Dr. Phil Zeltzman’s Blog
Grandpa Charlie has successful heart surgery
Charlie, a roughly 12 year old Yorkie, just wasn’t himself. His appetite was poor. His breathing was faster than normal.
His owner recalls: “Charlie lives to eat so I knew something was wrong when I couldn’t even tempt him to eat tuna!”
Blood work was fairly normal except for high sugar levels – nothing new since Charlie was a known diabetic.
Chest X-rays showed an enlarged heart.
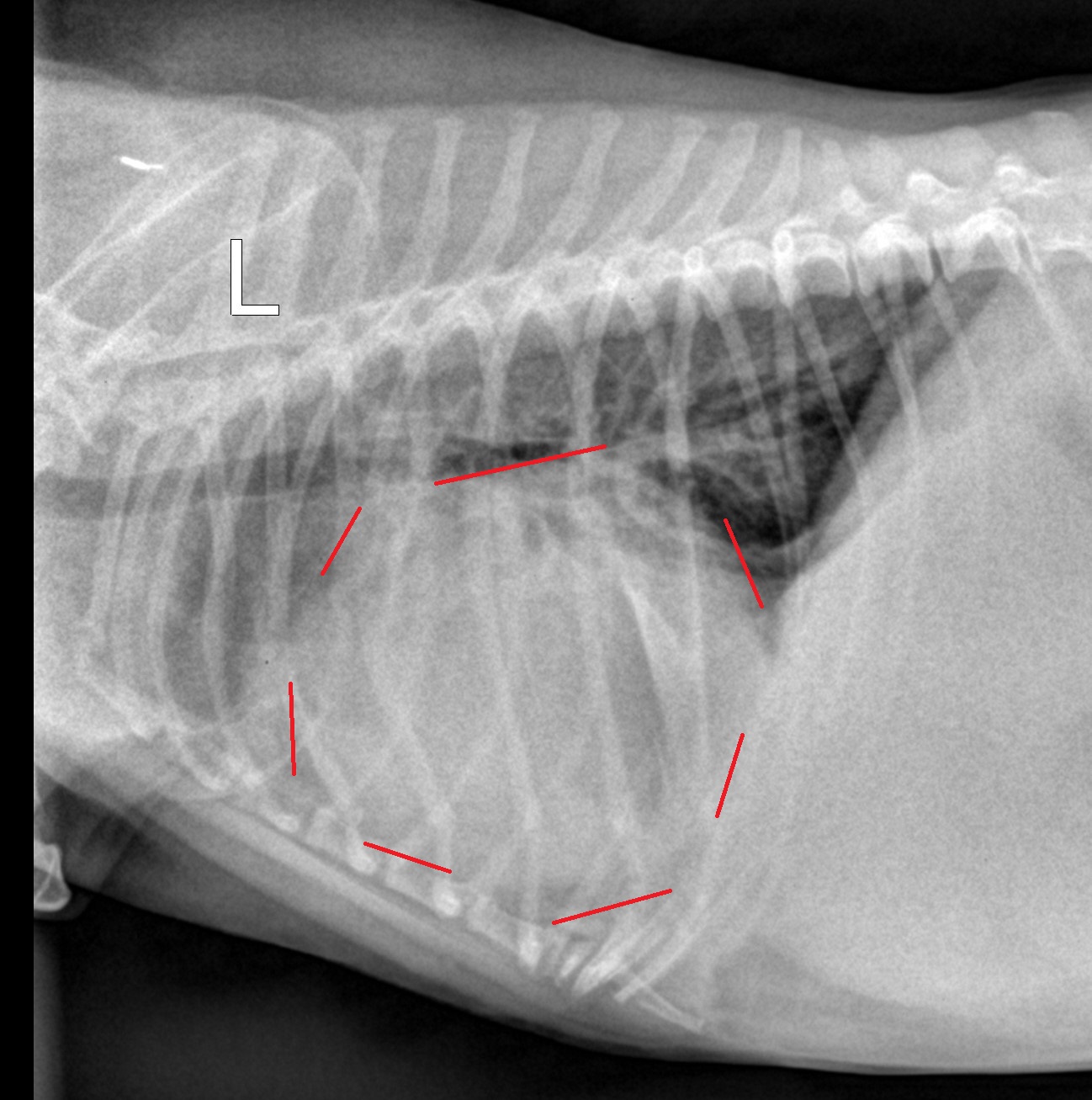
An ultrasound showed fluid around the heart. It also was suspicious for a tumor on the heart.
This is a pretty classic case of pericardial effusion.
What does that mean exactly?
The heart is covered by a sac called the peri-cardium (latin for “around the heart”). Its job is to protect and lubricate the heart, and to keep it in place within the chest.
Because this kind of tumor is fragile and very rich in blood vessels, it doesn’t take much for it to bleed.
Since the tumor is located inside the sac – the pericardium – blood builds up inside of it.
And because the sac can only expand so much, the fluid build-up eventually puts pressure on the heart.
Think of it as a bad headache or a migraine. The brain can only swell so much because of the skull around it.
This explained that Charlie didn’t feel well (poor appetite) and was out of breath.
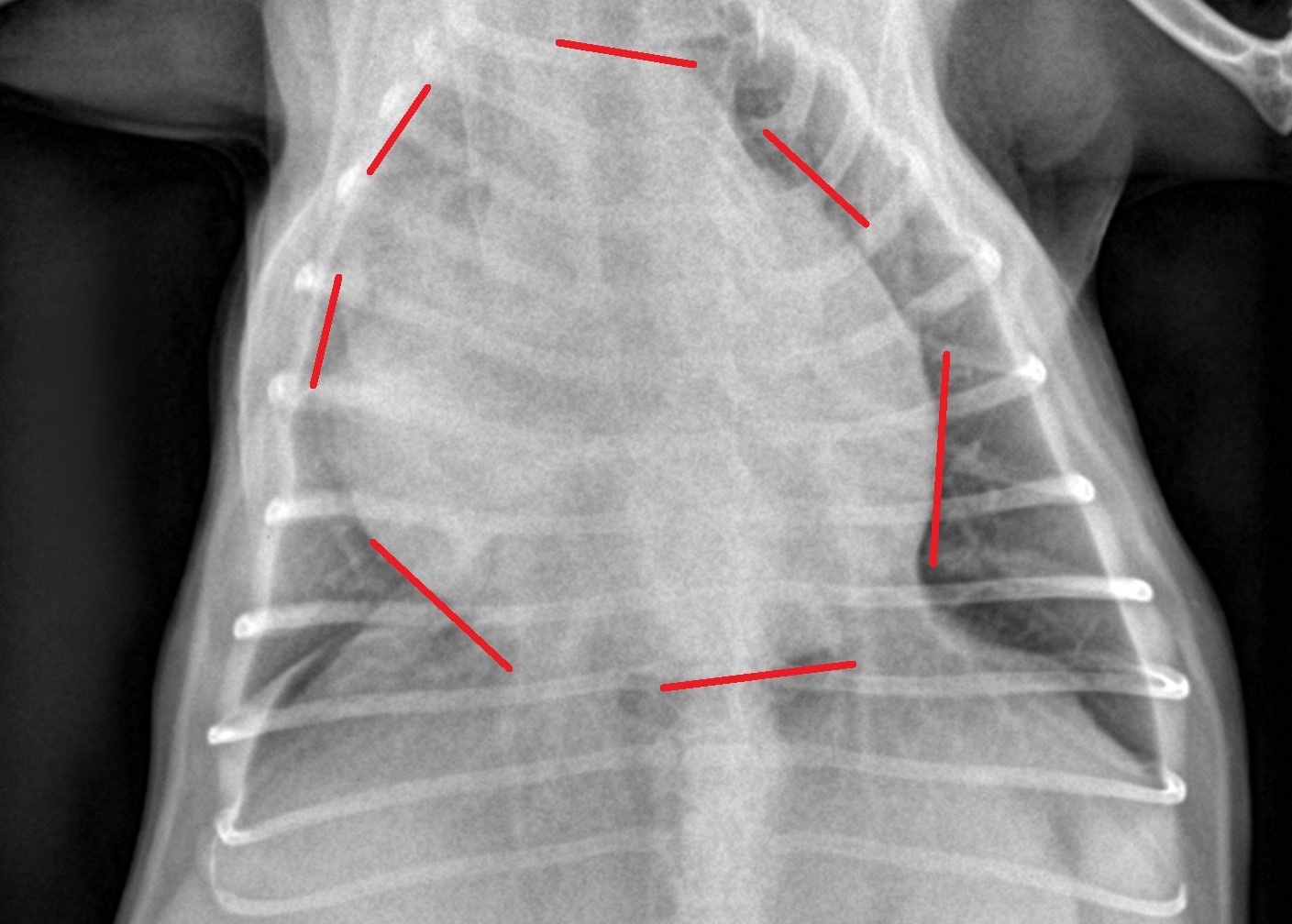
Not only was the heart feeling squeezed, but the lungs had less room to expand.
