Dr. Phil Zeltzman’s Blog
How Madeline got a new lease on life
Madeline, a 7-year-old shepherd mix, had trouble urinating for about two months.

(You can tell from her picture that she’s not at all a spoiled pup!)
Fair warning: this is an unusually long blog. It’s longer than a tweet. If you read it until the end, you will learn several valuable lessons that could save your pet’s life one day. So please hang in there and read along. It’s actually a quick read!
Madeline would strain to urinate, with frequent attempts, and accidents in the house. There was no blood in the urine, which made it less likely to be a bladder infection.
X-rays didn’t show anything unusual, including bladder stones.
After two months of trying various treatments (antibiotics, steroids etc) that didn’t make any difference, Madeline’s owner got rather frustrated and went elsewhere to get an ultrasound. And that was the key decision: the ultrasound showed a mass in her bladder. Rather than being in an area where it’s easy to remove (eg the front of the bladder), it was located in the very back, at the junction of the bladder and the urethra (the tube between the bladder and the outside world). This area is called the trigone. It’s the muscle that allows a dog to be continent, ie the opposite of incontinent. This made removing the mass risky.
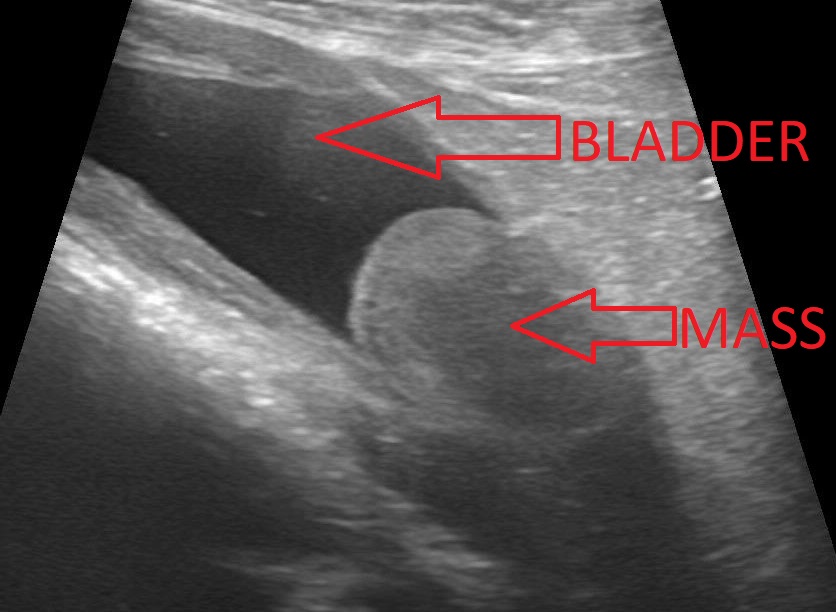
Depending on its position, the mass would randomly block the urethra, making it impossible for Madeline to urinate. Not only is this incredibly uncomfortable, it can lead to all kinds of complications including severe kidney damage.
Madeline’s owners went to several family vets and specialists to find a solution. They were told that the mass could not be removed or it would cause urinary incontinence. That it was in multiple locations in the bladder. That it was most likely cancer. And it was most likely a transitional cell carcinoma.
The only treatment suggested was radiation therapy – for $11,000. They were told that it may cause increased irritation of the bladder, which would lead to incontinence. “So the treatment could do more harm than good” explained Madeline’s owner.
She added: “We felt hopeless. Neither of us could focus on work. Every day, we would wake up not knowing if this was the day that our dog would not be able to urinate and we would have to put her down. I felt like the vets gave our dog a death sentence with no answers and no option for her to have any help whatsoever. This did not seem right to me. It did not seem ethical. We asked them desperately what they recommended and they told us if there is one thing that they could recommend, “it is not to get surgery.” They did recommend that we get her kidneys checked. Her kidneys were slightly enlarged, therefore she has no more than two weeks to live. We needed to monitor her closely to see when things got worse because then we would know when to put her down.”
The most often recommended palliative treatment for transitional cell carcinoma is a drug called piroxicam. It’s an anti-inflammatory drug, which side-effects include stomach ulcers.
So that’s what was prescribed for Madeline. Nothing else.
It is very tricky for me to write what follows, out of respect for the colleagues who were in charge of Madeline. But when solutions exist, I firmly believe that they should be offered to a loving, motivated pet owner. Then it’s their decision to accept or decline the treatment plan.
