Dr. Phil Zeltzman’s Blog
Ninja, my biggest surgical & ethical challenge in 2021
“I beg you for help.”
Such was the subject line of the email.

In the email, a pet owner explained:
“My dog Ninja, a 6 year old Siberian Husky, just had a CAT scan, then surgery to drain a cyst in his enlarged prostate” (17 cm long – about 7 inches).
“Because of the pressure on the colon and the bladder, Ninja couldn’t defecate or urinate!”
“His bladder has been so over-stretched, that it couldn’t contract and now Ninja still can’t urinate. A urinary catheter was placed temporarily… and the only option the surgeon gave us was euthanasia!”
“I don’t want to put him down. He is eating, drinking and (now) pooping. He acts normal but can’t pee. Please help me, I am very desperate.”
Desperate times call for desperate measures.
Ninja had a condition similar to unfortunate older gentlemen who struggle to pee because of an enlarged prostate. It is a frustrating & painful situation. But in a dog, it can be life-threatening.
There is a better solution than euthanasia. I suggested a surgery that involves placing a special tube in the bladder and allows draining the bladder on demand.
It’s certainly not for every pet owner, but Ninja’s owners were exactly the right people for the challenge: dedicated, attentive, and totally in tune with their dog. They had done their homework and found out about this option by reading my blog about Madeline, who had the same surgery for a different problem (a bladder tumor).
Chapter 1
Time was of the essence, so we quickly scheduled surgery at Brodheadvsille Vet Clinic.
Ninja had a “cystostomy” surgery, where a tube was placed to drain the bladder through an opening in the skin.
In addition, Ninja was neutered. After that necessary step, male hormones would decrease and cause the prostate to shrink. That would reduce the pressure on the urethra and allow Ninja to urinate.
Chapter 2
Everything went according to plan for about a month… until Ninja accidentally stepped on the tube.
The logical next step was to replace the life-saving drain. Unfortunately, preop bloodwork showed some concerning changes. Ninja’s immune system was attacking his own red blood cells (hemolytic anemia) and platelets (thrombocytopenia). This double condition is called Evans’ syndrome.
So we changed plans. Since it was too risky to perform surgery with such low numbers of red blood cells and platelets, we placed a traditional urinary catheter to allow Ninja to urinate.
We were able to do this thanks to the generosity of another practice owner near Allentown, PA.
The catheter had to be changed frequently to lower the risk of bladder infection (UTI).
His faithful owners would drain the bladder multiple times a day to allow it to stay small. Remember, the bladder was so over-stretched, that it couldn’t contract anymore…

Chapter 3
At that point, Ninja was referred to a board-certified internist (a medicine specialist) to manage his Evans syndrome.
Meanwhile, Ninja still couldn’t pee!
To make matters worse, an ultrasound showed that the prostate now had an abscess. Again, euthanasia was recommended.
Again, his owner called me to see if there were any other options.
After reaching out to multiple specialists, we found one willing to help. My amazing nurse and I suggested a completely crazy plan:
. An ICU specialist at a specialty hospital in NJ accepted to let us use the key to our problem: a special transfusion with platelets to help with clotting.
. We would drain the abscess at another practice in NJ, and place a new cystostomy tube to allow Ninja to pee.
. We would recover Ninja under the supervision the ICU specialist.
Amazingly, Ninja’s owners decided to go with surgery, about 2 months after the first one.
The procedure was uneventful, and after 2 days in ICU, Ninja went home.
Then came weeks and months of amazing dedication from Ninja’s owners.
Long story short, Ninja progressively got better and stronger.
Then out of the blue, to everybody’s surprise, he started to pee on his own!
After agonizing over the right time to remove the tube, we eventually did, once we were convinced that Ninja was emptying his bladder on his own sufficiently to survive.
Now you understand why Ninja was such a technical and mostly ethical dilemma for me.
When should a surgeon stop helping?
When should a pet owner stop hoping?
When should a pet to cross the rainbow bridge?
Why did I choose Ninja’s story…
… over so many other amazing pet stories I was fortunate to play a part in in 2021?
Because of the number of people who played a role in Ninja’s survival.
In the middle of the COVID crisis, it was an absolutely astonishing display of generosity, love and care, by multiple vets and nurses.
Across half a dozen practices.
And across 2 States (PA & NJ).
(trust me, I gave you the short version!!!)
Everybody rallied behind Ninja, led by his loving owners.
And the result is one happy, playful, fluffy Husky, whose only wish is to be comfortable, to be able to pee, and to return his owners’ love.
Ninja’s owner created an amazing video summary.
It’s a story about the love of a family pet.
A story about the power of dedication.
A story about not taking no for an answer.
You can watch it here: https://vm.tiktok.com/ZMRatj6Co/
Fair warning: it’s a tiny bit emotional…
What’s the moral of the story?
1. Neutering early in life decreases or eliminates the chances of having prostate issues in male dogs. There are many other good reasons, which you can read about here:
https://www.drphilzeltzman.com/blog/top-10-reasons-to-neuter-your-pet/
2. You are your pet’s best advocate. If something makes no sense to you, don’t give up. Sadly, there is not a solution or a cure for every condition. But at least, you should explore your options.
Don’t take no for an answer. Get a second opinion.
This is exactly what Madeline’s and Ninja’s owners did. They didn’t take no for an answer, and they saved their dogs’ lives.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
How I got a chance to fix a baby coyote!
I recently had the unique opportunity to fix a 2 month old coyote baby!
