Dr. Phil Zeltzman’s Blog
How do we monitor your pet’s anesthesia?
Vets have been able to dramatically decrease the death rate under anesthesia thanks to better anesthesia drugs and better monitoring.
What does monitoring mean?
Let’s review some techniques we use at our hospital to reduce the risks.
Please understand that not all practices have this equipment, for financial reasons mostly. As a general rule, we perform higher-risk and longer anesthesia and surgery, so we have an obligation to provide the best equipment available.
Vital signs
One of the many roles of the anesthesia nurse is to record the pet’s vital signs and numbers indicated by the devices described below: body temperature, blood pressure, heart rate, respiration rate, temperature etc.
This is critical to determine if there is a trend.
For example, is the blood pressure slowly dropping?
The surgeon is then alerted, and decisions can be made in a timely manner.
ECG
Most people have had an ECG (aka EKG), so most are familiar with the concept. An ECG measures the electric currents generated by the heart. It helps monitor the heart rate and rhythm. It allows early recognition of heart issues, such as arrhythmias (extra heart beats), which can then be treated appropriately.
Blood pressure
Blood pressure measurement is probably the earliest indicator of problems with anesthesia in pets.
Pulse oximetry
This is a way to estimate how much oxygen is being carried by red blood cells.
You may have been connected to such a device at the hospital.
This is the clip that is usually placed on your finger.
In pets, the probe is usually placed on the tongue.
Temperature
Anesthesia commonly reduces the body’s temperature.
We are obsessed with maintaining pets’ temperature, especially small ones.
Opening a body cavity (chest or belly) leads to losing even more body heat.
So we use several modalities to keep the temp up.
For example, every single patient gets a “Bair Hugger,” which is a warming blanket, in addition to a heating pad under their body.
It is important to warm patients up after surgery as well.
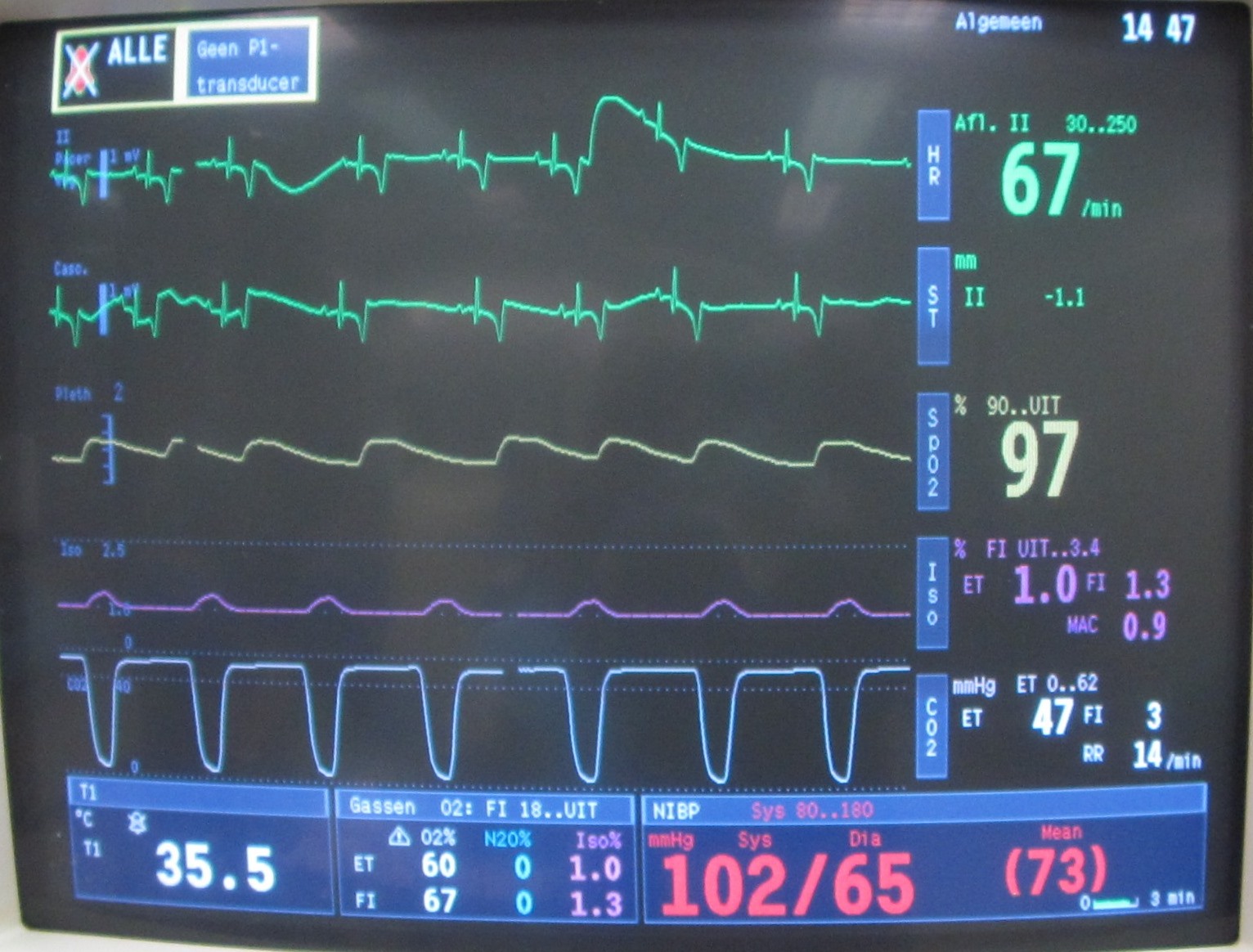
Capnography
This is a fancier machine, not routinely available in general practices.
