Dr. Phil Zeltzman’s Blog
Grandpa Charlie has successful heart surgery
Charlie, a roughly 12 year old Yorkie, just wasn’t himself. His appetite was poor. His breathing was faster than normal.
His owner recalls: “Charlie lives to eat so I knew something was wrong when I couldn’t even tempt him to eat tuna!”
Blood work was fairly normal except for high sugar levels – nothing new since Charlie was a known diabetic.
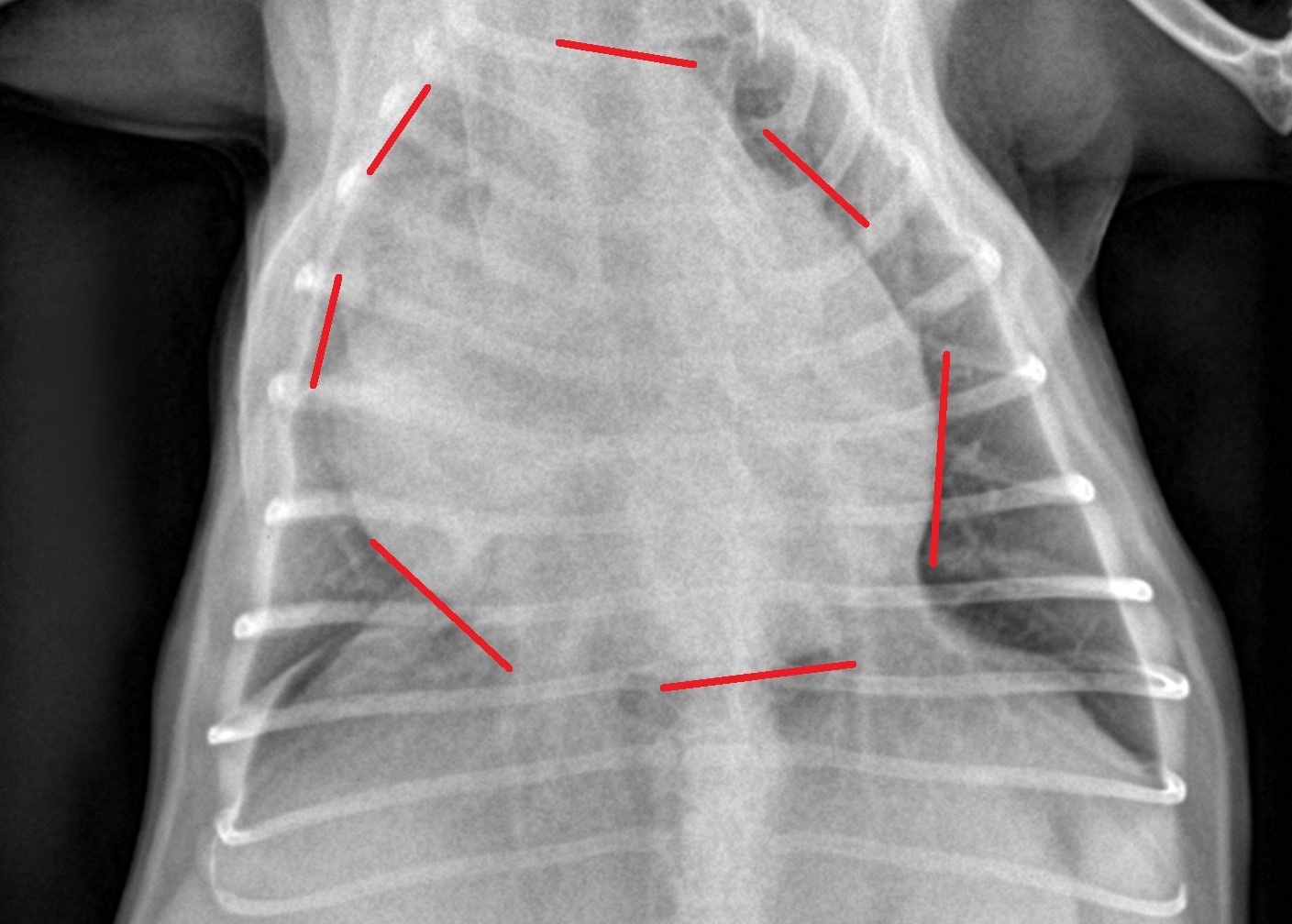
Chest X-rays showed an enlarged heart.