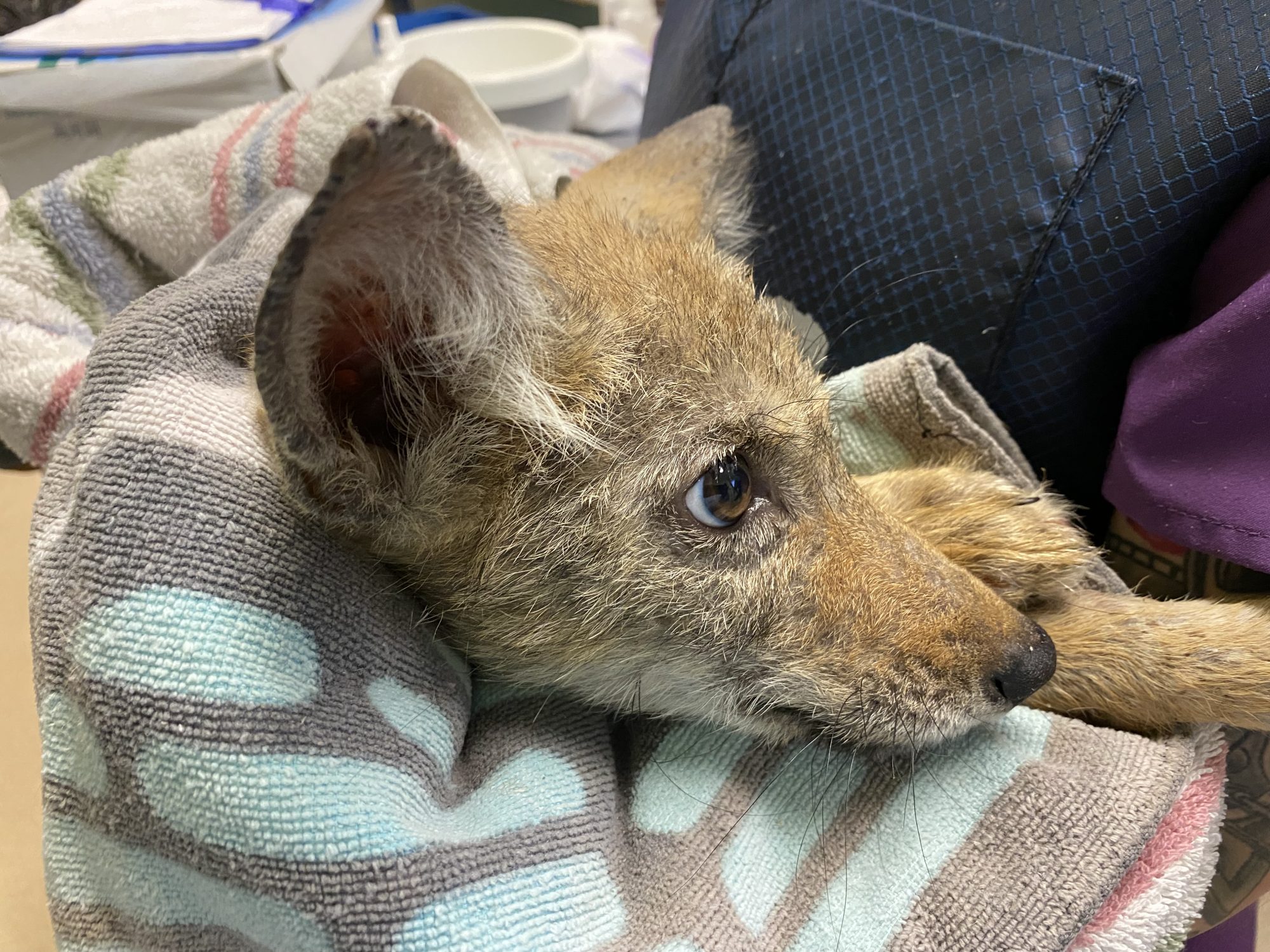
One of my referral clinics is heavily involved in wildlife rehab.
Mama coyote had been hit and killed by a car.
Her two orphans were eventually found.
One pup, promptly named Lukas, had sustained a fracture of the right humerus, the bone in the arm, which required surgery.
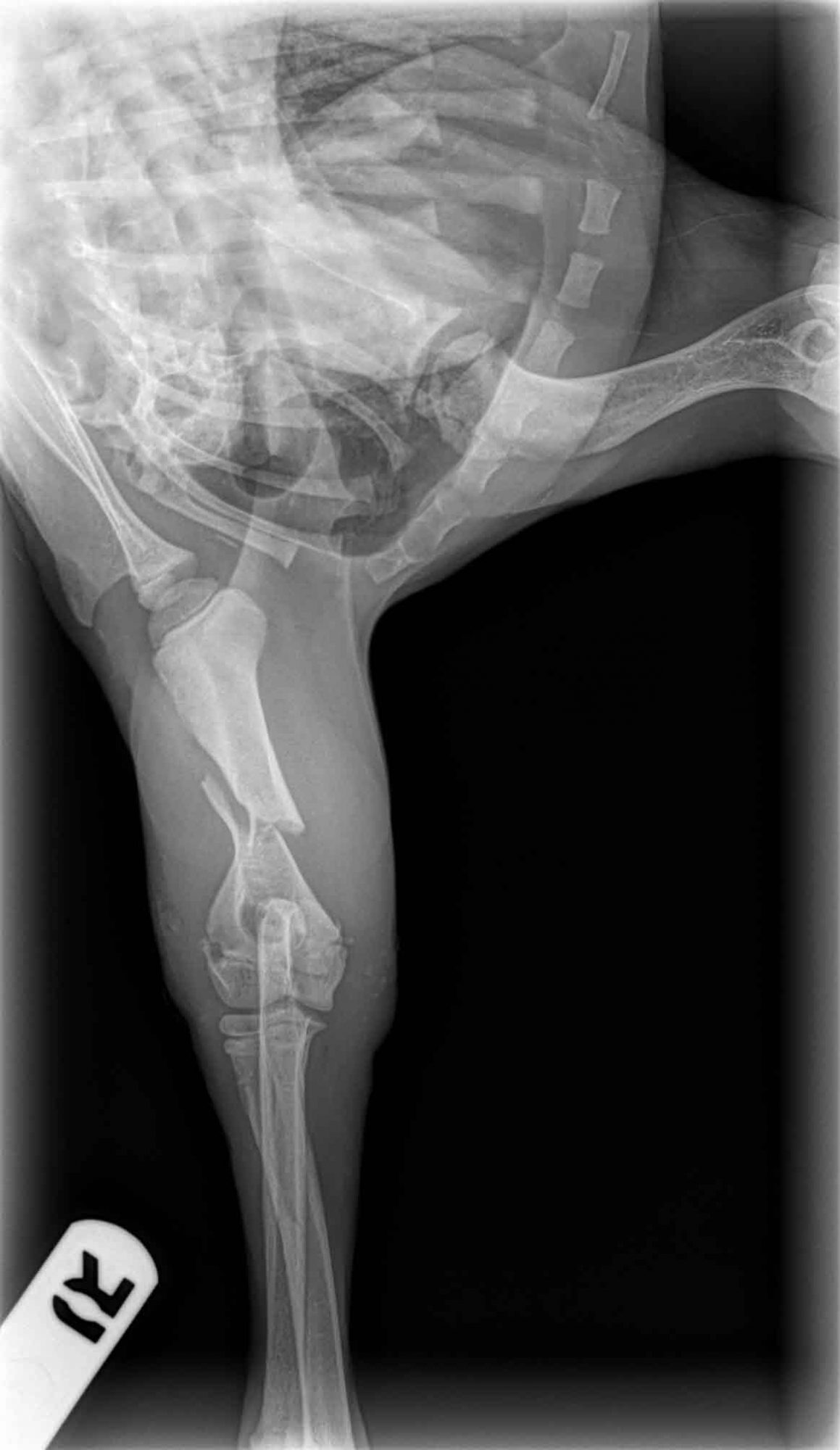
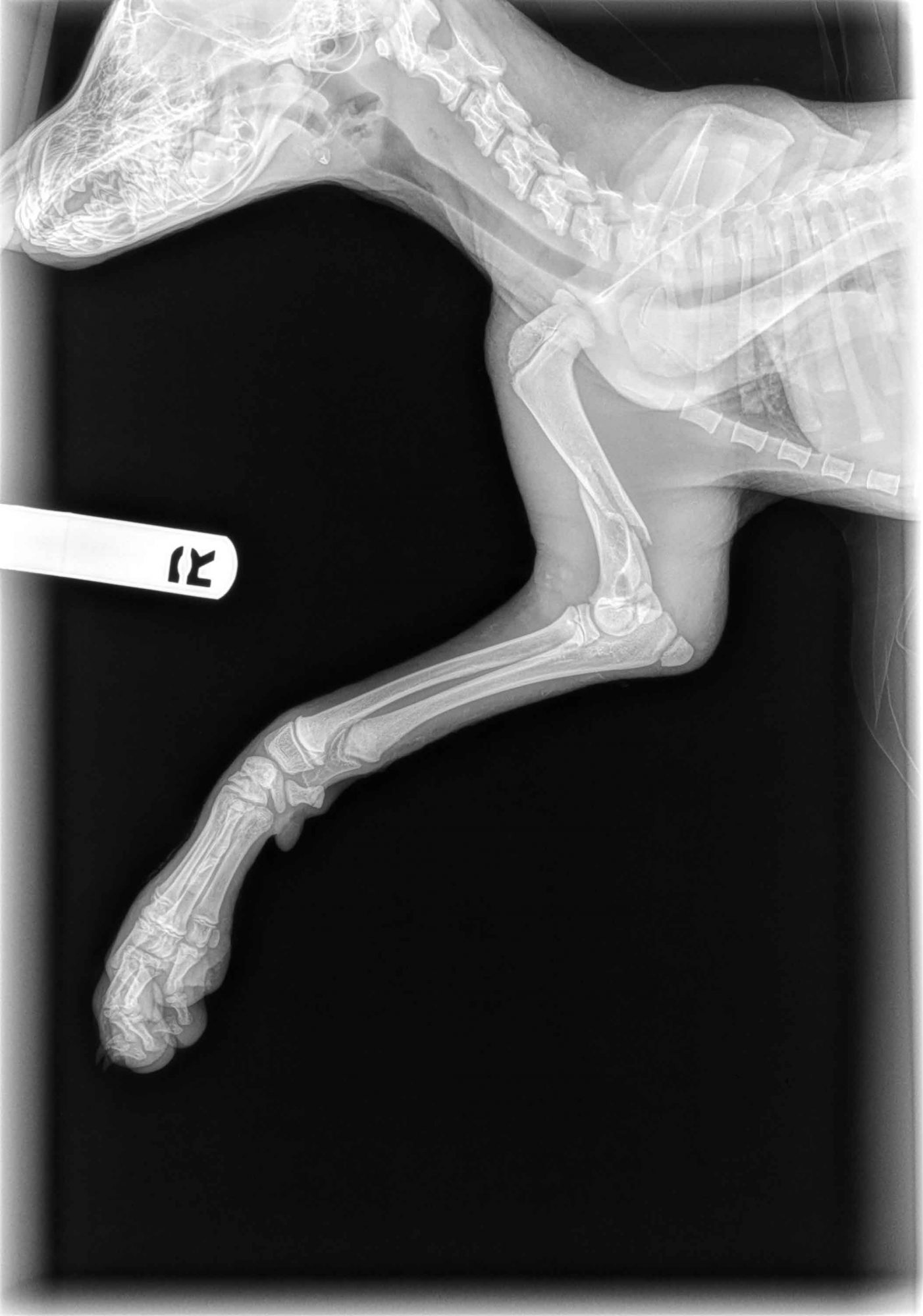
Preop blood work showed that he was healthy enough to undergo anesthesia.
There were 3 main risks to be aware of:
. Surgery is challenging because of puppies’ bones are soft, so they don’t hold screws very well.
. Pediatric patients who undergo anesthesia are at risk for hypoglycemia (low blood sugar), hypothermia (low temperature) and hypotension (low blood pressure).
. It’s much tougher to rehab a wild animal than a tamed house pet.
Fully understanding the risks, we put baby Lukas under anesthesia.