The best solution is surgery, to relieve the pressure.
Anesthesia in a 12 year old diabetic dog with a sick heart is not exactly the safest thing to do.
I went over the pros and cons of surgery with Charlie’s owner.
Who on earth chooses surgery in such an old, sick little dog?
There was no doubt in his owner’s mind that it was the right thing to do.
She believes: “Once you take on the commitment of owning an animal, they become part of your family. (Despite) the bleak prognosis, we can’t willingly say goodbye to our beloved pet. (…) Even though he may only live a year (or less) or two years more, we feel we must do all we can to prolong his life.”
And she very kindly shared: “Honestly, I felt very reassured by your discussions with me prior to surgery. You clearly laid out postop care. I felt calm the day of surgery knowing Charlie was in good hands.”
Equipped with such positive vibes, and despite the risks, we took Charlie to surgery.
After an incision on the left side of his chest, between two ribs, a large section of the pericardium was removed.
ASSUMING YOU HAVE THE STOMACH FOR IT, you can watch the short video below.
As my wonderful nurses can attest, watching a beating heart is one of the coolest things we see, but I understand it is certainly not for everybody!
Before removal of the pericardium, the heartbeat is typically harder to see, because the heart is surrounded by the pericardium and lots of blood. In this video, that is not really the case, because a lot of the blood inside the sac had been removed with a needle to provide relief to Charlie.
After removal of the pericardium, a surgery called a peri-cardectomy, the heartbeat is easier to see, because there is nothing restricting it anymore.
We then needed a way to remove free air from the chest. This is done with a device called a chest tube. You can see a glimpse of it at the end of the video, on the left side of Charlie’s body. It only stays in place for a short time after surgery, and can be removed once there is no more air and not too much fluid left to remove.
After the chest tube was secured, the rest of the chest was stitched up.
Then it was time to transition from the OR to ICU.
Little Grandpa Charlie recovered from surgery and anesthesia very smoothly.
In fact, minutes after coming out of the OR, he looked surprisingly good and comfortable. I was so impressed, that I took a video of him (see link above). Of course, he’s in a daze because he went through a lot and he was high on doggy morphine, but he still looked amazing so soon after surgery!
This is a great testament to the wonderful anesthesia nurse who took care of Charlie. Anesthesia is always a bit more challenging when we do open chest surgery, especially in a patient with a compromised heart.
Even more encouraging, Charlie ate dinner the evening of surgery, for the first time in days!
Who eats a few hours after open chest surgery?!
The chest tube was removed the very next day.
After a few days on heavy duty pain medications and lots of TLC, he was able to safely go home.
His owner remembers: “I didn’t see Charlie for several days after surgery. When Charlie did come home, he had the cone on, but he seemed to almost be his old self. He didn’t seem like he was in pain (we gave pain meds anyway!). He ate and drank fine. When going potty, he was eager to do more, wanting to get back to his walks – though we said not yet!”
Charlie is very lucky his owner didn’t procrastinate and trusted her guts based on what were after all (seemingly) very minor signs.
Remember, all there was is a decreased appetite and faster breathing, that’s it!
She recalls: “I just had a bad feeling and knew things weren’t good. He just wasn’t acting like himself and I worried he was in pain.”
It’s only been 2 months since surgery, but so far Charlie is doing great.
His owner writes: “Charlie is doing marvelously well! He is eating, drinking and has a happy demeanor. He seems comfy and happy! Overall, the experience went very well and all of our fears have been alleviated. We have our energetic Yorkshire Terrier back!
And her final words of wisdom:
“The day will come when we won’t have a choice anymore and we will have to say goodbye. But for now, and thanks also to you, that day is not today. Some beings and their life/memories with us are more important than $!”
If you would like to learn more about how your pet can have safe surgery and anesthesia, contact us through www.DrPhilZeltzman.com
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What you need to know about broken bones
We repair a surprisingly large number of fractured bones (aka broken bones).

They can happen at any age. We’ve surgically treated a 3 week old pup and a 23 year old kitty.
Virtually any bone in the body can sustain a fracture: skull, vertebrae, legs, pelvis, tail, ribs… no bone is spared!
Just in the past 3 weeks, we’ve had:
. 3 dogs who jumped out of the car window
. 1 dog who jumped off the couch
. 1 dog who was attacked by another one.
. 1 dog who was hit by a car.
And that’s just in 3 weeks!
This blog was written to:
. inform you about how fractures happen.
. tell you how they are commonly repaired.
. help you prevent them.
How do bone fractures happen?
Here are the top 10 reasons (in no particular order):
Falls
Cancer
Gunshot
Hit by car
Fights/Bites
Malformation
Jaw – Bad teeth
Bone deterioration
Fatigue (repeated trauma)
Various traumas (slipping on ice…)

How do we repair bone fractures?
There are multiple types of fractures and multiple ways to repair them. Let’s go over the most common ways.
But wait, not all fractures need surgery.
Some will simply heal with rest, time and pain medication.
Occasionally, healing can be attempted with a splint – a type of bandage reinforced with a molded piece of plastic (I am not too fond of casts…).
The challenge is to know which fractures can predictably heal with a splint.
For example, fractures of the forearm (radius & ulna) and shin bone (tibia & fibula) in small dogs don’t heal well with a splint, and most need surgery. This is a common misconception.
Many fractures require surgery.
There are 2 main ways to fix a fracture:
. with internal fixation, where no implant can be seen outside the skin.
. with external fixation, meaning that the implants are visible from the outside. This is called an external fixator.
- Plates and screws
The most common type of repair involves a bone plate and some screws. A plate is a flat stainless steel bar with holes, designed to keep the pieces of bone together while the fracture heals. The plate is attached to the bone with stainless steel screws.
Plates have different shapes, thicknesses, widths and lengths. The number of screw holes varies accordingly.
So a Yorkie with a forearm (radius) fracture may need a small 6-hole plate, and a Lab with a complicated thigh bone (femur) fracture may need a big 12-hole plate.
Therefore, a surgery practice must stock a variety of plates, since we need to be prepared to help a kitten as well as a Great Dane.