Madeline’s owner found me through my website, and they reached out for help. I had a few important concerns:
. Everybody was convinced this mass was cancerous, but there was no proof.
. No biopsy was suggested. The whole treatment plan (piroxicam) was founded on an assumption: that just because the most common bladder is transitional cell carcinoma, then that’s what Madeline had.
. And my most pressing concern: no immediate solution was offered to help her empty her bladder, which can absolutely lead to a life-threatening situation.
Madeline’s owner comments: “She went through an extended period of time being unable to urinate at all. No vet, emergency vet or specialist anywhere around us would give her immediate relief through a urinary catheter. I called Dr. Zeltzman in a panic and he immediately set us up with a clinic that would do the procedure. Luckily, she was able to urinate shortly after this and this was no longer an imminent need.”
. Surgery was completely eliminated as a solution by several specialists, including a surgeon.
So Madeline’s owners and I had a heart-to-heart discussion. After reviewing her medical record and ultrasound report, I suggested a 2-step surgery:
Part 1. Remove as much of the tumor as possible.
Yes, it was probable that we wouldn’t get it all.
Yes, it was likely that the tumor would regrow over time.
Yes, cancer was all over the bladder according to the ultrasound.
Yes, there was a risk of urinary incontinence.
But how exactly was Madeline supposed to empty her bladder with this mass blocking her urine? Trying to remove part of it would also allow sending a biopsy to the lab to get an actual diagnosis.
In addition, we’d know if piroxicam is the correct treatment.
Part 2. Then, we could offer my top-secret weapon: a solution to drain the bladder, short-term as well as short-term.
Of course, I’m joking. There is nothing secret about this solution. It’s in every surgery book.
I insisted several times that my solution “is not for everybody.” I explained that there were possible complications, such as repeated bladder infections. After several conversations, Madeline’s owners took a giant leap of faith. They went against the advice of multiple other vets, including specialists. And they asked me to put this plan into action.