What we couldn’t know before doing surgery, since scar tissue is not visible on X-rays, is how old the fracture was. It turns out that it had been a while. And that makes sense: by the time the terrified pup was found, rescued, assessed, transferred to the vet clinic, and then transferred to my care, it had been many days.
Another proof that the fracture was old is that his range of motion was very poor, even under full anesthesia (my exam notes said “Poor range of motion preop: cannot flex elbow beyond 45 degrees”).
My surgery report said “TONS of scar tissue… very difficult to recognize the anatomy of the bone.”
So we did what we could: stabilize the fracture the best we could, since lining up the bone was not possible. The result is not pretty on X-rays, but functional…
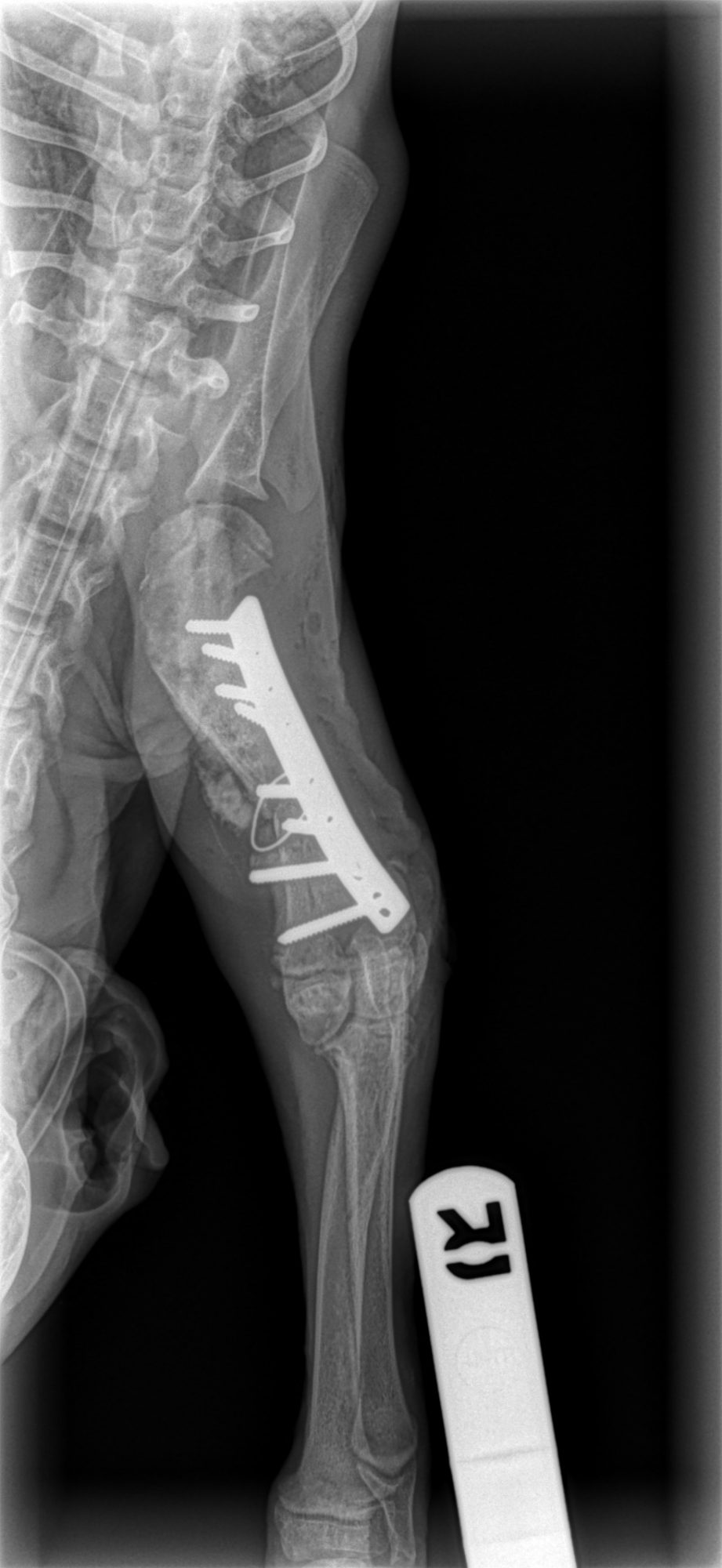
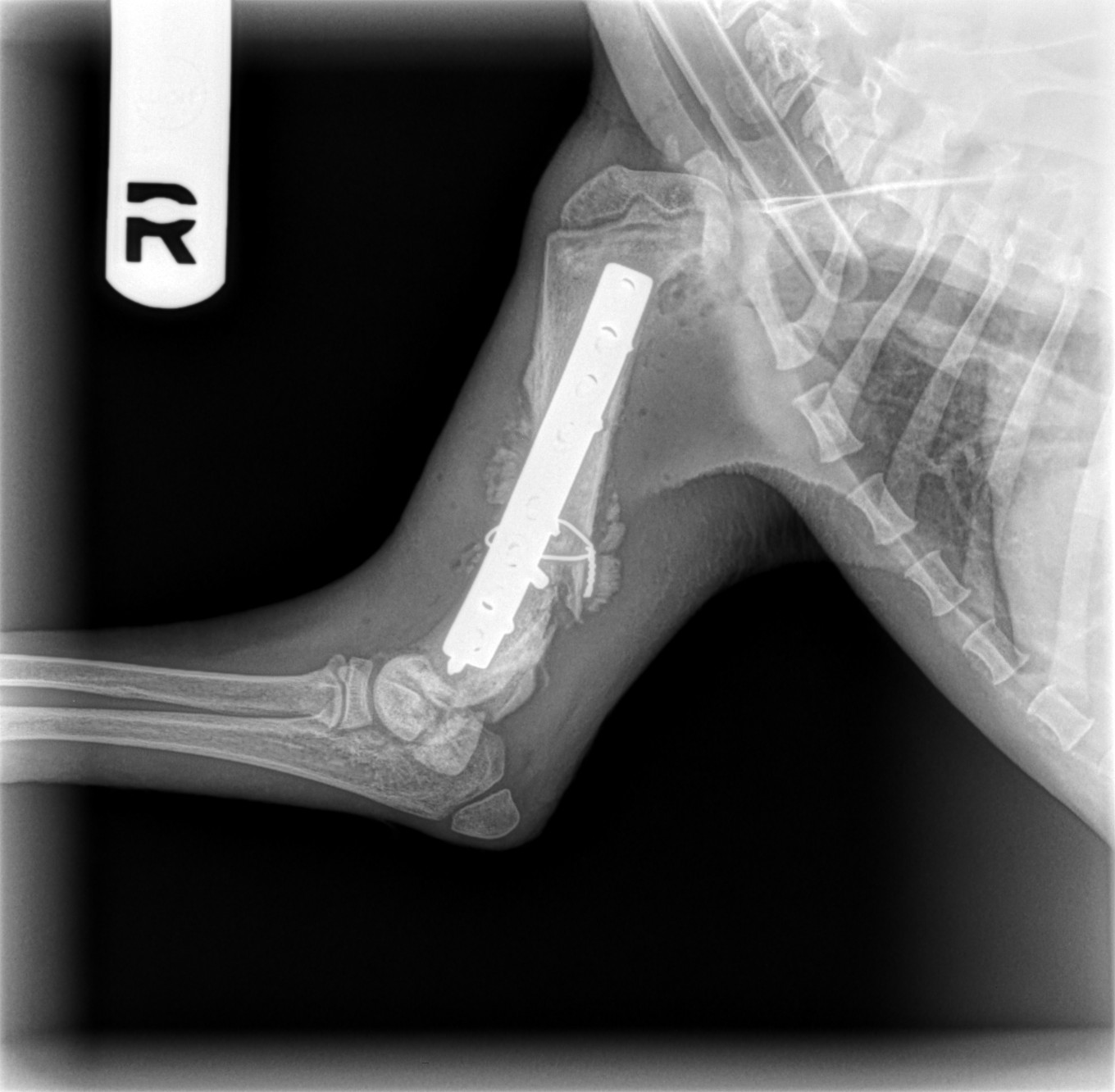
A stainless steel plate and 8 screws were placed.
Fortunately, Lukas recovered smoothly from anesthesia.

Despite the above challenges, the benefit of being young is that bones heal very quickly.
The next challenge was to allow Lukas to heal, confined in a small area, fed a healthy diet, while doing physical therapy so his elbow wouldn’t get too stiff.
All of that, while handling him as little as possible. It is very detrimental to overhandle wildlife, especially pediatrics, due to the risk of human imprinting.
Imprinting refers to a critical time in young animals when they form attachments and develop their identity. So they need to “imprint” onto their mother, or their siblings, or their buddies, not humans.
To avoid this risk, Lukas was eventually transferred to a rescue association.
Once fully healed based on 6 week X-rays, Lukas was reunited with his brother. They were kept at the rescue until they were 6 months old. Then they were released together, to live their coyote lives…
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Matilda and the amazing bladder stones
Matilda, a 12 year old Lab, had difficulty urinating, frequent urination and blood in the urine.

A physical exam and X-rays at her family vet revealed that her bladder was literally full of stones!
This is a serious condition, but it was reassuring that she did not have a bladder tumor, which could cause the same signs.