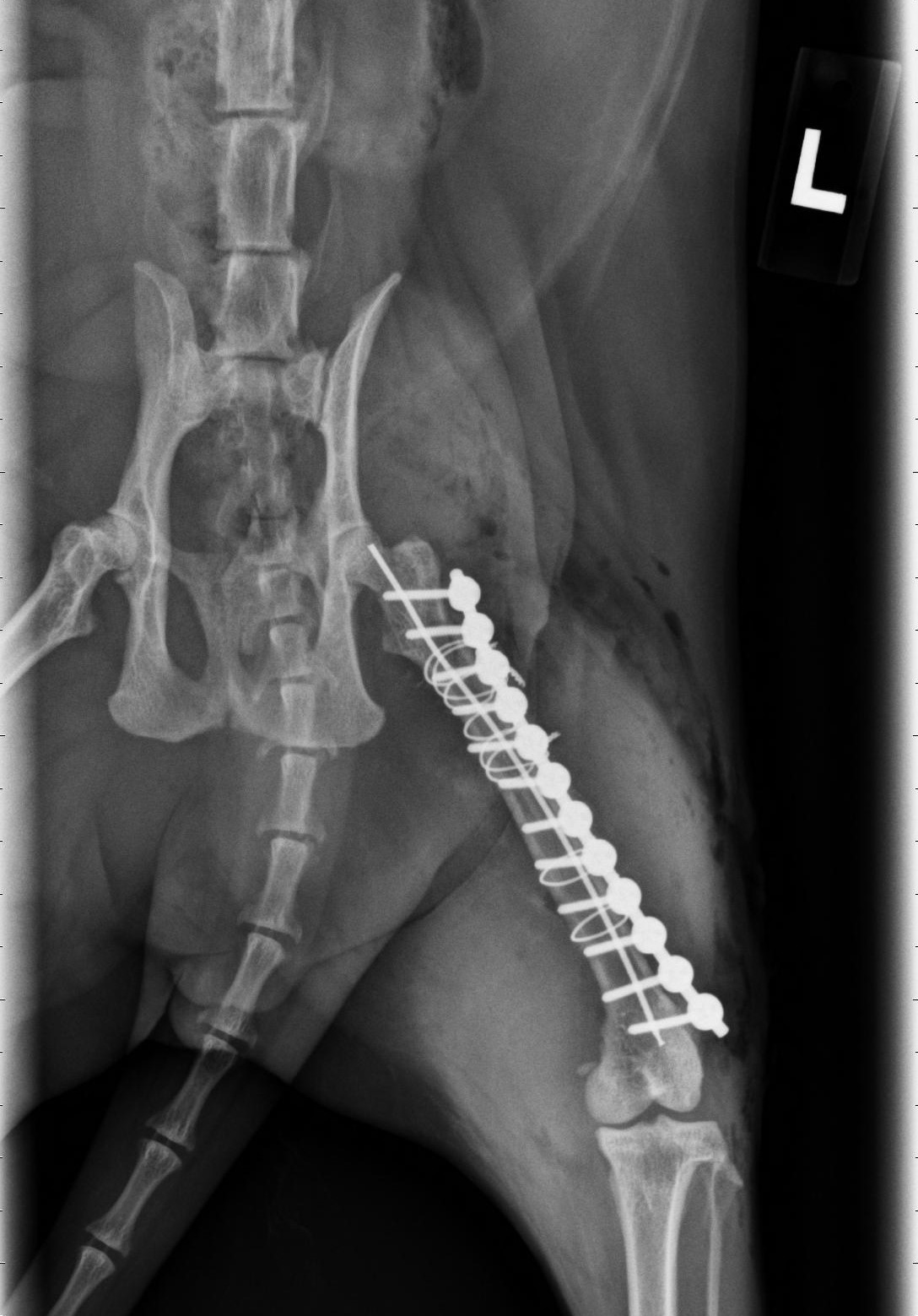
- Wires
To help reconstruct a bone that is in several pieces, we sometimes need the help of stainless steel wire (“cerclage wire”).
Some wire is placed around pieces of bone, and the ends are twisted, like a twisty-tie on your bread.
- Pins
Pins look like knitting needles. They come in various lengths and sizes.
They are used to connect one piece of bone to another. Pins are used in very specific cases, either to reinforce a plate and screw repair (see above), or as the main repair (see below).
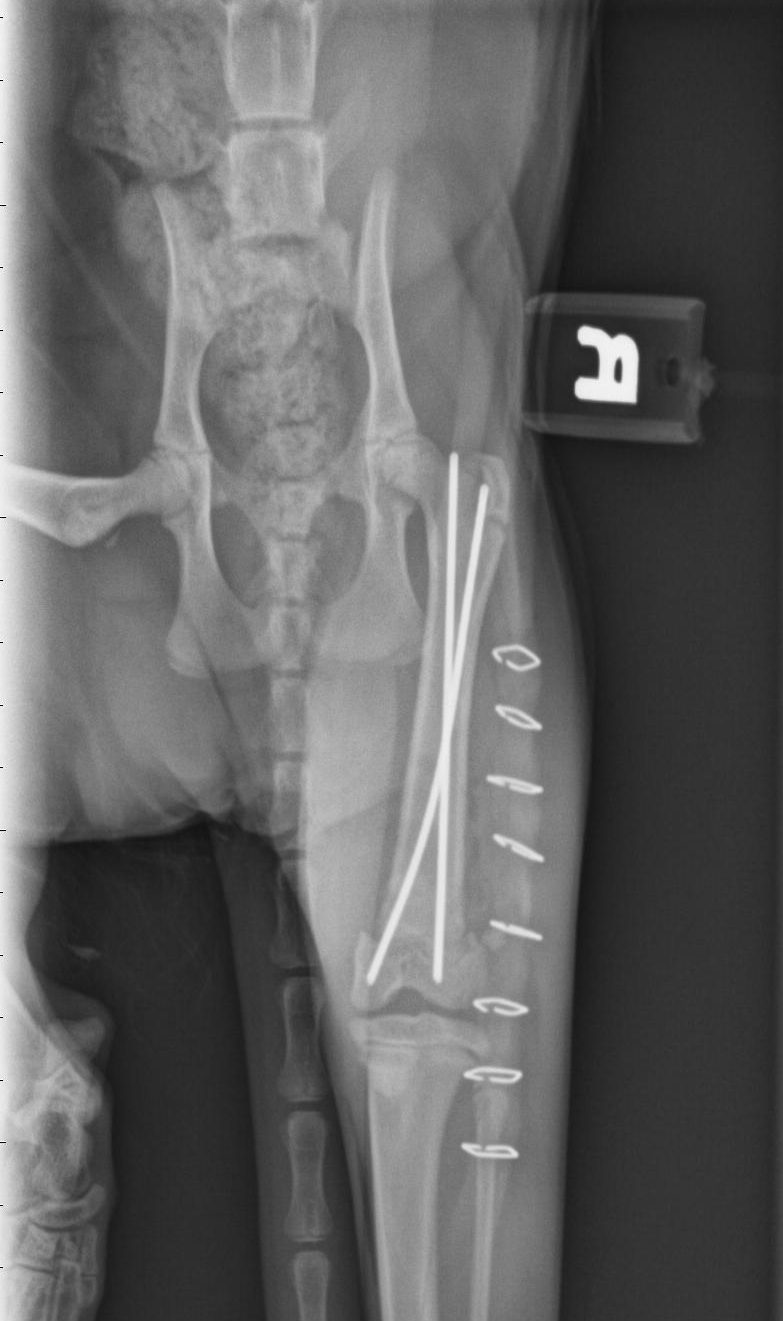
Again, all the implants described above are used under the skin, so they are used for “internal fixation.” Once the surgeon is done, the skin is sutured, and you can’t see anything stick out. These implants are typically designed to stay in forever. Only if they cause problem would we remove them.