It monitors the amount of CO2 (carbon dioxide) in the patient.
If it becomes too high, it means that the patient is not breathing enough to “blow off” the toxic CO2.
The anesthesia nurse would then help the patient breathe.
Such equipment undoubtedly helps us greatly improve the safety of anesthesia.
By far, my favorite way to monitor my patients is my skilled nurses.
The risk obviously depends on the patient and the type of surgery.
For example, spaying a healthy 6 month old Lab puppy is less risky that removing a 1 pound cancerous tumor from the liver of a 14 year old diabetic, seizure-prone poodle with heart and kidney disease!
That said, the OVERALL death rate under anesthesia is:
. 0.06 to 0.43% in cats;
. 0.11 to 0.43% in dogs
according to several studies conducted in the late 1990s.
As you can see, careful monitoring makes the anesthesia as safe as possible, so that we can reach our ultimate goals: a healthy pet and a happy pet owner.
If you would like to learn how we can help your pet with safe surgery and anesthesia, please contact us through www.DrPhilZeltzman.com
Never miss a blog by subscribing here: www.DrPhilZeltzman.com/blog
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How Yoda lost his tail
Yoda was a healthy 4 year old French Bulldog with one ongoing, itchy, painful, smelly issue…

He had frequent skin infections around his crooked little tail.
As in many Bulldog type dogs, Yoda had a “screw tail,” also called “corkscrew tail,” “ingrown tail,” or tail fold dermatitis.”
The problem with this condition is not the tail itself, but the issues the malformation creates. The malformed tail creates skin folds that become infected.
The skin folds are not exposed to air and they create a moist, dark, warm environment – heaven for all kinds of nasty bacteria.
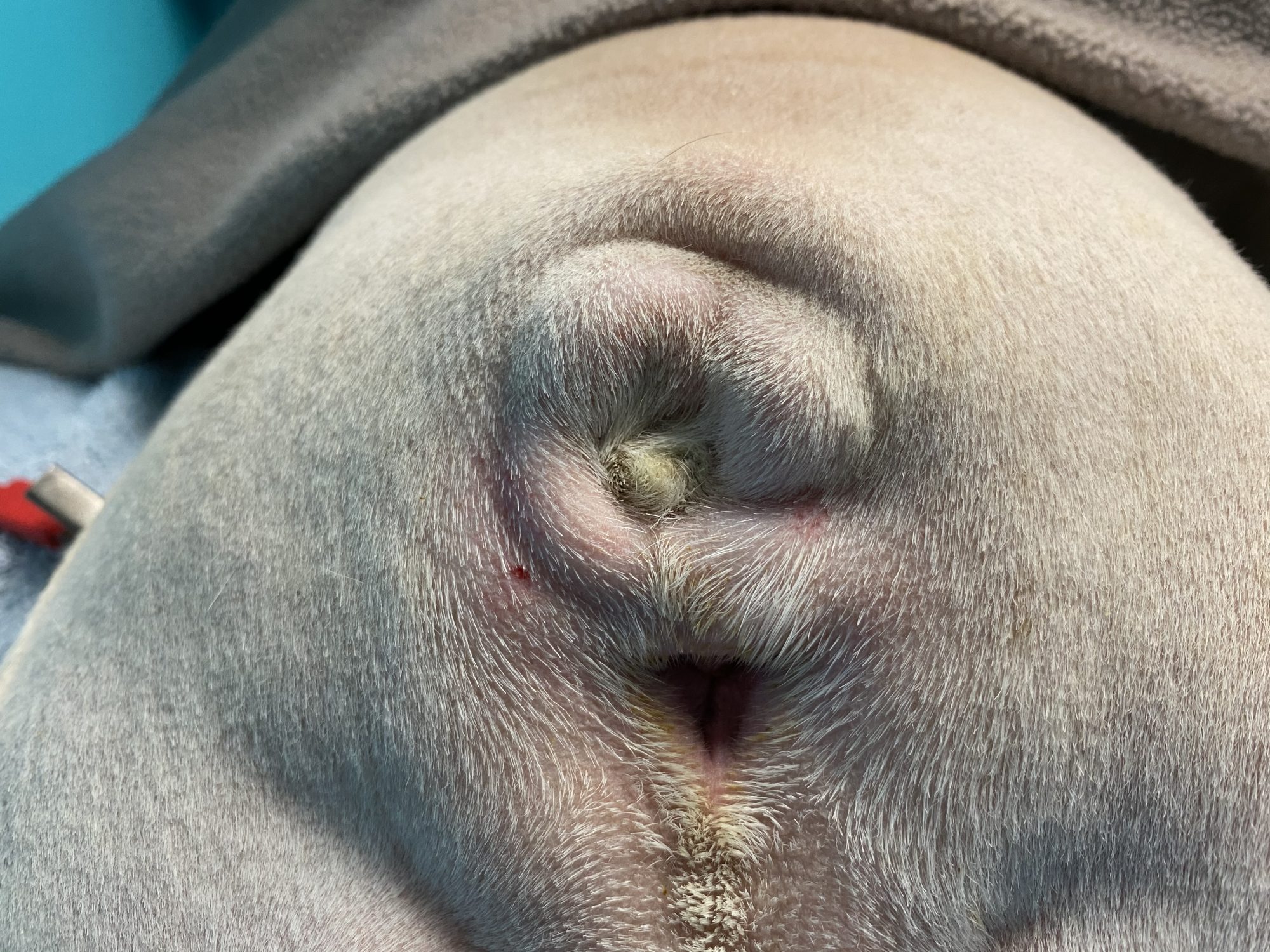
Mild cases of screw tail can be treated medically or conservatively with proper hygiene & daily cleaning.