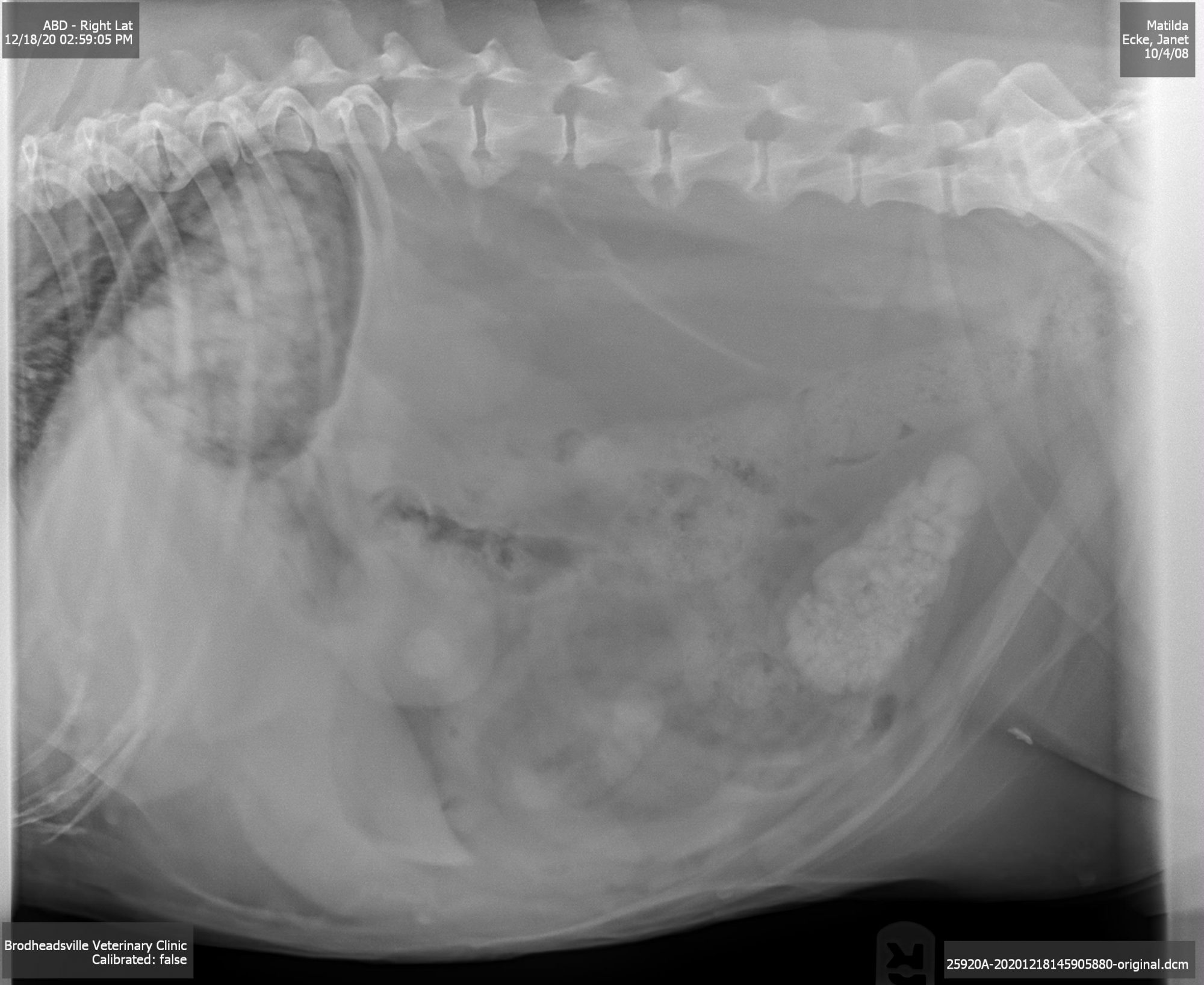
The solution to remove Matilda’s stones was bladder surgery (please note that what follows pretty much also applies to male dogs and cats, as well as female cats).
Blood work was normal, including kidney values, which confirmed that Matilda was a good candidate for anesthesia.
The surgery is called a cystotomy. An incision is made in the belly, then into the bladder. The stones were then physically removed.
Here is a very short video showing removal of the bladder stones – BUT PLEASE BE AWARE THAT IT IS A BIT GRAPHIC AND NOT FOR THE FAINT OF HEART!!!
Removing the stones is the easy part. The sometimes tricky part is to remove stones that may have gone down the urethra (i.e. the tube between the bladder and the outside world). Stones can get stuck there and cause a blockage, preventing a pet to pee.
In males, another surgery is occasionally needed to create a new opening to allow peeing (this is called a urethrostomy).
Two tests are routinely sent to the lab:
. A stone analysis. The goal is to figure out which minerals the stones are made of. This is critical for vets to recommend the proper diet to prevent the stones from coming back.
. A culture. This is a sterile swab to determine if a bladder infection (UTI) might be the cause for the bladder stones – or a consequence. This is also a critical test to choose the proper antibiotic to take care of the infection.

This is all the stones we removed!
Once the bladder is all cleaned out, it can then be stitched up, as well as the belly. Recovery is typically 3-4 weeks.
Interestingly, bladder surgery patients can continue to experience the same urinary symptoms postop as before surgery – for different reasons:
. frequent urination, because the bladder is irritated and things feel weird “inside.”
. blood in the urine, because the bladder is very rich in blood vessels, and the bladder just had an incision.
These signs can last a week or two.
Matilda went home the next day, with antibiotics and 2 pain medications. She was progressively switched to a special food over 10 days.
A week later, the culture results showed that the antibiotic had to be changed. And 3 weeks later, the stone analysis confirmed that she was on the proper diet.
Committing to using the special food exclusively – for life – is extremely important. Bladder stones are formed because of an imbalance between minerals (most commonly calcium or magnesium), or a change in the pH of the urine.
So giving the special food for a few months, then going back to the old food, usually to save money, is a recipe for failure. Likewise, giving people food or treats may sound like a generous and loving idea, but you might recreate the imbalance between minerals and can be enough to cause more bladder stones… which means the poor dog may need another surgery.
Surgical removal of bladder stones is the most efficient way to address this condition. It also may be the only option when the urethra is blocked by a stone (urethral obstructions), which is a life-threatening emergency.
After 4 weeks of rest, Matilda was allowed to progressively return to her normal life, couch surfing and chasing tennis balls.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
You won’t believe what I removed from Daisy’s head!
Daisy, a 1 year pitbull, was found as a stray in the woods. She had wounds on her face and body, as well as an issue with her left eye. She had a hard time opening her jaw. Here is a picture of her head while under anesthesia.