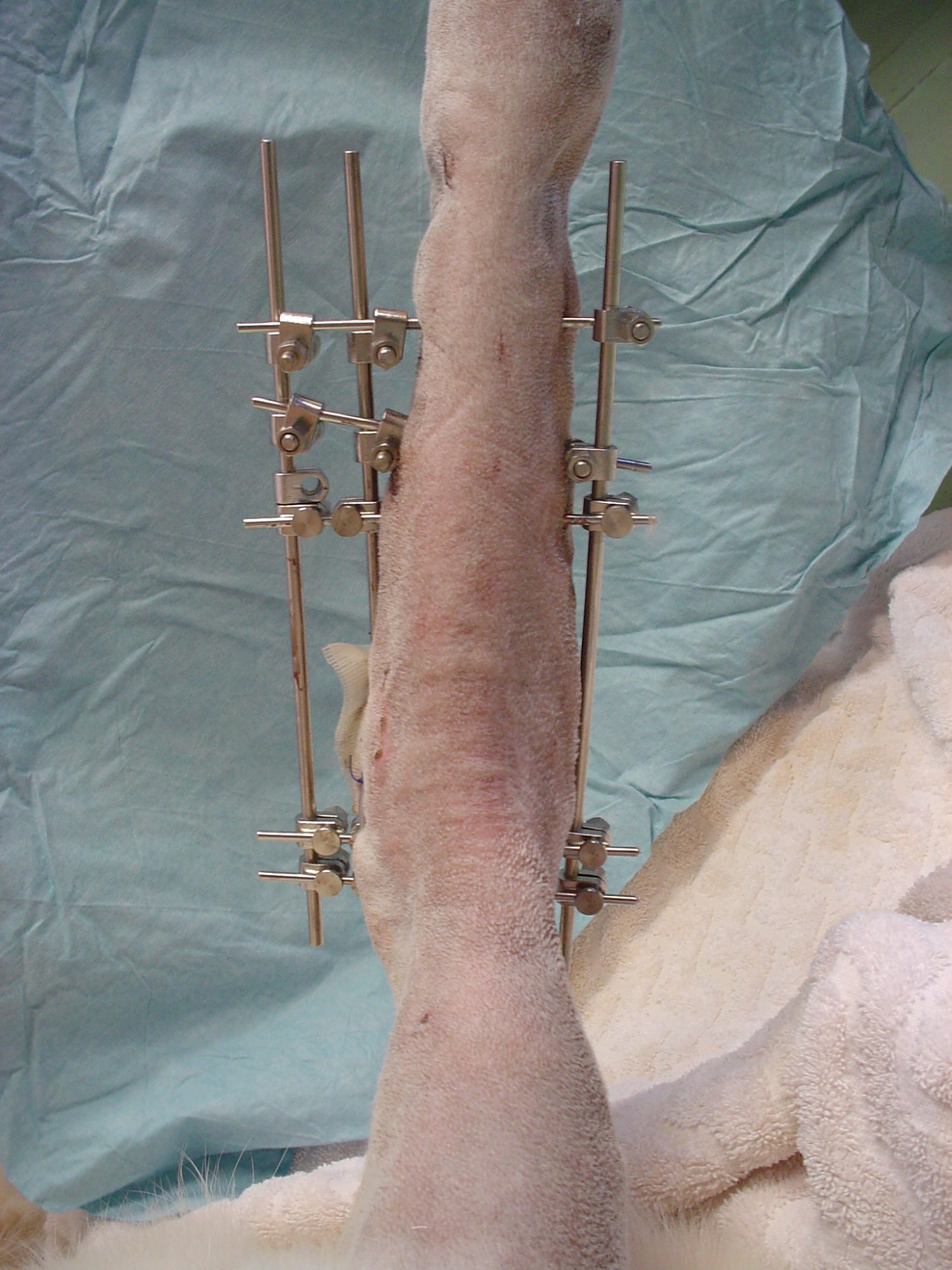
- External fixators
In some cases, such as bad gunshot wounds, we prefer using “external fixation.”
There are different types of external fixators, but here is the concept: several pins are placed through the skin, into the broken pieces of bone.
Then a big metal bar, or some other device, is used to connect all the pins. By keeping the pins together, we indirectly keep the pieces of bone aligned, which helps them heal.
To avoid infection, the holes in the skin must be cleaned regularly, e.g. with hydrogen peroxide.
Because it is external to the skin, the fixator must be removed after the fracture is healed. This is typically a quick procedure under heavy sedation or brief anesthesia.
How can you prevent bone fractures?
As always, prevention is the best medicine. Not every fracture can be prevented. Accidents do happen.
Some dogs sustain a fracture while playing in the back yard. Some cats get a fracture while playing indoors. As sad as it is, that is nobody’s fault and simply cannot be avoided.
Many could have been prevented. Several easy ways come to mind:
– Keep your dog on a leash when outdoors to decrease the risk of getting into a fight or being hit by a car.
– Keep cats indoors.
– Keep dogs inside a fenced-in yard.
– Don’t let small dogs jump from your arms or furniture. They can get very common fractures of the forearm or the elbow.
– Never let your car windows open to allow your dog to enjoy the wind and the smells. Remember, we saw 3 dogs who jumped from a car window in the past 3 weeks. All 3 owners swore that they had done it multiple times and they had never jumped before. Which is true… until they did.
Fractures can be painful both to the patient and the owner’s finances. Luckily, most fractures can be repaired and most pets can ultimately lead a normal, happy, comfortable life.

Postop care:
Depending on the fracture, the type of repair and the pet, you might need:
. very strict confinement, on ground zero, in a large crate or a small room, most often for 2 months.
. weekly splint changes if needed.
. regular X-rays to assess healing of the bone.
. pain medications and antibiotics.
. short leash walks for elimination only (for dogs).
. rehab once the bone has healed, to transition to normal life.
Then they can go back to their interrupted agenda: the squirrel herder, the keeper of the couch, the bird chaser, the flower bed destroyer or the overall ruler of the back yard.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How Yoda lost his tail
Yoda was a healthy 4 year old French Bulldog with one ongoing, itchy, painful, smelly issue…

He had frequent skin infections around his crooked little tail.
As in many Bulldog type dogs, Yoda had a “screw tail,” also called “corkscrew tail,” “ingrown tail,” or tail fold dermatitis.”
The problem with this condition is not the tail itself, but the issues the malformation creates. The malformed tail creates skin folds that become infected.
The skin folds are not exposed to air and they create a moist, dark, warm environment – heaven for all kinds of nasty bacteria.
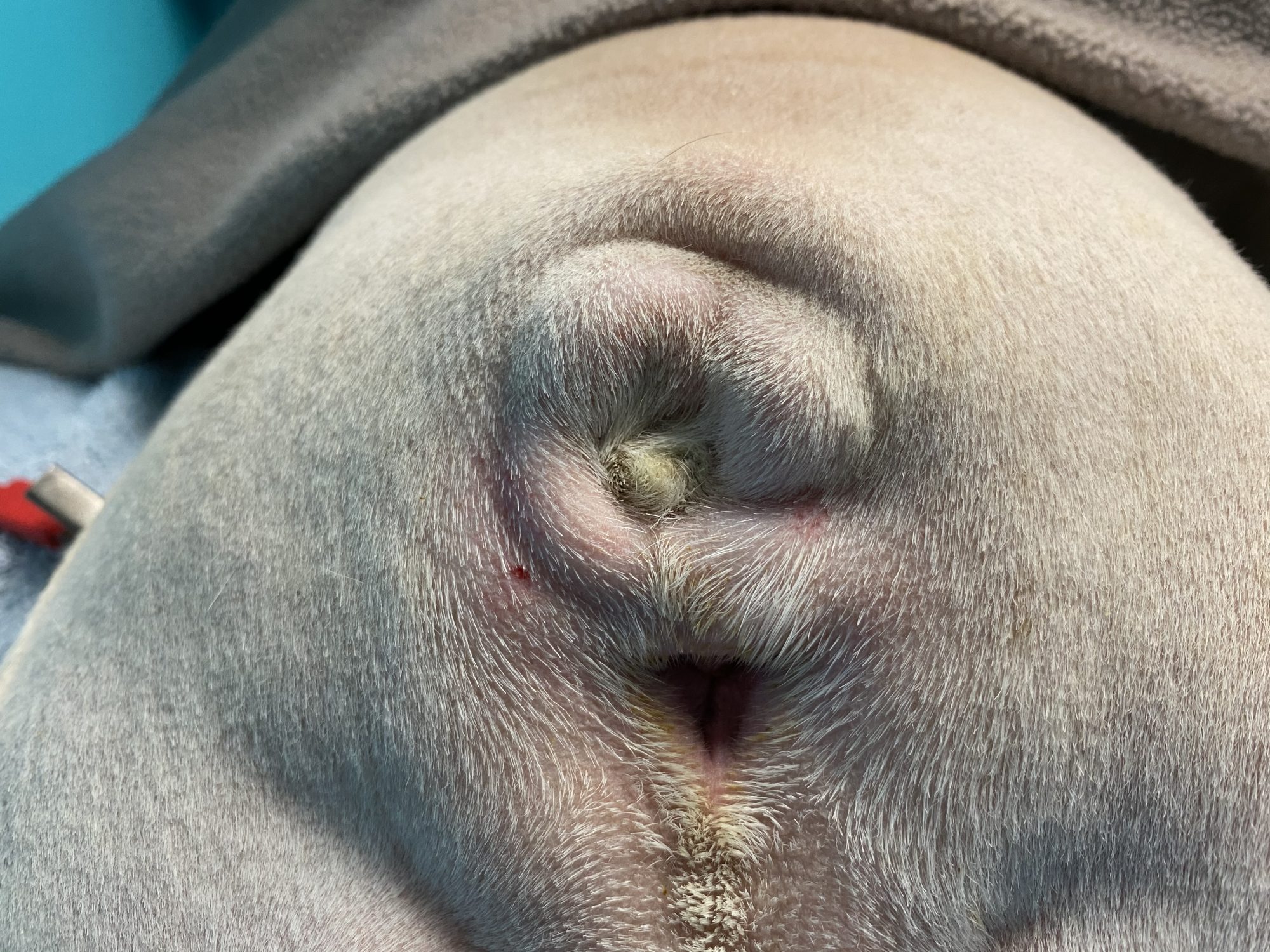
Mild cases of screw tail can be treated medically or conservatively with proper hygiene & daily cleaning.