Unfortunately, despite Yoda’s family vet’s and his owner’ best efforts, nothing helped.
This is a classic, vicious cycle with no end in sight. Antibiotics didn’t work. Antiseptics didn’t work. Pet wipes didn’t work.
Most of the clients I see for this problem are frustrated after months to years of unsuccessful treatments and impressive veterinary bills.
So what’s the solution?
The only permanent solution is to remove the “screw tail.”
The goal of surgery is to remove the malformed part of the tail and the entire infected skin fold.
The end result: no more dark, moist, warm environment for bacteria to thrive in.
This is a fairly technical and sometimes challenging procedure, which is often performed by a board-certified surgeon.
There are a few risks to be aware of:
. Patients with a flat face (brachycephalic breeds) have a higher risk during anesthesia, so an experienced anesthesia nurse is critical.
. We have to work in a filthy area, both because of the infection in the tail fold and because of the proximity of the anus. We certainly scrub the skin as thoroughly as possible, but there is always a mild risk of infection.
. There is a delicate balance between removing too much skin and not enough. Not enough skin leaves infection behind, so there is potential for complications. Too much skin taken away can lead to difficulty stitching up the skin nicely.
. Fecal incontinence is a complication that is often mentioned, but that is a low risk in the hands of an experienced surgeon.
. After surgery, some patients drag or scoot their hind end, which can result in damage to the incision and poor healing.
The outcome is typically very good with proper postop care.
Yoda did great during his procedure. He recovered smoothly from anesthesia and surgery.
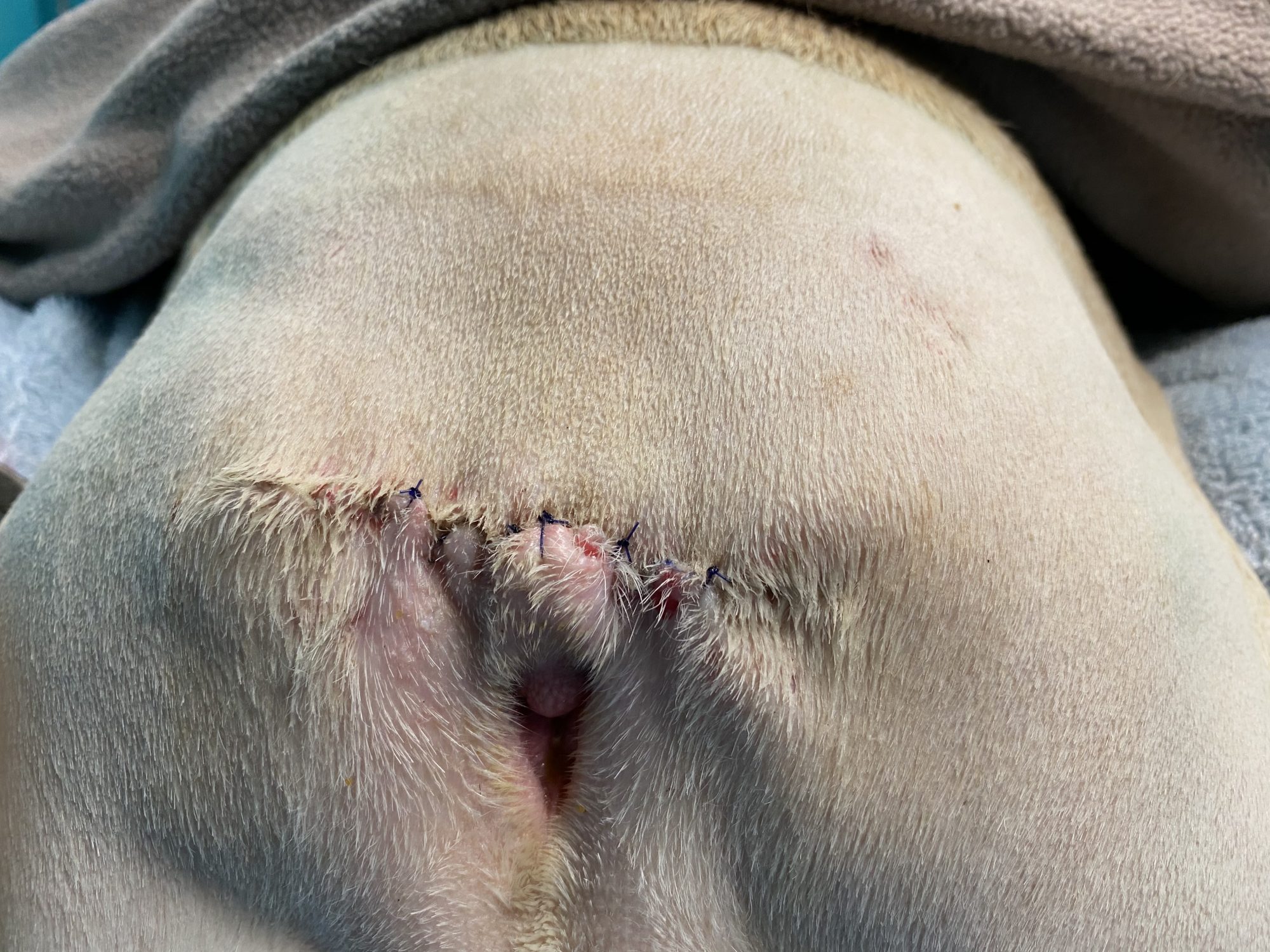
After 3 weeks of TLC, his owner reported that Yoda was doing well at home.