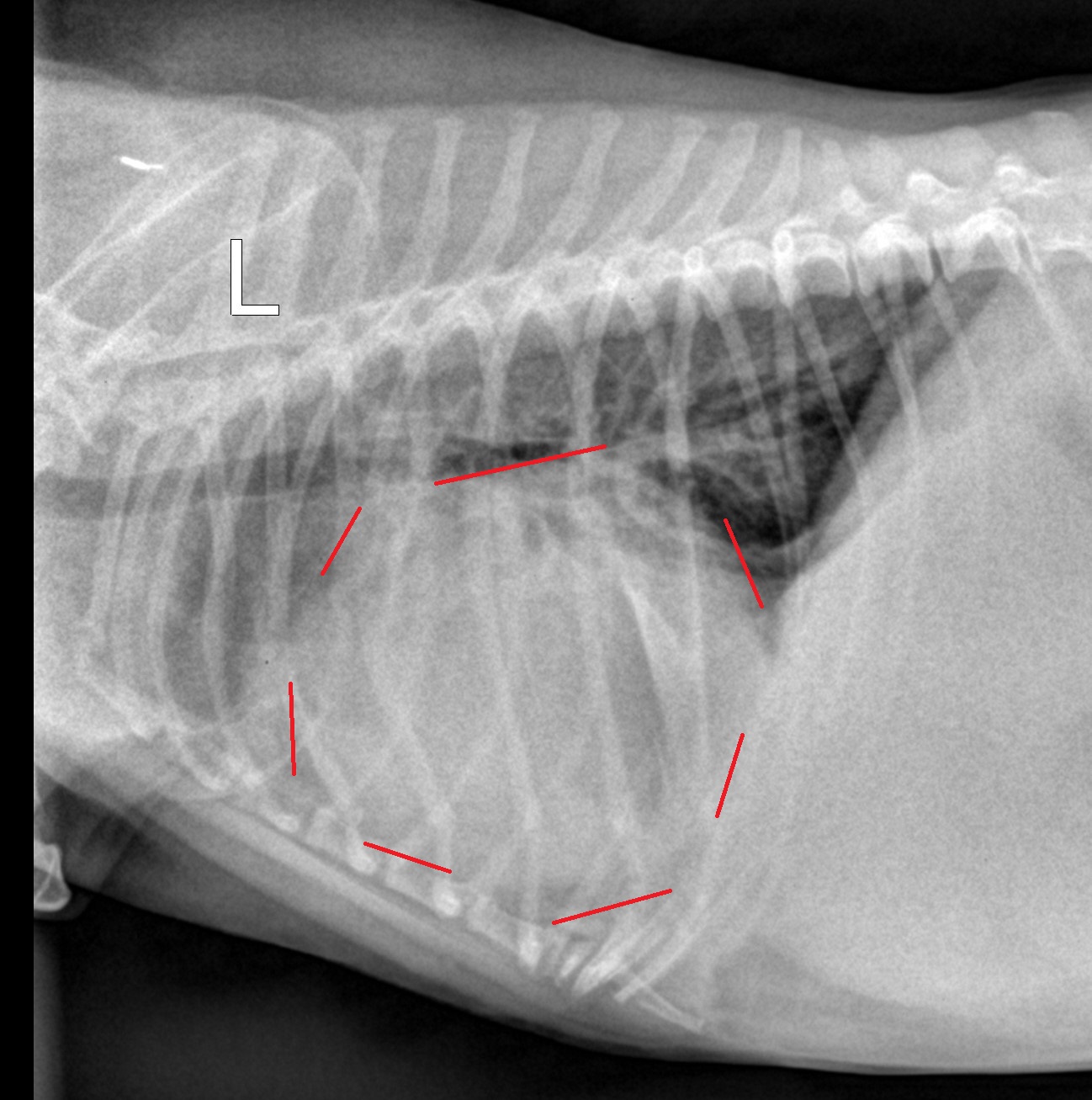
An ultrasound showed fluid around the heart. It also was suspicious for a tumor on the heart.
This is a pretty classic case of pericardial effusion.
What does that mean exactly?
The heart is covered by a sac called the peri-cardium (latin for “around the heart”). Its job is to protect and lubricate the heart, and to keep it in place within the chest.