Unfortunately, despite Yoda’s family vet’s and his owner’ best efforts, nothing helped.
This is a classic, vicious cycle with no end in sight. Antibiotics didn’t work. Antiseptics didn’t work. Pet wipes didn’t work.
Most of the clients I see for this problem are frustrated after months to years of unsuccessful treatments and impressive veterinary bills.
So what’s the solution?
The only permanent solution is to remove the “screw tail.”
The goal of surgery is to remove the malformed part of the tail and the entire infected skin fold.
The end result: no more dark, moist, warm environment for bacteria to thrive in.
This is a fairly technical and sometimes challenging procedure, which is often performed by a board-certified surgeon.
There are a few risks to be aware of:
. Patients with a flat face (brachycephalic breeds) have a higher risk during anesthesia, so an experienced anesthesia nurse is critical.
. We have to work in a filthy area, both because of the infection in the tail fold and because of the proximity of the anus. We certainly scrub the skin as thoroughly as possible, but there is always a mild risk of infection.
. There is a delicate balance between removing too much skin and not enough. Not enough skin leaves infection behind, so there is potential for complications. Too much skin taken away can lead to difficulty stitching up the skin nicely.
. Fecal incontinence is a complication that is often mentioned, but that is a low risk in the hands of an experienced surgeon.
. After surgery, some patients drag or scoot their hind end, which can result in damage to the incision and poor healing.
The outcome is typically very good with proper postop care.
Yoda did great during his procedure. He recovered smoothly from anesthesia and surgery.
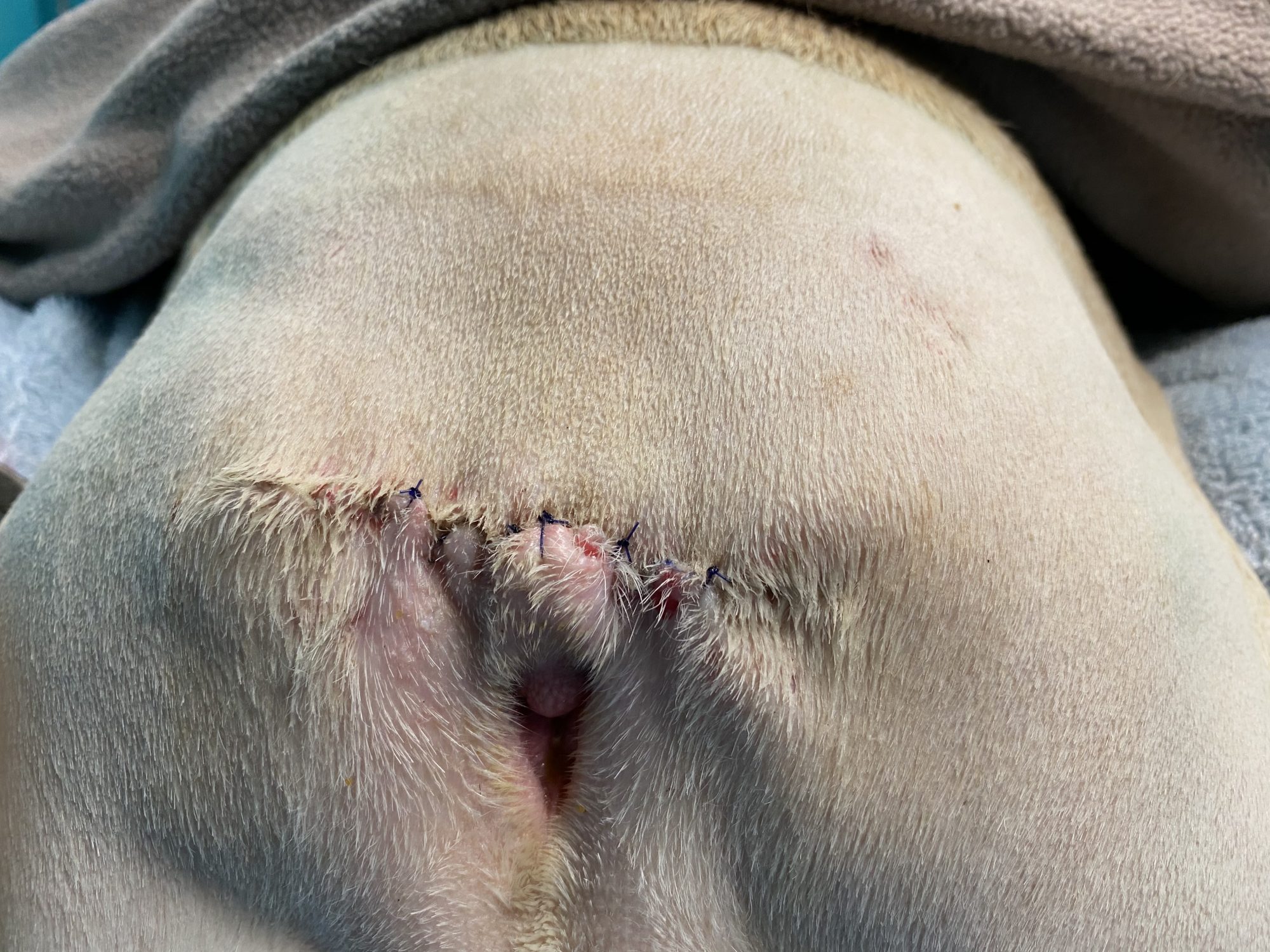
After 3 weeks of TLC, his owner reported that Yoda was doing well at home.
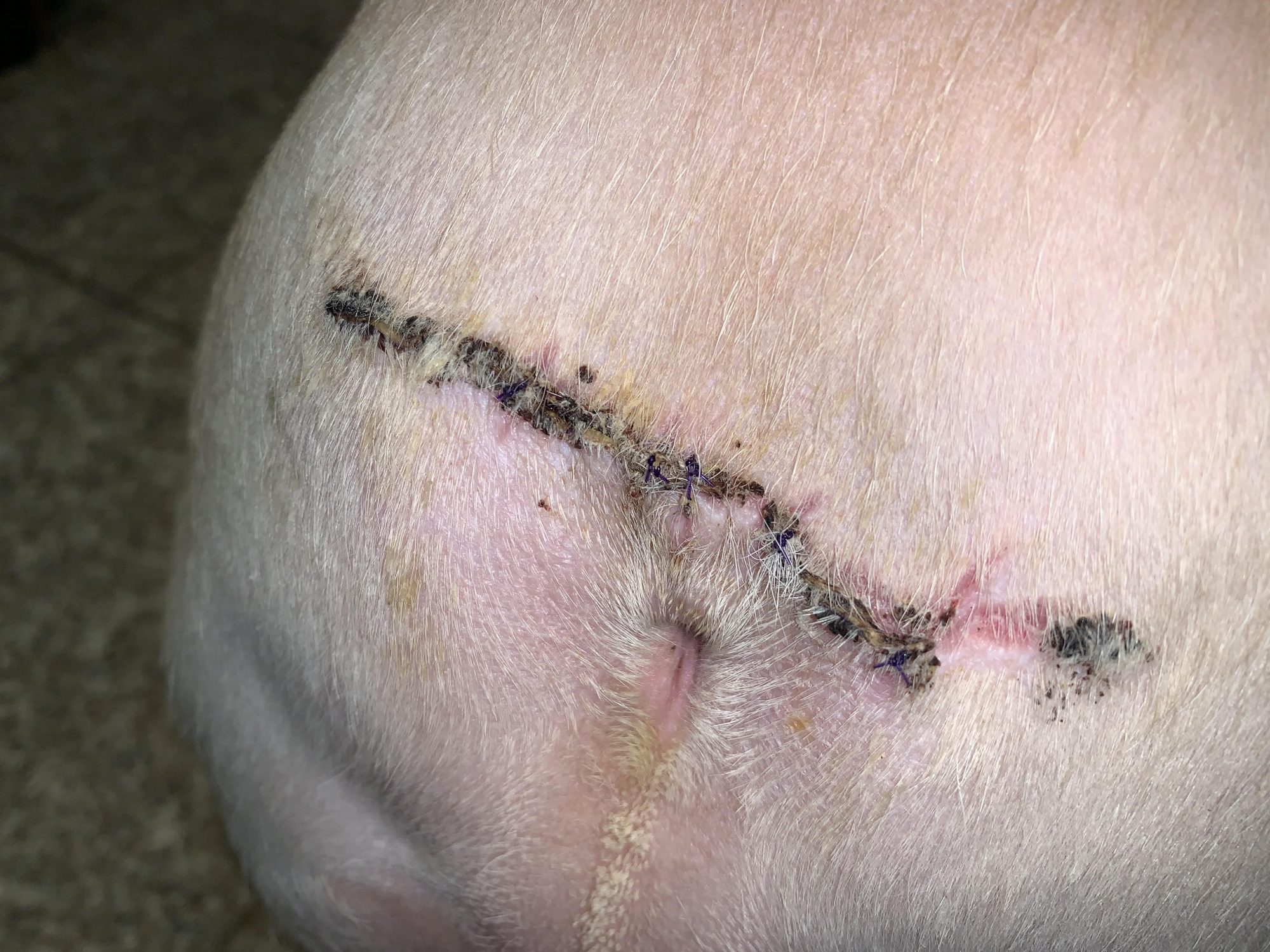
No more smell, no more itching, no more scooting, no more soreness.