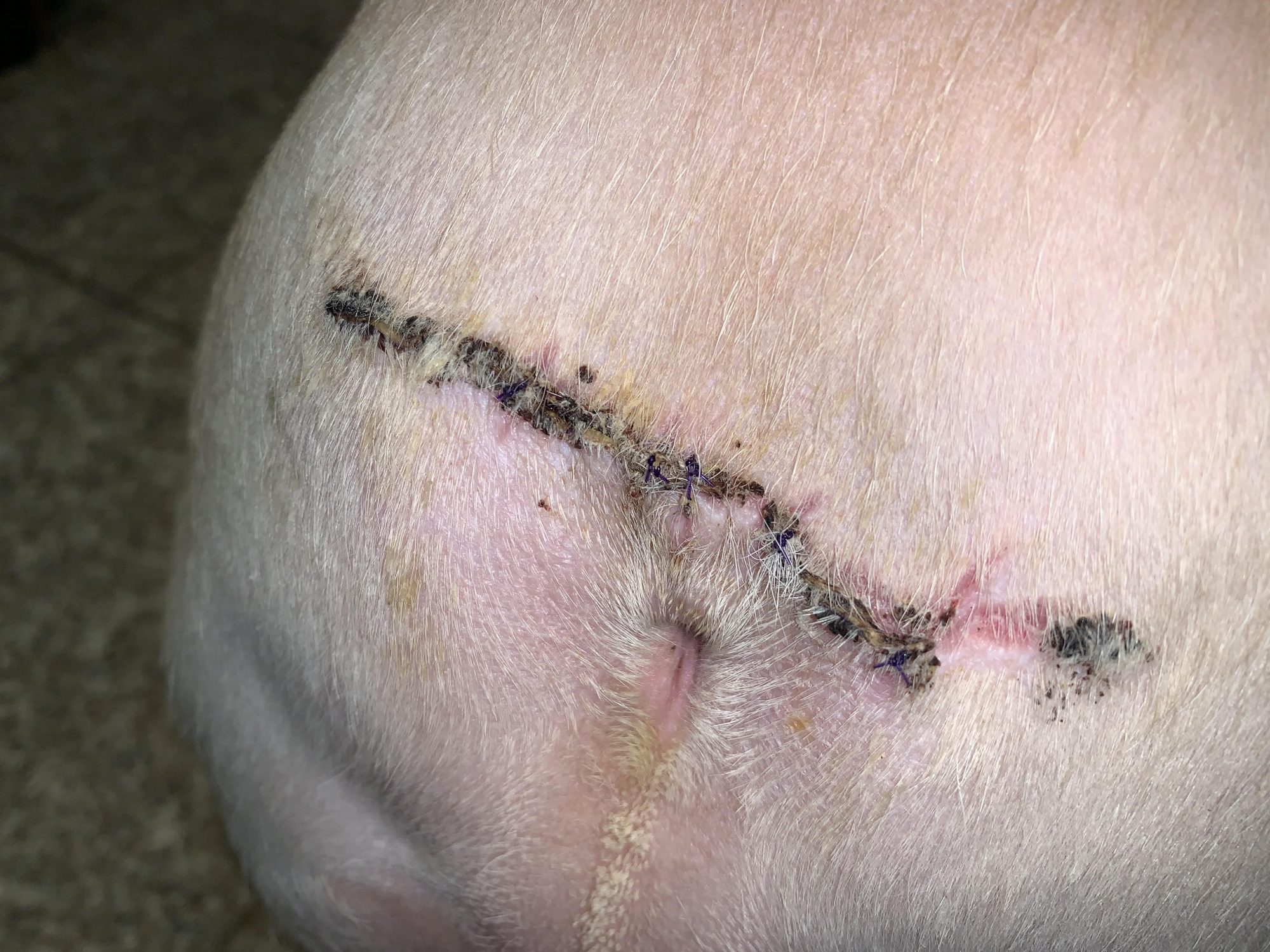
No more smell, no more itching, no more scooting, no more soreness.