WARNING – the next picture is graphic.
Prior to anesthesia, Madeline’s blood work was checked again to make sure her kidneys were functioning normally and there was no secondary issue caused by her urinary blockage. Everything came back normal and she was prepped for surgery.
Again, the 1st step was to remove the tumor. It was a little bit bigger than a dime. Small, but potentially deadly. It clearly blocked the entire urethra. It was removed as gently as possible from inside the bladder/urethra junction.
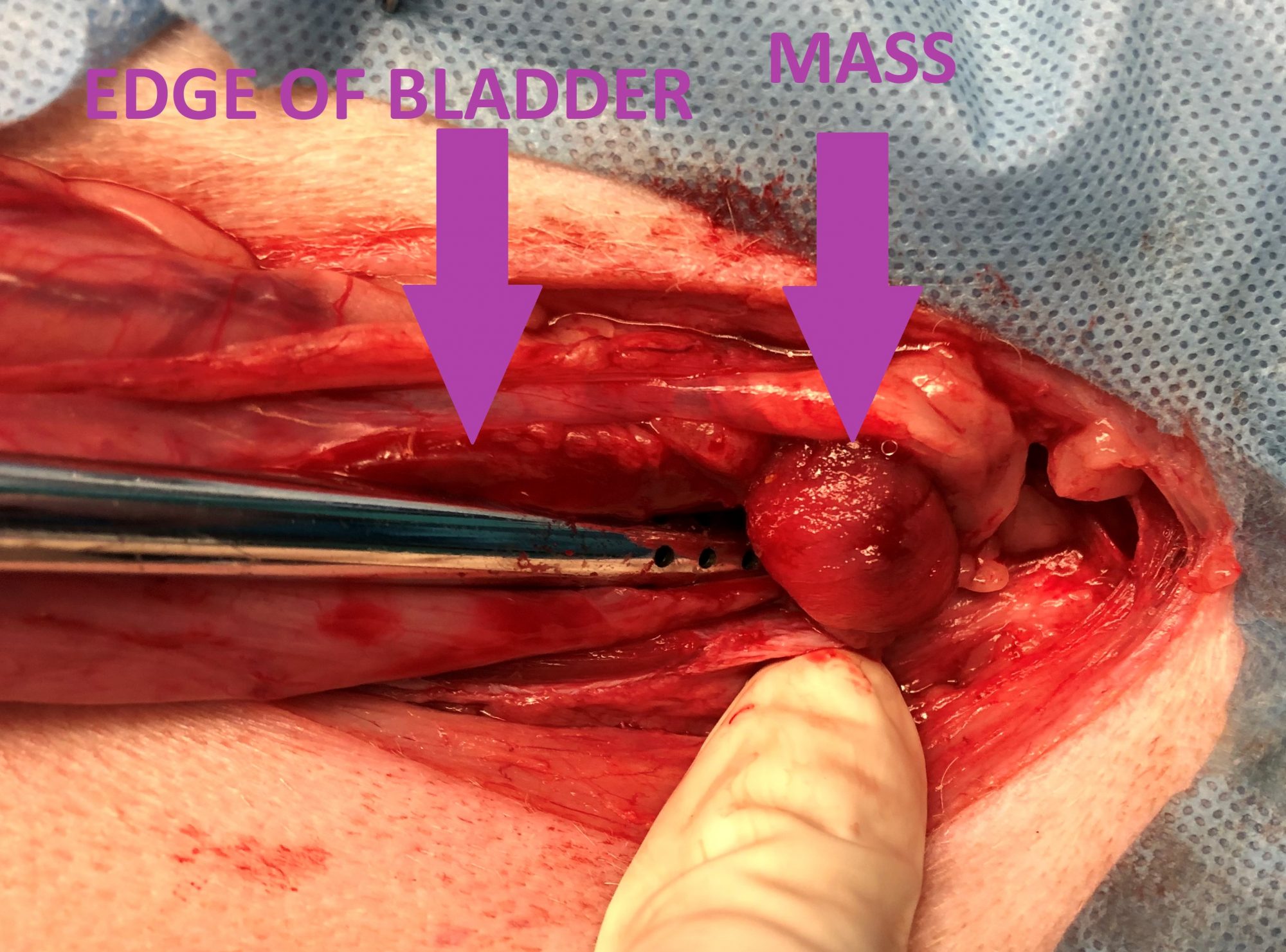
The rest of the bladder felt normal to the touch and looked normal. There were no obvious signs of spreading throughout the bladder.
Next, came my no-so-secret weapon: it’s a special tube called a cystostomy tube. This is a soft tube that is placed in the bladder and comes out of a small incision in the belly. The tube has a special valve attached to it to control the flow of urine, allowing the owners to empty the bladder as needed. The tube can remain in place in the short-term. In Madeline’s case, it may very well stay in for life.
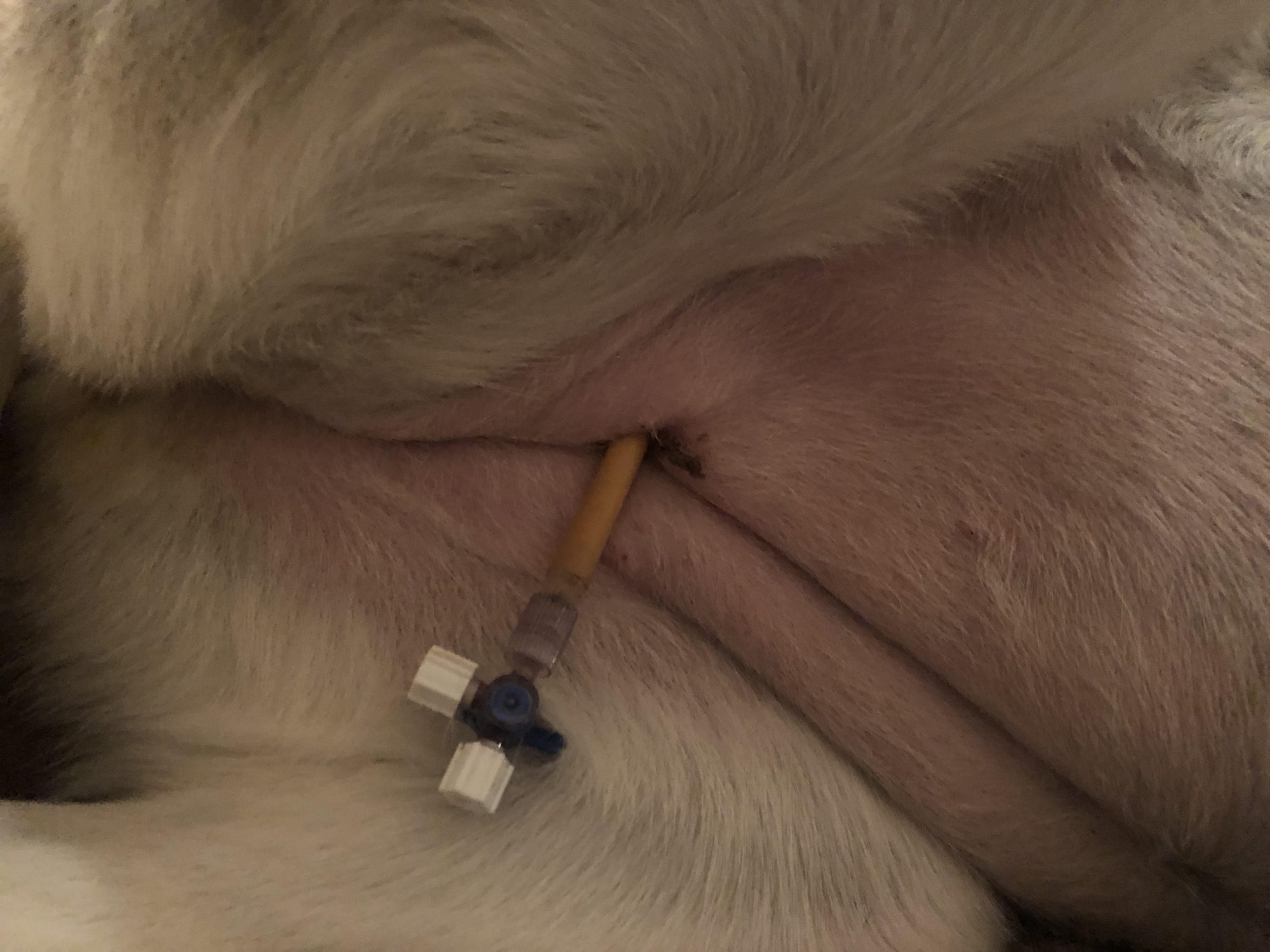
Surgery went very well and Madeline recovered smoothly. She went home after her owners were showed how to care for the cystostomy tube.
No big surprise, she was able to urinate on her own shortly following surgery, which was a relief – literally! Regardless, I instructed her owners to use the tube once a day to get comfortable with it. This way, they would be proficient at using it, the day it might be the only option Madeline has to empty her bladder…
About 1 week after surgery, the biopsy report came back. Guess what? Madeline’s tumor was not transitional cell carcinoma! Sadly, it was cancer. It is a rare tumor of the muscle of the bladder called leio-myo-sarcoma. Which doesn’t responds to piroxicam.
Amazingly, the pathologist said that we got it all – although with “very narrow margins”, which means that it is likely to come back.
A week after surgery, Madeline was doing “fantastic”. She was urinating on her own normally. Her owners “could not be happier.” They were taking excellent care of her cystostomy tube and emptying the bladder once daily as instructed.