Just pure Bulldog happiness, and a happy, wiggly behind.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What caused Kona to lose a kidney?
Kona, a female Lab, was only 1 year old, yet she had had several bladder infections.

Rather than keeping her on repeated antibiotics, her family vet looked into the situation and discovered that Kona had an extra fold over her vulva.
This common (and under-diagnosed) condition is called a “redundant vulvar fold,” “vulvar fold dermatitis,” “recessed vulva” or “hooded vulva” (see below a picture in another patient, a 6 year old Newfie, where the vulva is barely visible).
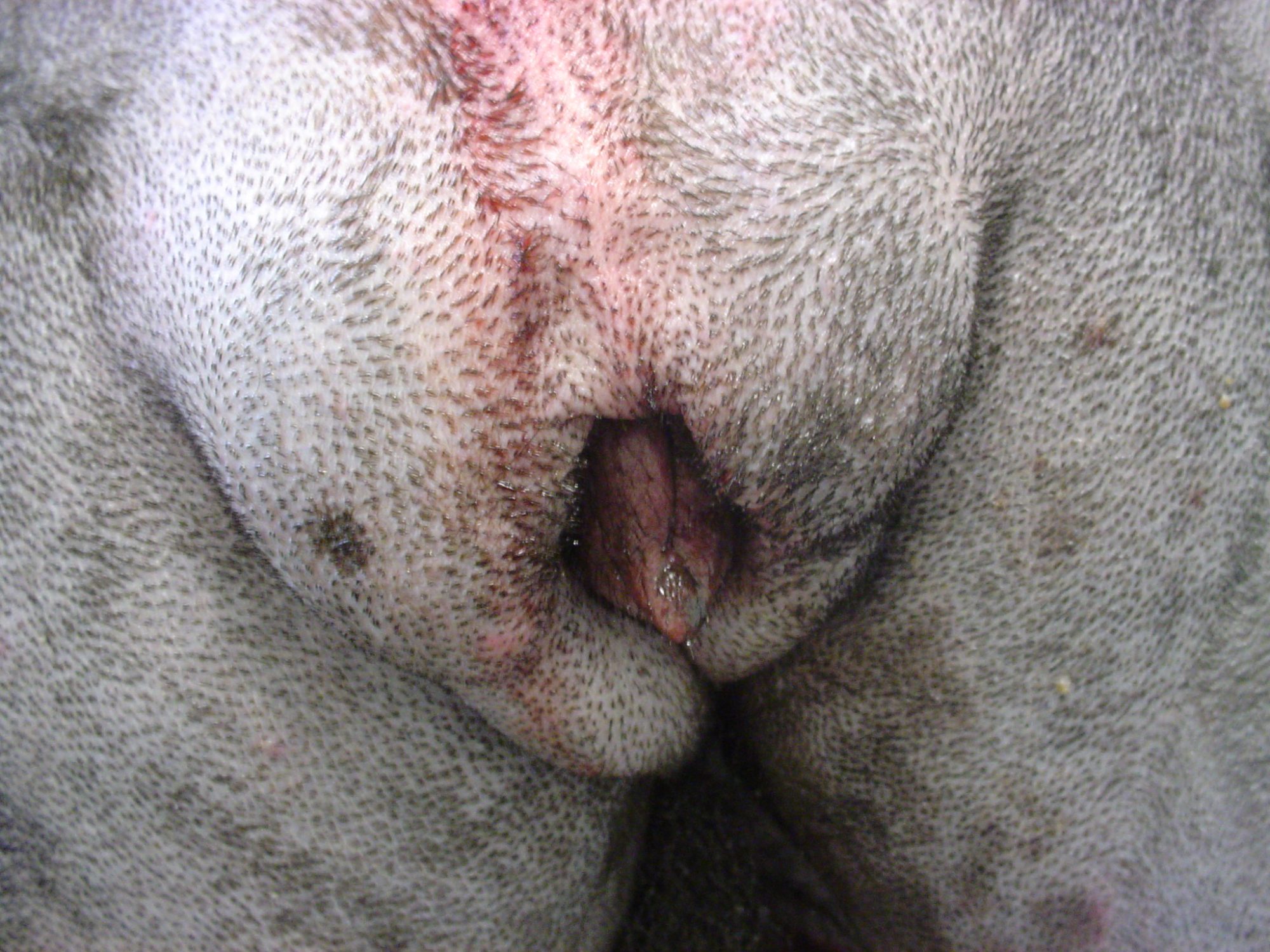
The treatment is a reconstructive surgery called vulvoplasty or episioplasty. The goal is to remove the extra skin.
The main challenge is to remove just the right amount. Not too little, and not too much.
Kona’s pet owner wisely chose to have her spayed under the same anesthesia. Her vet asked me to look into the possibility of a malformation of her urinary system called an ectopic ureter. The ureter is the tiny tube between the kidney and the bladder.
It was a possibility because Kona was constantly leaking urine, i.e. she was incontinent.
During surgery, we removed the extra skin fold, spayed her, found no ectopic ureter… but found another condition.
She had a hydro-ureter, i.e. a ureter that was huge, about 5 times bigger than on the other side. This required removing it, and sacrificing the kidney on the same side – of course after calling the owner in the middle of surgery to request permission to do so.
Surgery was uneventful, and Kona recovered smoothly from anesthesia.
Here is a (warning, graphic) picture of the kidney and the enlarged ureter (hydro-ureter) in another patient, a 6 year old Malamute.