Just pure Bulldog happiness, and a happy, wiggly behind.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What caused Kona to lose a kidney?
Kona, a female Lab, was only 1 year old, yet she had had several bladder infections.

Rather than keeping her on repeated antibiotics, her family vet looked into the situation and discovered that Kona had an extra fold over her vulva.
This common (and under-diagnosed) condition is called a “redundant vulvar fold,” “vulvar fold dermatitis,” “recessed vulva” or “hooded vulva” (see below a picture in another patient, a 6 year old Newfie, where the vulva is barely visible).
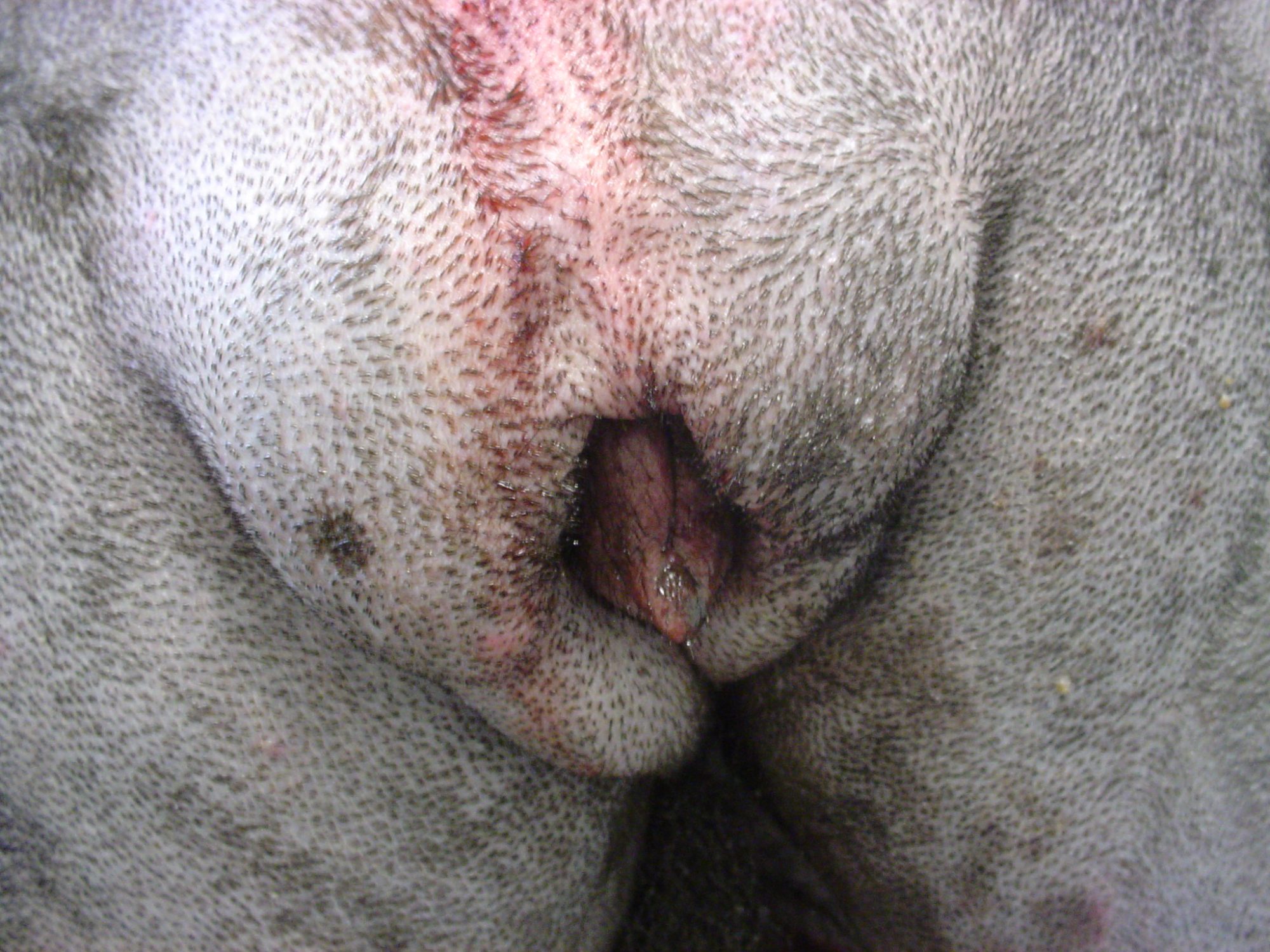
The treatment is a reconstructive surgery called vulvoplasty or episioplasty. The goal is to remove the extra skin.
The main challenge is to remove just the right amount. Not too little, and not too much.
Kona’s pet owner wisely chose to have her spayed under the same anesthesia. Her vet asked me to look into the possibility of a malformation of her urinary system called an ectopic ureter. The ureter is the tiny tube between the kidney and the bladder.
It was a possibility because Kona was constantly leaking urine, i.e. she was incontinent.
During surgery, we removed the extra skin fold, spayed her, found no ectopic ureter… but found another condition.
She had a hydro-ureter, i.e. a ureter that was huge, about 5 times bigger than on the other side. This required removing it, and sacrificing the kidney on the same side – of course after calling the owner in the middle of surgery to request permission to do so.
