated appropriately.
Blood pressure
Blood pressure measurement is probably the earliest indicator of problems with anesthesia in pets.
Pulse oximetry
This is a way to estimate how much oxygen is being carried by red blood cells.
You may have been connected to such a device at the hospital.
This is the clip that is usually placed on your finger.
In pets, the probe is usually placed on the tongue.
Temperature
Anesthesia commonly reduces the body’s temperature.
We are obsessed with maintaining pets’ temperature, especially small ones.
Opening a body cavity (chest or belly) leads to losing even more body heat.
So we use several modalities to keep the temp up.
For example, every single patient gets a “Bair Hugger,” which is a warming blanket, in addition to a heating pad under their body.
It is important to warm patients up after surgery as well.
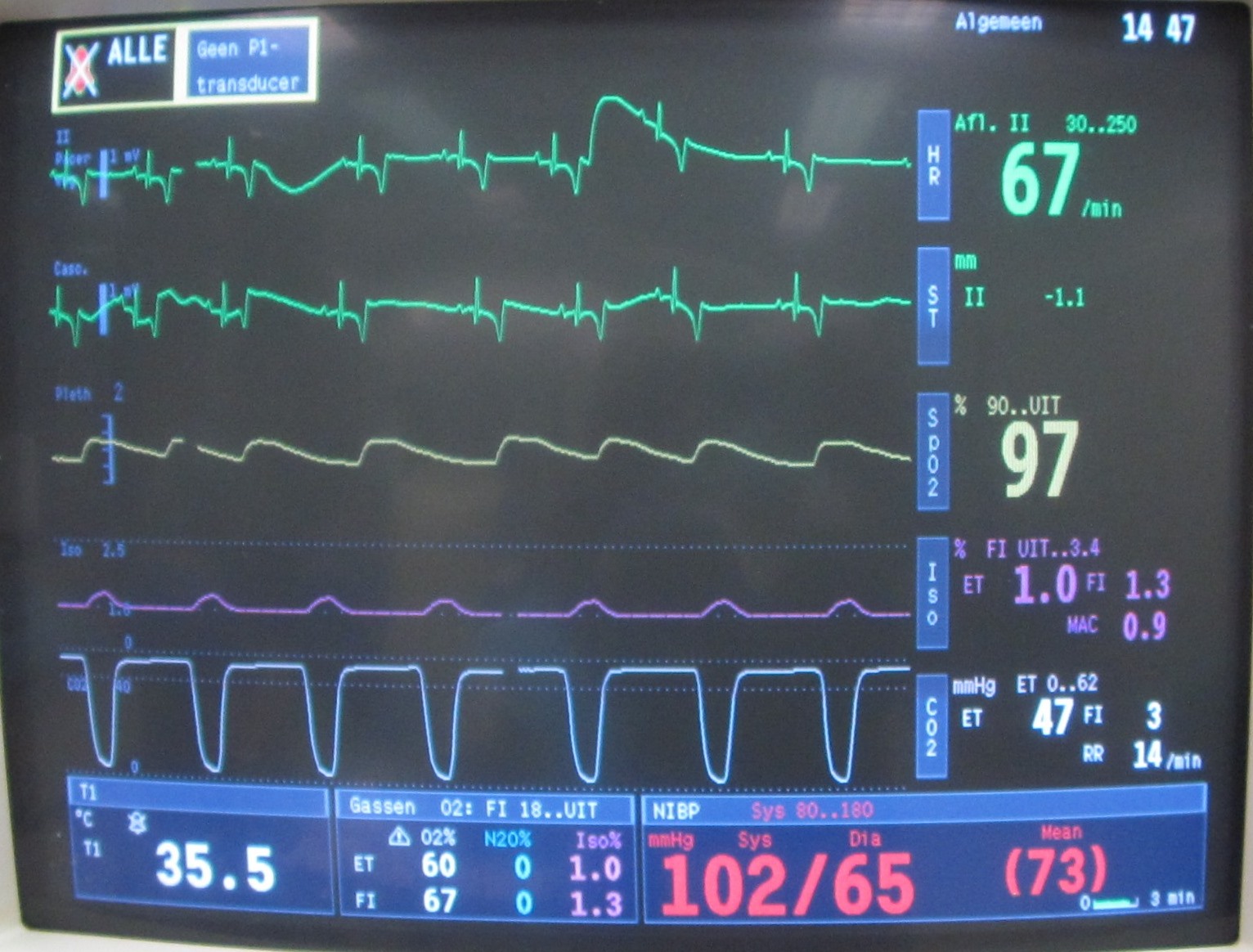
Capnography
This is a fancier machine, not routinely available in general practices.
It monitors the amount of CO2 (carbon dioxide) in the patient.
If it becomes too high, it means that the patient is not breathing enough to “blow off” the toxic CO2.
The anesthesia nurse would then help the patient breathe.
Such equipment undoubtedly helps us greatly improve the safety of anesthesia.
By far, my favorite way to monitor my patients is my skilled nurses.
The risk obviously depends on the patient and the type of surgery.
For example, spaying a healthy 6 month old Lab puppy is less risky that removing a 1 pound cancerous tumor from the liver of a 14 year old diabetic, seizure-prone poodle with heart and kidney disease!
That said, the OVERALL death rate under anesthesia is:
. 0.06 to 0.43% in cats;
. 0.11 to 0.43% in dogs
according to several studies conducted in the late 1990s.
As you can see, careful monitoring makes the anesthesia as safe as possible, so that we can reach our ultimate goals: a healthy pet and a happy pet owner.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