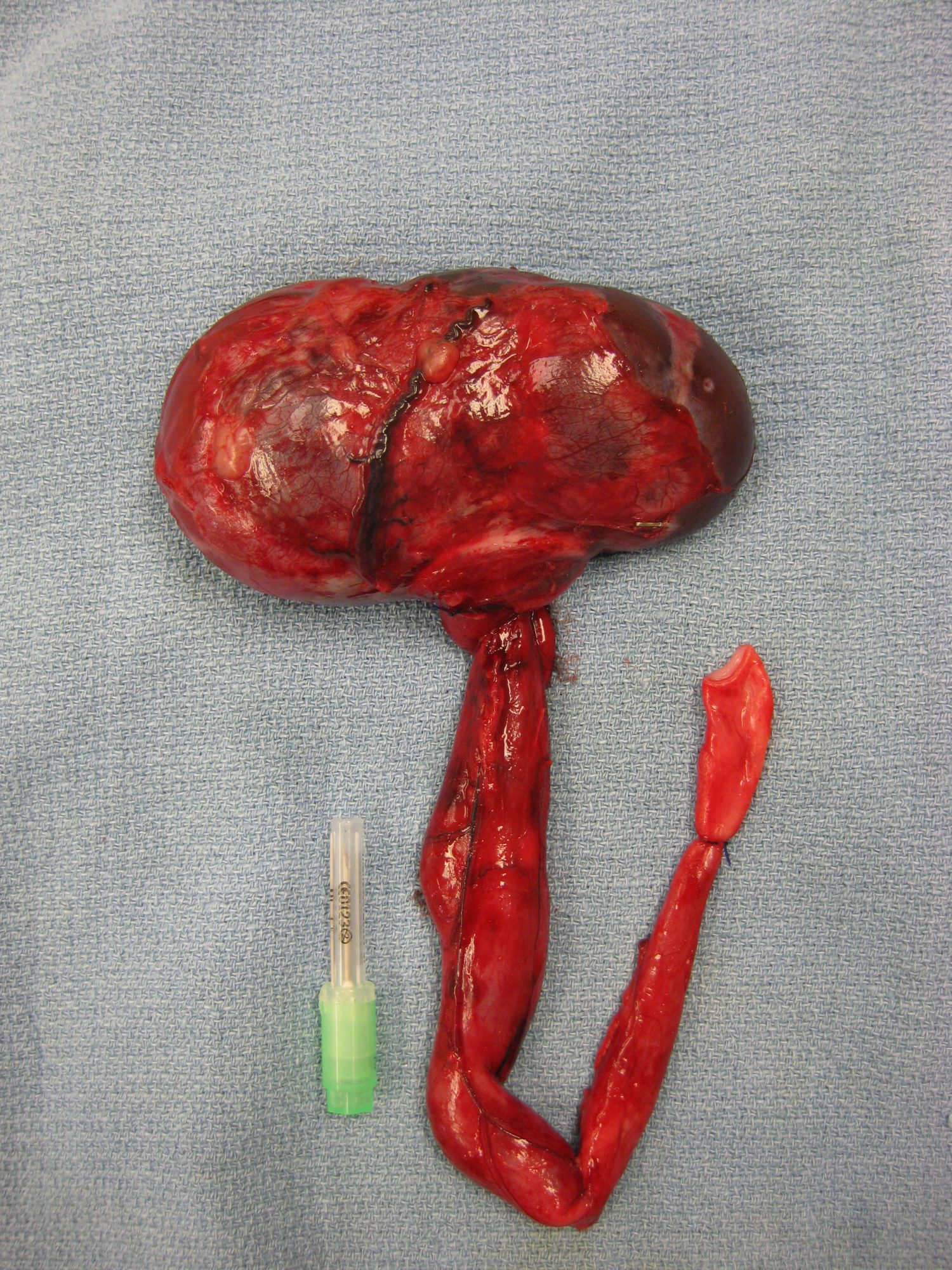
Three weeks later, her owner EB writes:
“Kona is doing well. I have not noticed any leaking and when she urinates, it is a steady stream. Her incision looks great and she is her spunky self.”
Obviously, this is an unusual situation, but a good reminder to keep an open mind when a patient has an unusual situation, like leaking urine constantly.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
A LOOK BACK AT 2021…
A LOOK BACK AT 2021…
The beginning of a new year is a great time to reflect on past accomplishments. For me, as a surgeon, it includes thinking of all the patients we helped and which surgeries we performed the most.
This can give you an idea of which surgeries pets are most likely to need…
So here were our top 10 surgeries in 2021.
1. ACL SURGERY
It never fails.
ACL surgery remains the most common surgery we perform, mostly in dogs (and less so in cats).
We have different procedures in our toolbox depending on the patient.
. TPLO (Tibial Plateau Leveling Osteotomy) is THE most common surgery we perform, by far.
. The “traditional” technique with heavy nylon sutures can be used in well-selected dogs (and occasionally in cats).
. The TWO (Tibial Wedge Osteotomy) has come in handy a few times this year in dogs who had implants that prevented doing a TPLO, or who had extremely steep angle at the top of their shin bone.
. TTA (Tibial Tuberosity Advancement).
One size doesn’t fit all here. We don’t see every problem as a nail, and we don’t only have one hammer.
2. Mass removal
We’ve removed masses in and under the skin, in the chest, in the bone (legs, toes, jaws)…
Thankfully, not all tumors are cancerous, and we’ve removed many benign masses.
3. Belly surgery
Belly surgery or “exploratory laparotomy” allowed us to:
. remove foreign objects from the stomach
. remove body parts (gallbladder, spleen, adrenal gland)
. take biopsies
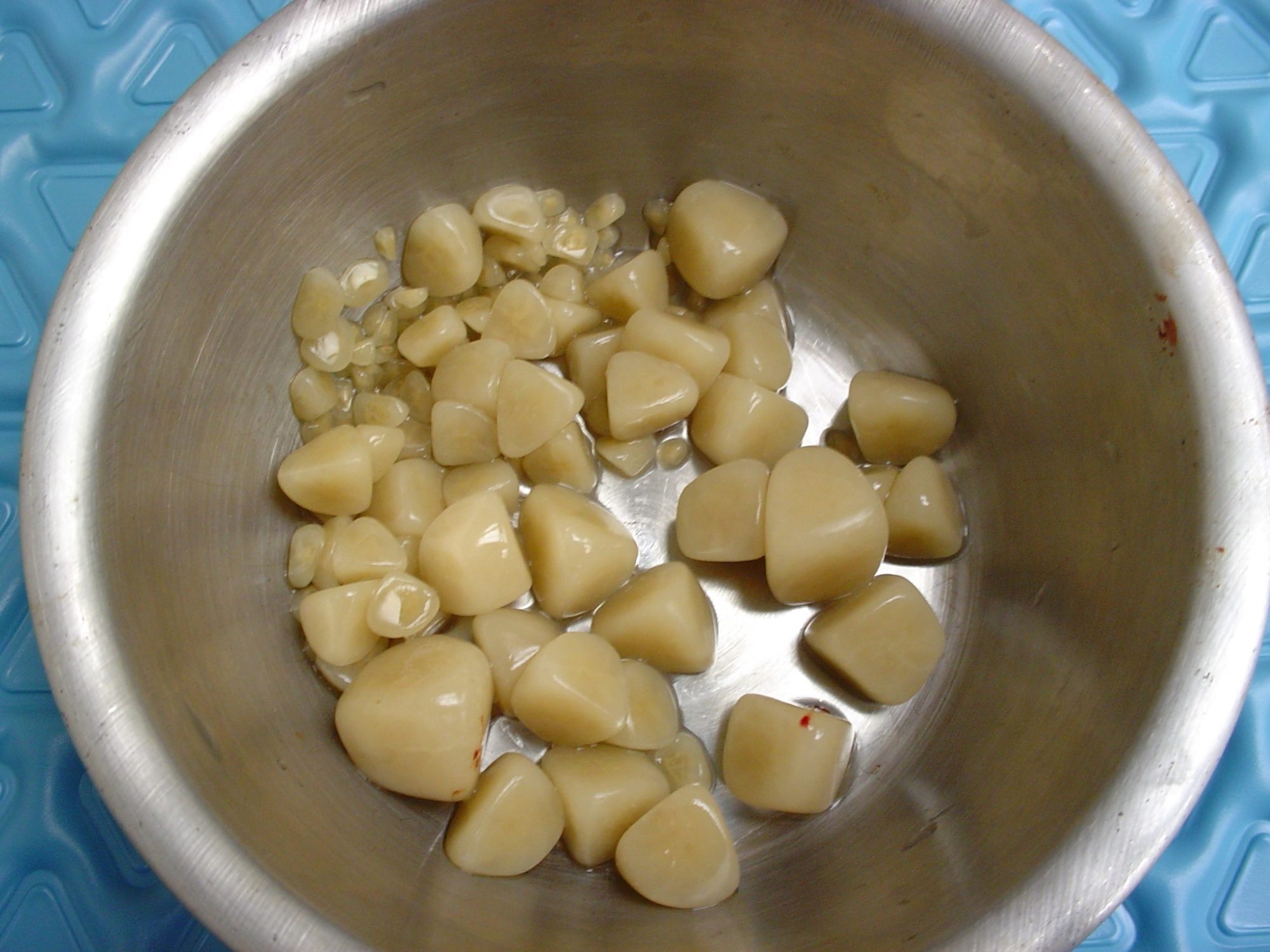
. remove bladder stones, etc.