Surgery was uneventful, and Kona recovered smoothly from anesthesia.
Here is a (warning, graphic) picture of the kidney and the enlarged ureter (hydro-ureter) in another patient, a 6 year old Malamute.
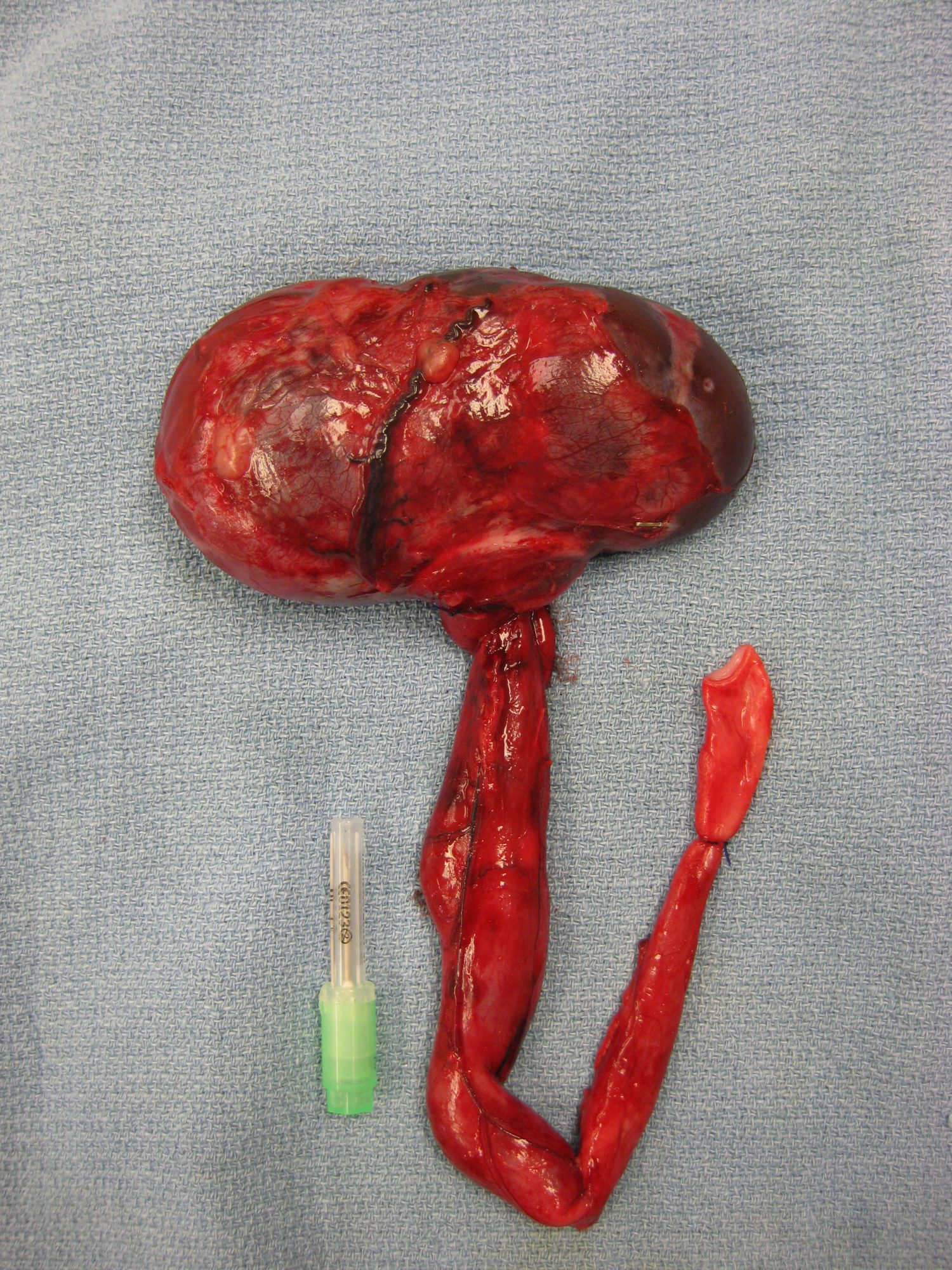
Three weeks later, her owner EB writes:
“Kona is doing well. I have not noticed any leaking and when she urinates, it is a steady stream. Her incision looks great and she is her spunky self.”
Obviously, this is an unusual situation, but a good reminder to keep an open mind when a patient has an unusual situation, like leaking urine constantly.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How Xena had a simple life-saving surgery
Xena, a beautiful 6 month old female German shepherd, was ready to be spayed. Benefits include eliminating the risk of mammary (breast) cancer and preventing a deadly infection of the uterus called pyometra.

In addition, Xena’s family vet discussed the benefit of performing a prophylactic gastropexy.
A what?
A gastropexy is a simple surgery performed to prevent twisting of the stomach – sadly sometimes called bloat – or more appropriately Gastric Dilatation Volvulus (GDV), stomach torsion or flipped stomach.
Prophylactic means that it’s an elective or preventive surgery performed before the stomach ever has a chance to twist.