Because this kind of tumor is fragile and very rich in blood vessels, it doesn’t take much for it to bleed.
Since the tumor is located inside the sac – the pericardium – blood builds up inside of it.
And because the sac can only expand so much, the fluid build-up eventually puts pressure on the heart.
Think of it as a bad headache or a migraine. The brain can only swell so much because of the skull around it.
This explained that Charlie didn’t feel well (poor appetite) and was out of breath.
Not only was the heart feeling squeezed, but the lungs had less room to expand.
The best solution is surgery, to relieve the pressure.
Anesthesia in a 12 year old diabetic dog with a sick heart is not exactly the safest thing to do.
I went over the pros and cons of surgery with Charlie’s owner.
Who on earth chooses surgery in such an old, sick little dog?
There was no doubt in his owner’s mind that it was the right thing to do.
She believes: “Once you take on the commitment of owning an animal, they become part of your family. (Despite) the bleak prognosis, we can’t willingly say goodbye to our beloved pet. (…) Even though he may only live a year (or less) or two years more, we feel we must do all we can to prolong his life.”
And she very kindly shared: “Honestly, I felt very reassured by your discussions with me prior to surgery. You clearly laid out postop care. I felt calm the day of surgery knowing Charlie was in good hands.”
Equipped with such positive vibes, and despite the risks, we took Charlie to surgery.
After an incision on the left side of his chest, between two ribs, a large section of the pericardium was removed.
ASSUMING YOU HAVE THE STOMACH FOR IT, you can watch the short video below.
As my wonderful nurses can attest, watching a beating heart is one of the coolest things we see, but I understand it is certainly not for everybody!
Before removal of the pericardium, the heartbeat is typically harder to see, because the heart is surrounded by the pericardium and lots of blood. In this video, that is not really the case, because a lot of the blood inside the sac had been removed with a needle to provide relief to Charlie.
After removal of the pericardium, a surgery called a peri-cardectomy, the heartbeat is easier to see, because there is nothing restricting it anymore.
We then needed a way to remove free air from the chest. This is done with a device called a chest tube. You can see a glimpse of it at the end of the video, on the left side of Charlie’s body. It only stays in place for a short time after surgery, and can be removed once there is no more air and not too much fluid left to remove.
After the chest tube was secured, the rest of the chest was stitched up.
Then it was time to transition from the OR to ICU.
Little Grandpa Charlie recovered from surgery and anesthesia very smoothly.
In fact, minutes after coming out of the OR, he looked surprisingly good and comfortable. I was so impressed, that I took a video of him (see link above). Of course, he’s in a daze because he went through a lot and he was high on doggy morphine, but he still looked amazing so soon after surgery!
This is a great testament to the wonderful anesthesia nurse who took care of Charlie. Anesthesia is always a bit more challenging when we do open chest surgery, especially in a patient with a compromised heart.
Even more encouraging, Charlie ate dinner the evening of surgery, for the first time in days!
Who eats a few hours after open chest surgery?!
The chest tube was removed the very next day.
After a few days on heavy duty pain medications and lots of TLC, he was able to safely go home.
His owner remembers: “I didn’t see Charlie for several days after surgery. When Charlie did come home, he had the cone on, but he seemed to almost be his old self. He didn’t seem like he was in pain (we gave pain meds anyway!). He ate and drank fine. When going potty, he was eager to do more, wanting to get back to his walks – though we said not yet!”
Charlie is very lucky his owner didn’t procrastinate and trusted her guts based on what were after all (seemingly) very minor signs.
Remember, all there was is a decreased appetite and faster breathing, that’s it!
She recalls: “I just had a bad feeling and knew things weren’t good. He just wasn’t acting like himself and I worried he was in pain.”
It’s only been 2 months since surgery, but so far Charlie is doing great.
His owner writes: “Charlie is doing marvelously well! He is eating, drinking and has a happy demeanor. He seems comfy and happy! Overall, the experience went very well and all of our fears have been alleviated. We have our energetic Yorkshire Terrier back!
And her final words of wisdom:
“The day will come when we won’t have a choice anymore and we will have to say goodbye. But for now, and thanks also to you, that day is not today. Some beings and their life/memories with us are more important than $!”
If you would like to learn more about how your pet can have safe surgery and anesthesia, contact us through www.DrPhilZeltzman.com
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