You can read about bladder stone surgery here:
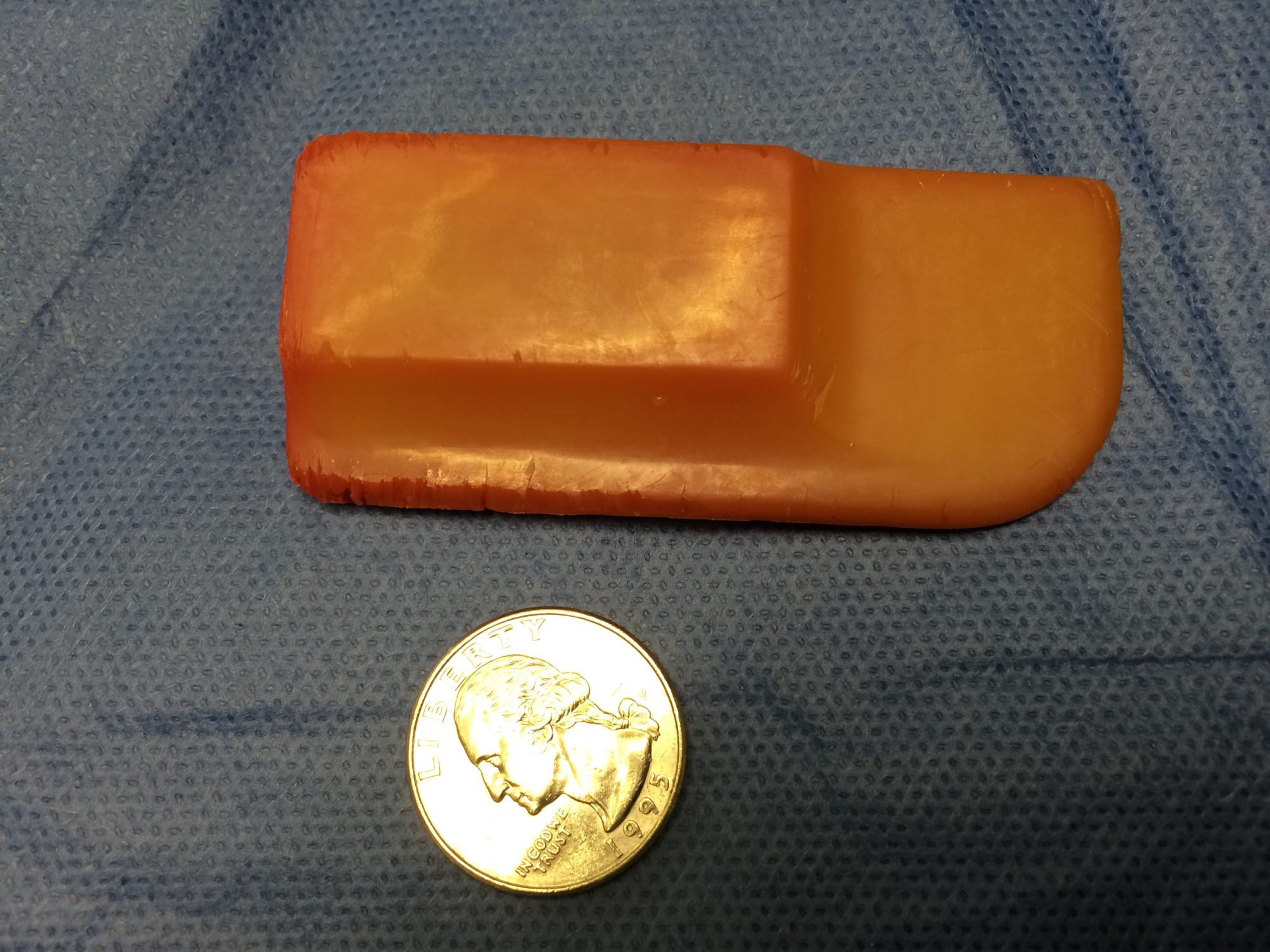
Some cats had their colon removed because of a serious condition called megacolon. This is the only definitive solution when cats are so severely constipated, that the colon has become a painful giant bag of dehydrated poop. At that stage, medications are a waste of time and money.
Procrastinating to move on with surgery invariably leads to a much worse anesthesia candidate. These cats may go from otherwise healthy to skinny and unhealthy. Not to mention the fact that they suffer from untreatable constipation.
We also performed a number of prophylactic gastropexies, a preventive procedure designed to present stomach twisting in dogs at risk for “bloat.” This life-saving procedure should be considered in Great Danes (the #1 breed for this disease), German shepherds, Labs and several other large dog breeds.
4. Joint dislocations
We’ve mostly treated joint dislocations in the hip and the knee. Some pets had trauma, others were born that way (congenital dislocation).
The most common one is the kneecap dislocation. The kneecap slides out of the groove where it is supposed to live, at the bottom of the thigh bone (or femur). It is common in dogs, and we’ve treated a few cats with that condition last year.
5. Fractures
We’ve fixed fractures in just about every bone this year, mostly the forearm (radius), the shin bone (tibia) and the thigh bone (femur), as well as some toes, the jaw and the arm (humerus).
To fix these broken bones, we’ve used plates and screws, pins, or a device called an external fixator.
Causes of broken bones mostly included jumping, falling or being hit by a car.
6. TECA
Total Ear Canal Ablation (TECA) is the only definitive treatment for dogs (most often Cockers) and cats who have never-ending ear infections. They lead to pain, head shyness and sometimes aggressiveness.
Unfortunately, most of these pets are treated with medications for years, which can’t even go down into the ear canal because it has become so swollen.
We occasionally perform a TECA in pets who had a tumor in the ear.
TECA is an invasive procedure, with possible complications, yet it fortunately works very well in the majority of patients.
7. FHO
FHO (Femoral Head Ostectomy) is used to treat hip dislocations or hip dysplasia.
The “ball” of the hip (femoral head) is removed during surgery.
FHO is also done in pets with a hip fracture or deterioration of the bone (e.g. Legg Perthes disease in small dogs).
8. Laryngeal paralysis
Dogs, mostly Labs, can have a condition that paralyzes their larynx, a.k.a. voice box, and causes them to suffocate. It’s an incredibly stressful condition. Fortunately, surgery (a “tie back”) allows them to have a wider airway, which typically works very well. These patients quickly go from suffocating to being able to breathe comfortably.
You can read about the amazing story of Mae Mae here:
9. Brachycephalic syndrome
This condition is seen in dogs (and rarely cats) with a flat face, which caused snoring and difficulty breathing: Bulldogs, pugs, Boston terriers, Persian cats etc.
It typically involves 4 conditions:
. The most visible part are stenotic nares (aka tiny nostrils) which prevents getting enough oxygen. Surgery involved making them wider, aka “a nose job” or a rhinoplasty.
. An elongated soft palate. The tip of the roof of the mouth is so long, that it covers the entrance of the windpipe. When it vibrates, it causes snoring. We can shorten it during surgery.
. Saccules are fleshy structures at the beginning of the windpipe. Over time, the saccules can pop out into the airway – and further block the flow of oxygen. We can remove them during surgery.
. A tiny windpipe, which we can’t do anything about.
You can read more about this surgery done on Kasper here:
https://www.drphilzeltzman.com/blog/guess-who-had-a-nose-job-today/
10. Reconstructive surgery
We did multiple surgeries that required reconstructing a body part:
. Cleft palate (or roof of the mouth), which you can read more about here:
https://www.drphilzeltzman.com/blog/squirrel-gets-a-new-lease-on-life-after-cleft-palate-surgery/
. Male cats who could not pee (P/U or perineal urethrostomy).
. A dog’s penis which had a (benign) tumor.
. Hernias, which are a condition where an organ ends up where it shouldn’t be.
Remembering some of the surgeries we’ve performed in 2021 is also an opportunity to give credit to the wonderful vets, nurses, and pet owners who have been caring for them.
Until next time,
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