The success rate of this simple surgery is very high. It is critical to understand that the dog can still bloat, ie the stomach fills up with air. This still means that they would need emergency treatment to deflate the stomach. But it’s a much safer place to be in, since the stomach should not twist on itself.
It is a potentially life-saving procedure that should be considered in Great Danes (the #1 breed for this disease), German shepherds, Dobies, Weimies, Labs and several other large dog breeds with a “deep chest.”

After Xena’s owner had a friend who lost her Great Dane because of a twisted stomach, she wisely chose the added surgery as recommended.
During the gastropexy, the stomach is tacked or stitched to the inside of the belly. This simple procedure prevents the twisting of the stomach.
Then a standard spay was performed.
I’ve performed many of these life-saving surgeries at the time of a spay or neuter. Occasionally, it is done in an older dog who is already spayed or neutered – which is still a great idea.
Xena recovered well after 4 weeks of restricted activity, pain medications and antibiotics.
And now, her family’s mind is at ease, knowing that they did all they could to help Xena live a long, healthy and hopefully GDV-free life.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
A LOOK BACK AT 2021…
A LOOK BACK AT 2021…
The beginning of a new year is a great time to reflect on past accomplishments. For me, as a surgeon, it includes thinking of all the patients we helped and which surgeries we performed the most.
This can give you an idea of which surgeries pets are most likely to need…
So here were our top 10 surgeries in 2021.
1. ACL SURGERY
It never fails.
ACL surgery remains the most common surgery we perform, mostly in dogs (and less so in cats).
We have different procedures in our toolbox depending on the patient.
. TPLO (Tibial Plateau Leveling Osteotomy) is THE most common surgery we perform, by far.
. The “traditional” technique with heavy nylon sutures can be used in well-selected dogs (and occasionally in cats).
. The TWO (Tibial Wedge Osteotomy) has come in handy a few times this year in dogs who had implants that prevented doing a TPLO, or who had extremely steep angle at the top of their shin bone.
. TTA (Tibial Tuberosity Advancement).
One size doesn’t fit all here. We don’t see every problem as a nail, and we don’t only have one hammer.
2. Mass removal
We’ve removed masses in and under the skin, in the chest, in the bone (legs, toes, jaws)…
Thankfully, not all tumors are cancerous, and we’ve removed many benign masses.
3. Belly surgery
Belly surgery or “exploratory laparotomy” allowed us to:
. remove foreign objects from the stomach
. remove body parts (gallbladder, spleen, adrenal gland)
. take biopsies
. remove bladder stones, etc.
You can read about bladder stone surgery here:
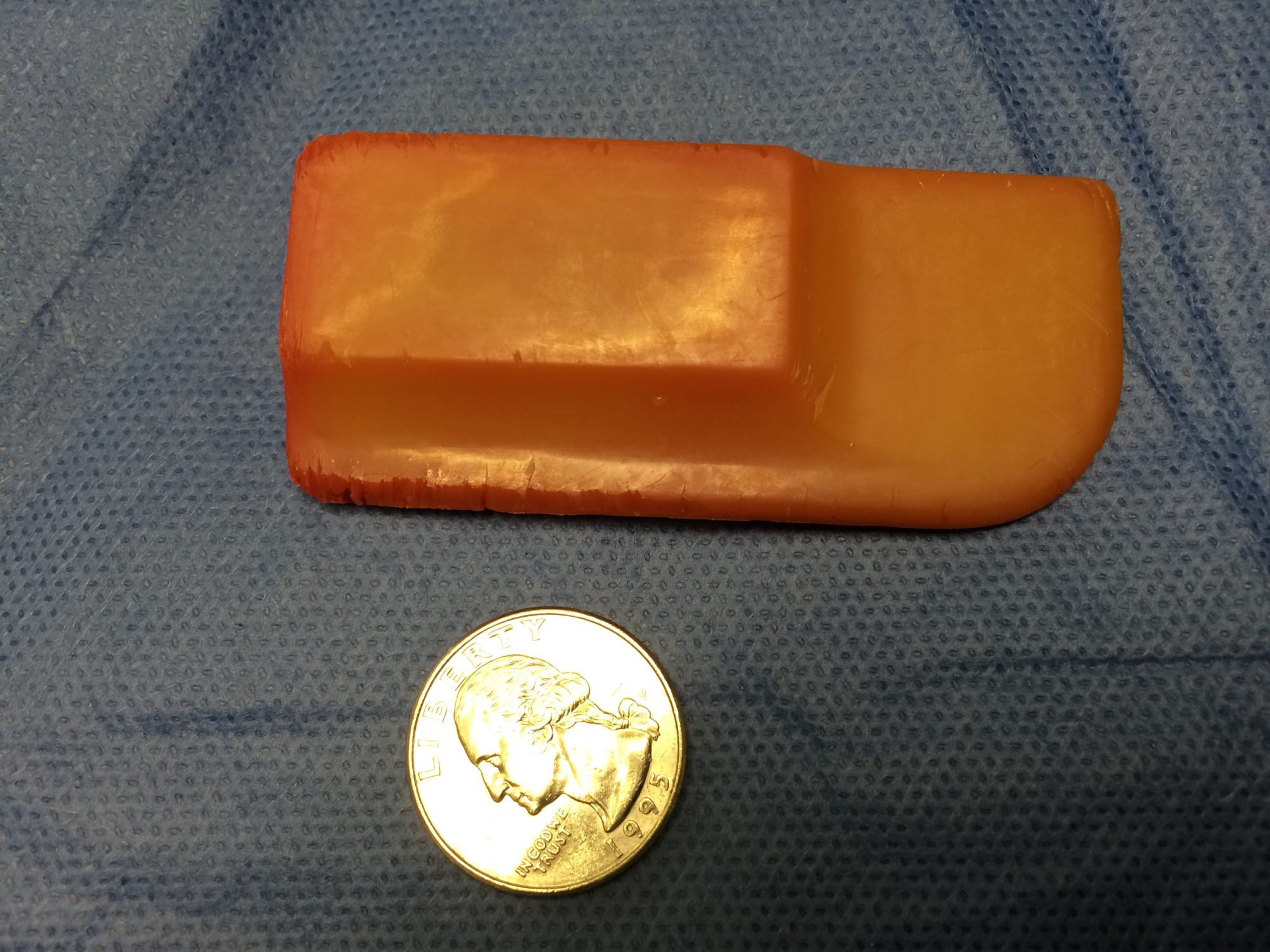
Some cats had their colon removed because of a serious condition called megacolon. This is the only definitive solution when cats are so severely constipated, that the colon has become a painful giant bag of dehydrated poop. At that stage, medications are a waste of time and money.