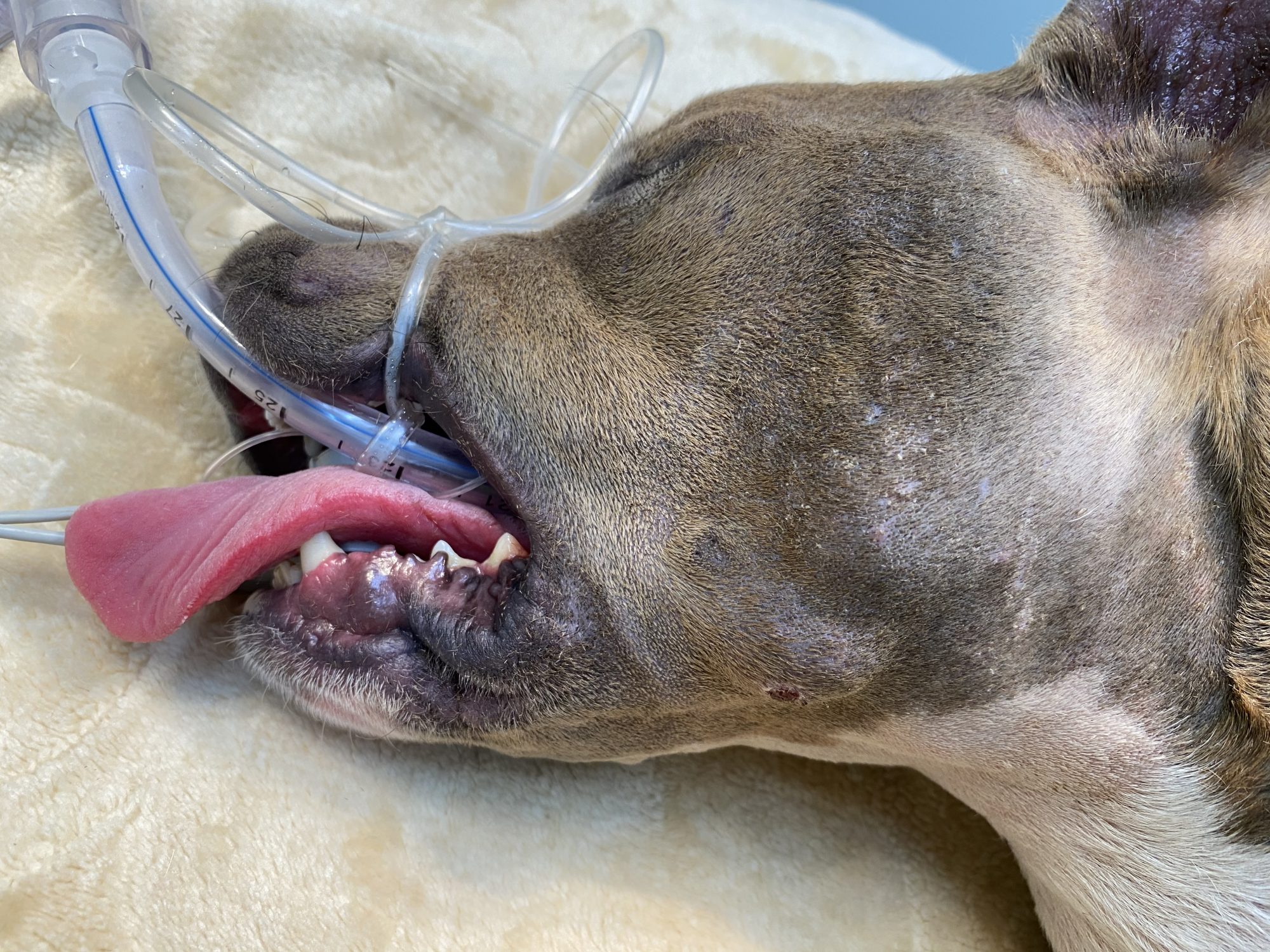
She was taken to her family vet for medical care. A physical exam revealed a large, firm swelling on her lower left cheek. The mass was draining.
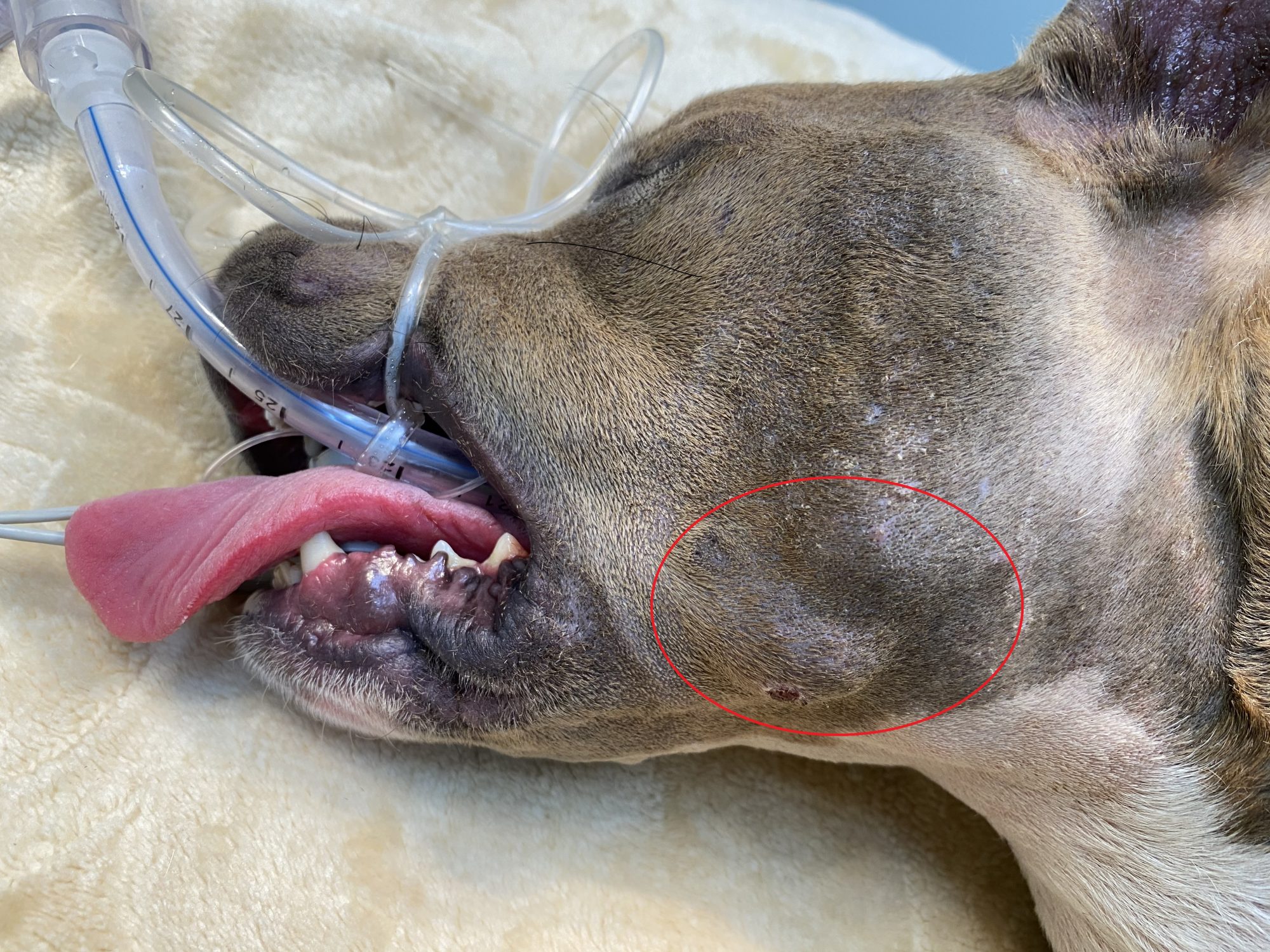
To be safe, the vet wisely decided to take some X-rays to see what was going on inside. To everyone’s amazement, Daisy had a huge nail inside her head!