Two weeks after surgery, the staples were removed. Her owner commented: “We’re doing great! Never happier! Madeline is doing fantastic! It is almost like she knows that her life was saved and she is showering us in kisses to show us her appreciation. She has completely adapted to wearing a cone and even carries her ball around in her cone! The incision site looks clean and dry. We’re so thrilled with how she has progressed so far. We cannot thank you enough for all you have done.”
I guess the giant leap of faith was the right decision…
Please understand that my point in sharing Madeline’s story is not to brag. My goal is not to show that I am smarter than anybody else.
My goal however, is to remind loving pet owners of a few important, simple facts (which long-time readers have read about many times before in this blog):
. Don’t make assumption when it comes to a cancer diagnosis. Lives are at stake here. Demand proof of the diagnosis – when possible. I’ve treated many “cancer” patients who never had cancer at all…
. Trust your gut. If you are not comfortable with a practice, or a vet, or a treatment plan, then get a 2nd or a 3rd opinion. Within reason of course.
. Just because you’re not a vet doesn’t mean that you can’t use your own logic. If there is a blockage, are there viable solutions to relieve it? If cancer is suspected, can we prove it? Can we find out which type before a treatment is recommended?
Madeline’s owners unknowingly did all of that. They weren’t satisfied with the lack of options to help their dog. They thought that there might be a better solution than a death sentence. Fortunately for Madeline, they were right.
We don’t know how long Madeline will be around. Bladder cancer is a serious diagnosis. To me, and to her owners, it’s not so much a matter of quantity of life (ie survival), it’s mostly a matter of quality of life. Being able to urinate freely is one of the mandatory requirements.
Madeline owner concludes: “We couldn’t be more grateful for what Dr. Zeltzman has done. Although we do know that she still has cancer, Dr. Zeltzman gave us more time with our baby. Most importantly, he gave us options while giving her pain relief.“
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