Procrastinating to move on with surgery invariably leads to a much worse anesthesia candidate. These cats may go from otherwise healthy to skinny and unhealthy. Not to mention the fact that they suffer from untreatable constipation.
We also performed a number of prophylactic gastropexies, a preventive procedure designed to present stomach twisting in dogs at risk for “bloat.” This life-saving procedure should be considered in Great Danes (the #1 breed for this disease), German shepherds, Labs and several other large dog breeds.
4. Joint dislocations
We’ve mostly treated joint dislocations in the hip and the knee. Some pets had trauma, others were born that way (congenital dislocation).
The most common one is the kneecap dislocation. The kneecap slides out of the groove where it is supposed to live, at the bottom of the thigh bone (or femur). It is common in dogs, and we’ve treated a few cats with that condition last year.
5. Fractures
We’ve fixed fractures in just about every bone this year, mostly the forearm (radius), the shin bone (tibia) and the thigh bone (femur), as well as some toes, the jaw and the arm (humerus).
To fix these broken bones, we’ve used plates and screws, pins, or a device called an external fixator.
Causes of broken bones mostly included jumping, falling or being hit by a car.
6. TECA
Total Ear Canal Ablation (TECA) is the only definitive treatment for dogs (most often Cockers) and cats who have never-ending ear infections. They lead to pain, head shyness and sometimes aggressiveness.
Unfortunately, most of these pets are treated with medications for years, which can’t even go down into the ear canal because it has become so swollen.
We occasionally perform a TECA in pets who had a tumor in the ear.
TECA is an invasive procedure, with possible complications, yet it fortunately works very well in the majority of patients.
7. FHO
FHO (Femoral Head Ostectomy) is used to treat hip dislocations or hip dysplasia.
The “ball” of the hip (femoral head) is removed during surgery.
FHO is also done in pets with a hip fracture or deterioration of the bone (e.g. Legg Perthes disease in small dogs).
8. Laryngeal paralysis
Dogs, mostly Labs, can have a condition that paralyzes their larynx, a.k.a. voice box, and causes them to suffocate. It’s an incredibly stressful condition. Fortunately, surgery (a “tie back”) allows them to have a wider airway, which typically works very well. These patients quickly go from suffocating to being able to breathe comfortably.
You can read about the amazing story of Mae Mae here:
9. Brachycephalic syndrome
This condition is seen in dogs (and rarely cats) with a flat face, which caused snoring and difficulty breathing: Bulldogs, pugs, Boston terriers, Persian cats etc.
It typically involves 4 conditions:
. The most visible part are stenotic nares (aka tiny nostrils) which prevents getting enough oxygen. Surgery involved making them wider, aka “a nose job” or a rhinoplasty.
. An elongated soft palate. The tip of the roof of the mouth is so long, that it covers the entrance of the windpipe. When it vibrates, it causes snoring. We can shorten it during surgery.
. Saccules are fleshy structures at the beginning of the windpipe. Over time, the saccules can pop out into the airway – and further block the flow of oxygen. We can remove them during surgery.
. A tiny windpipe, which we can’t do anything about.
You can read more about this surgery done on Kasper here:
https://www.drphilzeltzman.com/blog/guess-who-had-a-nose-job-today/
10. Reconstructive surgery
We did multiple surgeries that required reconstructing a body part:
. Cleft palate (or roof of the mouth), which you can read more about here:
https://www.drphilzeltzman.com/blog/squirrel-gets-a-new-lease-on-life-after-cleft-palate-surgery/
. Male cats who could not pee (P/U or perineal urethrostomy).
. A dog’s penis which had a (benign) tumor.
. Hernias, which are a condition where an organ ends up where it shouldn’t be.
Remembering some of the surgeries we’ve performed in 2021 is also an opportunity to give credit to the wonderful vets, nurses, and pet owners who have been caring for them.
Until next time,
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