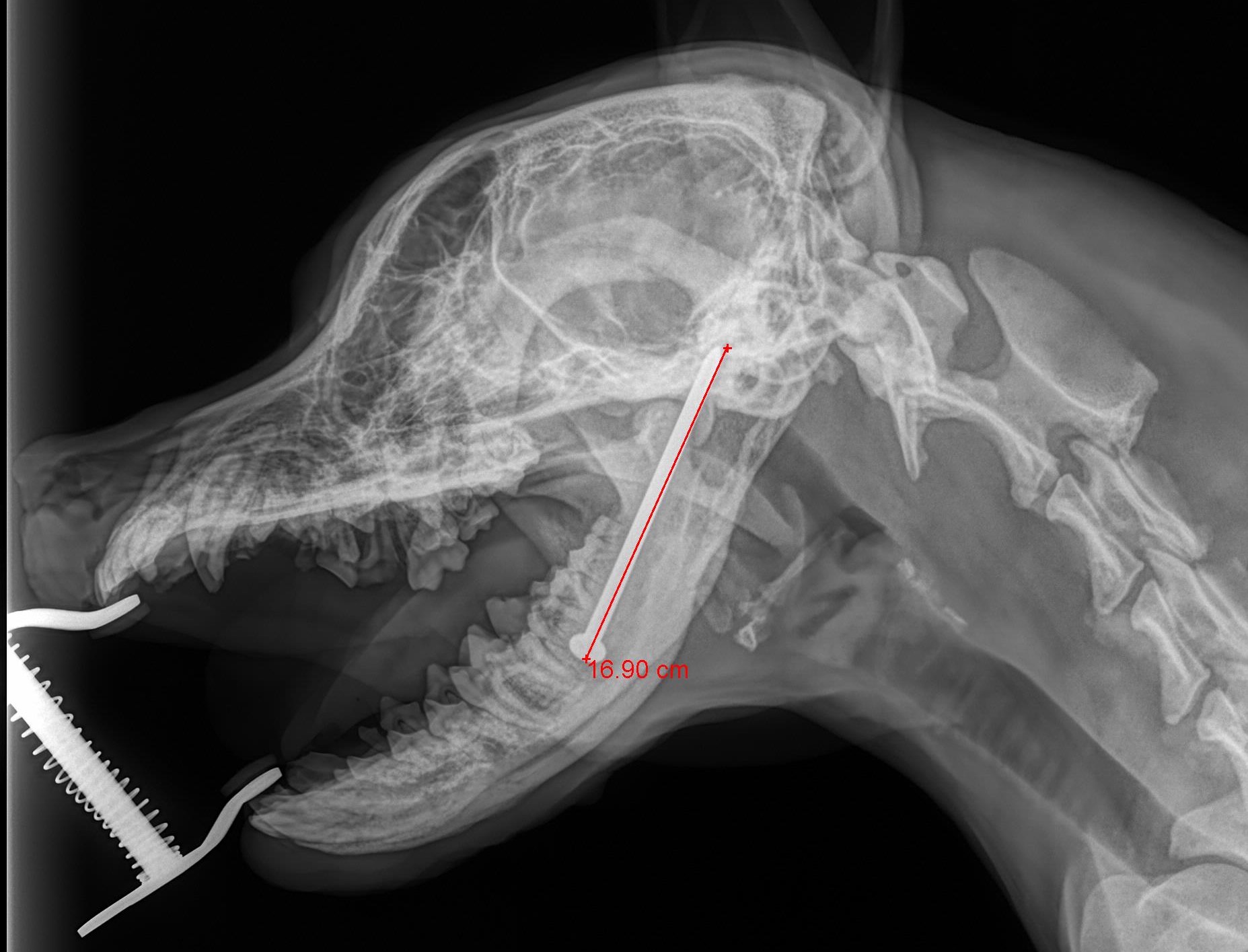
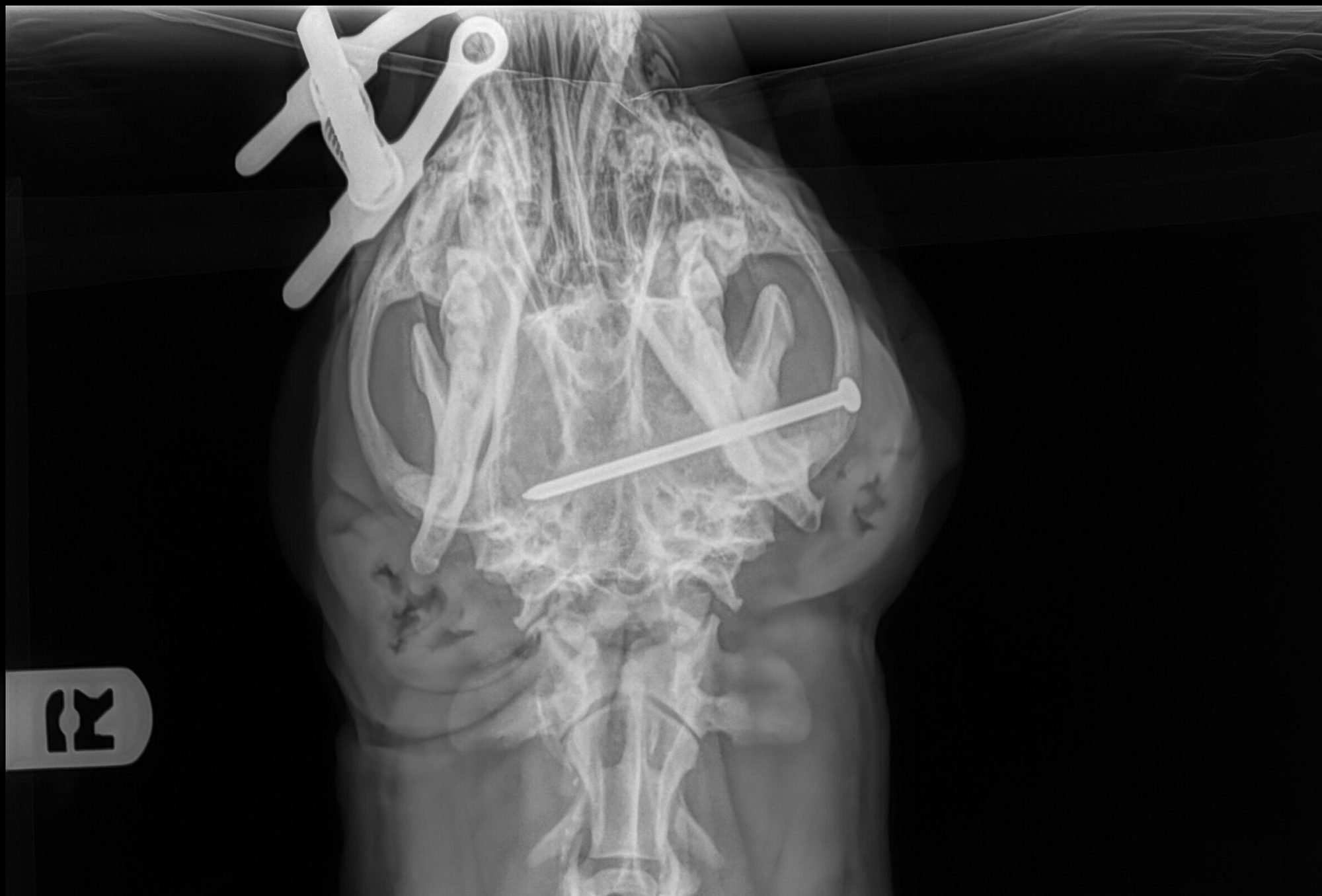
At this point, the vet contacted me regarding surgery to remove the nail.
We were able to fit Daisy in our schedule the very next day. This couldn’t wait!
There were multiple unanswered questions: How complicated would the surgery be? How was the nail involved with the jaw bone? How about the eye?
Luckily for Daisy, the surgery turned out to be simpler than anybody thought. I made an incision over the firm lump on her cheek. Once we found the nail head, I grabbed it with an instrument and gently pulled, and pulled, and pulled.
Here is the amazing, very short video showing removal of the nail – BUT PLEASE BE AWARE THAT IT IS A BIT GRAPHIC AND NOT FOR THE FAINT OF HEART!!!
Link to https://youtu.be/bjccCGAjXXk
After surgery, we measured the nail at a whopping 3.5 inches long (9 cm). That’s more than half the width of this poor Daisy’s face! She recovered smoothly from anesthesia.
Her treatment nurse commented: “Daisy did very well after surgery. She was comfortably standing up in her run. Her vitals are normal. She can safely go home.”
So Daisy was sent to her new home, where she will hopefully live happily ever after.
Her new owner shared the following observations:
“Before surgery, she had this bizarre howl/growl/squeal. She now has a real bark.
Before, she couldn’t fully open her mouth. She can now, and she’s eating well.
She is acting like a real puppy. So happy! She is almost smiling!
She acts like a NEW dog today.
Thank you again!!!!!!!!!!!”
No one knows how Daisy ended up in the woods. Nobody knows what tragic events happened prior to her discovery. And certainly, no one knows how she ended up with a giant nail in her head!
She is lucky to have found such a generous soul, so willing to adopt her and care for her.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Who on earth wants surgery on their 23 year old cat?
I recently repaired a fracture on a 23 year old cat. Some of my nurses aren’t even that old! It’s a true story with a very happy ending.
Basil, the 23 year old cat, had a broken tibia. The shin bone was broken in 3 main pieces. He went to the local ER, where his owner was told that he was too old and should be put to sleep.

That did not sit well with Basil’s owner. He may be 23 years old, but he was healthy otherwise, so why end his life? His owner contacted me regarding Basil’s situation. We agreed that it was ethical to perform surgery on him, since he was healthy otherwise, and we scheduled him for surgery.
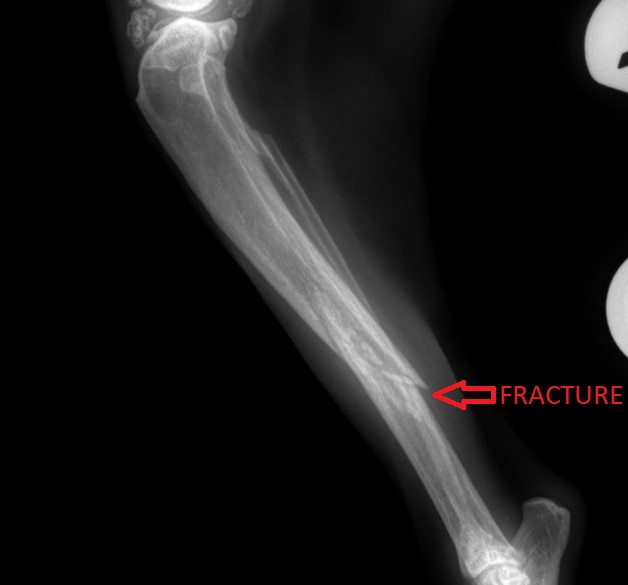
Fixing the shattered bone required 1 pin, 1 plate, 4 wires, and 9 screws to repair! A bone graft was added to speed up healing. Surgery went well and sweet Basil recovered smoothly under the close supervision of his nurses.
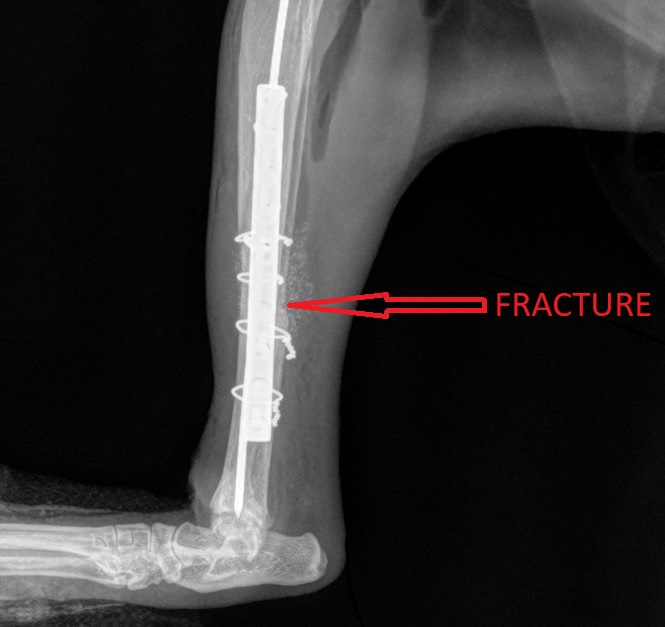
At home, he was strictly confined for 8 weeks. At suture removal, after only 2 weeks, he surprised everybody by walking around using the leg very well.
And after 8 weeks, follow up X-rays showed that the bone had healed nicely and we could start to increase Basil’s activity.
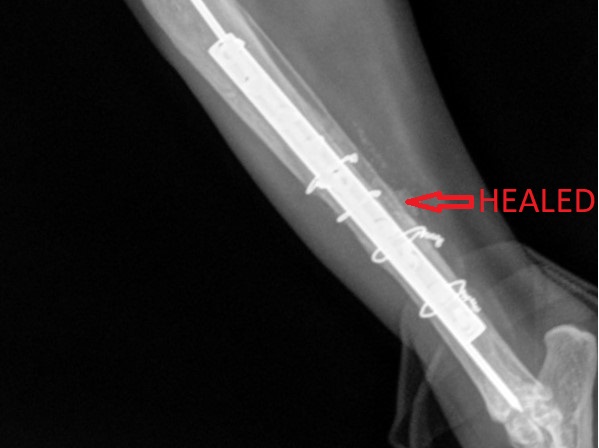
And after one more month of that, Basil returned to his normal Grandpa life.
So what’s the moral of this story?
As I always say, “Age is not a disease.”
A few conditions need to be met for surgery to be a valid option in my opinion:
. The patient should be reasonably healthy
. The condition should be fixable.
. Quality of life should be good after surgery.
. The owner should be 100% on board.
Two months after surgery, Basil’s owner writes: “My sweet 23 year old cat is finally back on the couch with me. He is getting giant hugs. He’s really doing great. I really have no words to thank you enough.”
I don’t see why we should deny help to a patient who fulfills these criteria.
Basil’s owner certainly felt that way, and I am sure Basil did as well…
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

